Serology Fundamentals - Antibody Adventures
- Serology: Detects antigen-antibody (Ag-Ab) reactions in serum.
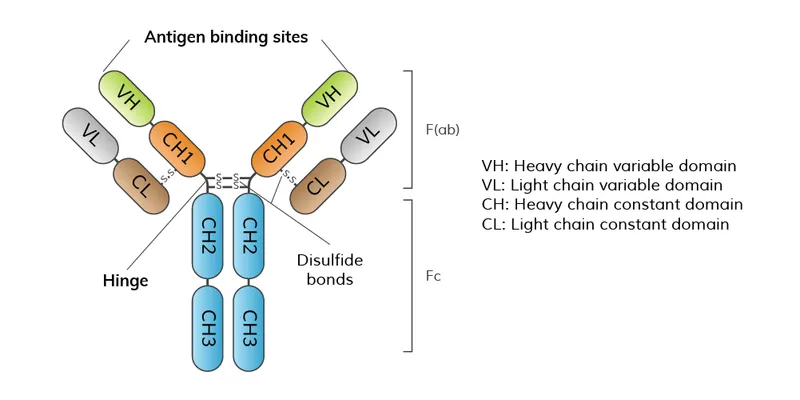
- Antibody (Immunoglobulin/Ig):
- Proteins from plasma cells; bind specific antigens.
- Structure: Y-shaped; 2H & 2L chains. Fab (Ag-binding), Fc.
- Classes: IgG, IgA, IgM, IgD, IgE (📌 GAMED).
- Antigen (Ag): Triggers immune response; epitope is binding site.
- Ag-Ab Reaction:
- Specificity: Unique Ag-Ab fit.
- Affinity: Single Ag-Ab bond strength.
- Avidity: Overall multiple bond strength.
⭐ IgM is the largest antibody (pentamer) and the first to appear in a primary immune response, indicating acute infection. 📌 M for Mega & M for iMMediate.
Classic Serological Tests - The Old Guard
- Precipitation: Soluble antigen + antibody → insoluble precipitate.
- Visible at optimal Ag-Ab ratio (zone of equivalence).
- Types: Ring (Ascoli's), Slide (VDRL), Immunodiffusion (Ouchterlony).
- Agglutination: Particulate antigen + antibody → visible clumping.
- Types: Slide (Widal-rapid), Tube (Widal-quantitative), Latex (ASO, CRP), Passive.
- Hemagglutination: Direct (blood groups), Indirect (Rose-Waaler for RF).
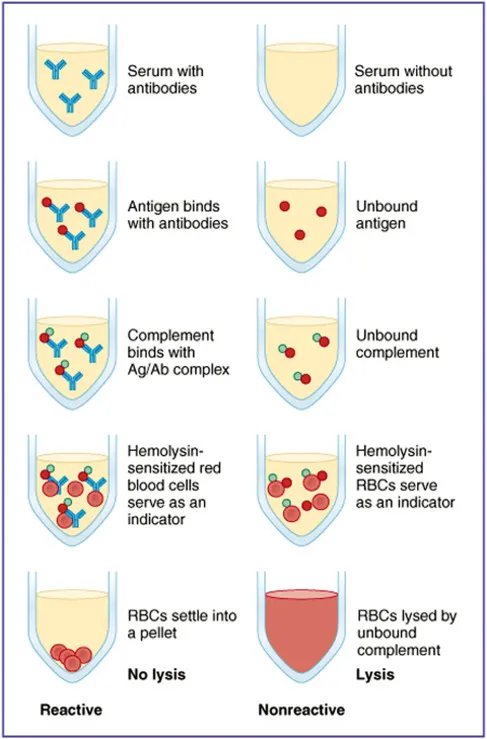
- Complement Fixation Test (CFT): Two-stage; detects Ag-Ab reaction by complement (C') consumption.
- Positive = No hemolysis (C' used); Negative = Hemolysis (C' free).
⭐ Prozone phenomenon: Excess antibody leads to false negative results in precipitation/agglutination tests; resolved by diluting the patient's serum.
Labeled Immunoassays - Tag, You're It!
-
Principle: Use labeled reactants (Abs or Ags) for sensitive detection of immune complexes.
-
Labels: Enzymes (ELISA), Fluorochromes (IFA), Chemiluminescent tags (CLIA), Radioisotopes (RIA - rare).
-
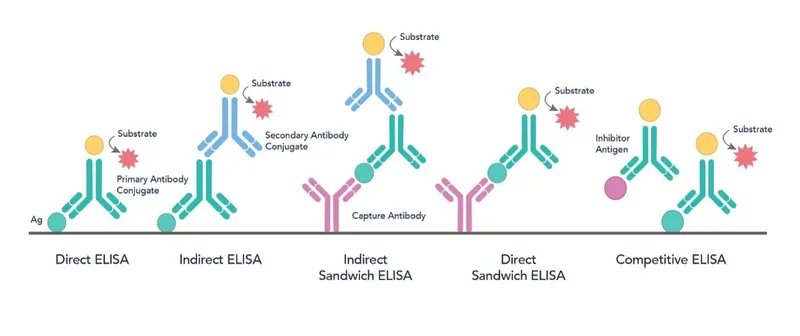
ELISA (Enzyme-Linked Immunosorbent Assay)
- Widely used; detects Ag or Ab.
- Types: Direct, Indirect, Sandwich, Competitive.
- Enzyme + Substrate → Signal (e.g., color).
⭐ Sandwich ELISA is common for Ag detection (e.g., HIV p24, HBsAg); Ag is 'sandwiched' between two Abs.
-
IFA (Immunofluorescence Assay)
- Uses fluorescent-labeled Abs.
- Direct (DIF): Labeled Ab on Ag in tissue.
- Indirect (IIF): Labeled secondary Ab detects primary Ab-Ag complex.
-
Western Blot (Immunoblot)
- Confirmatory (e.g., HIV). Proteins separated by size, then probed.
Clinical Application & Pitfalls - Detective Work
- Disease Diagnosis & Monitoring:
- HIV: ELISA (screening), Western Blot (confirmatory). Note window period.
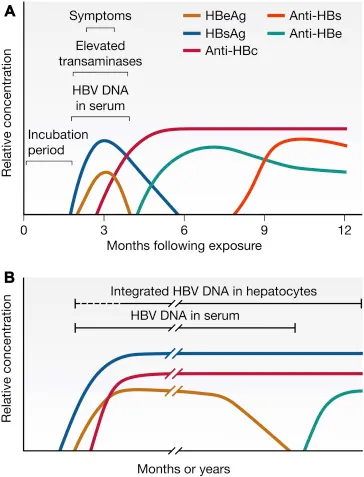
- Hepatitis (A,B,C,E): Specific antigen-antibody patterns define infection stage.
⭐ For Hepatitis B diagnosis, HBsAg indicates active infection, Anti-HBs indicates immunity (from vaccination or recovery), and Anti-HBc IgM indicates acute infection.
- Syphilis: Non-treponemal (VDRL/RPR - screening, titre monitoring); Treponemal (TPHA/FTA-ABS - confirmatory).
- TORCH Panel: IgM for acute infection; IgG for past exposure/immunity. IgG avidity differentiates recent vs. past.
- Interpreting Results:
- Paired Sera: ≥4-fold rise in antibody titre is diagnostic.
- Seroconversion: Appearance of antibodies after infection.
- Window Period: Time before antibodies are detectable.
- Pitfalls & Limitations:
- Cross-reactivity: e.g., biological false positives in VDRL (📌 Mnemonic: VDRL - Viruses, Drugs, Rheumatic fever, Rheumatoid arthritis, Leprosy, Lupus).
- Prozone Phenomenon: Excess antibody → false negative (agglutination tests).
- Immunodeficiency: May cause delayed or absent antibody response.
- False positives/negatives inherent to tests.
High‑Yield Points - ⚡ Biggest Takeaways
- Seroconversion (four-fold antibody rise) confirms acute infection.
- IgM indicates acute/recent infection; IgG suggests past exposure/immunity.
- Antigen detection (e.g., ELISA, rapid tests) enables early diagnosis.
- Agglutination tests (Widal, VDRL) detect antibody-antigen clumping.
- ELISA is highly sensitive/specific for infections like HIV, Hepatitis.
- Western blot is a confirmatory test (e.g., HIV), detecting specific proteins.
- Prozone phenomenon (excess antibody) causes false-negative agglutination; dilute serum to resolve.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more