Rapid Diagnostic Tests: The Basics - Speedy Sleuths
- Definition: Tests providing rapid results, often at or near the point of patient care.
- Principle: Typically detect microbial antigens, host antibodies, or microbial nucleic acids.
- Key Advantages:
- Speed (results often <30 mins to 2 hours)
- Ease of use (minimal training)
- Minimal equipment needs
- Point-of-care testing (POCT) suitability
- Limitations:
- Generally lower sensitivity/specificity compared to culture or PCR.
- Often qualitative (yes/no) or semi-quantitative.
- Potential for false positives/negatives; results need clinical correlation.
⭐ Key advantages of RDTs include speed (results often in <30 mins to 2 hours), ease of use, and minimal equipment needs, making them ideal for resource-limited settings and point-of-care testing.
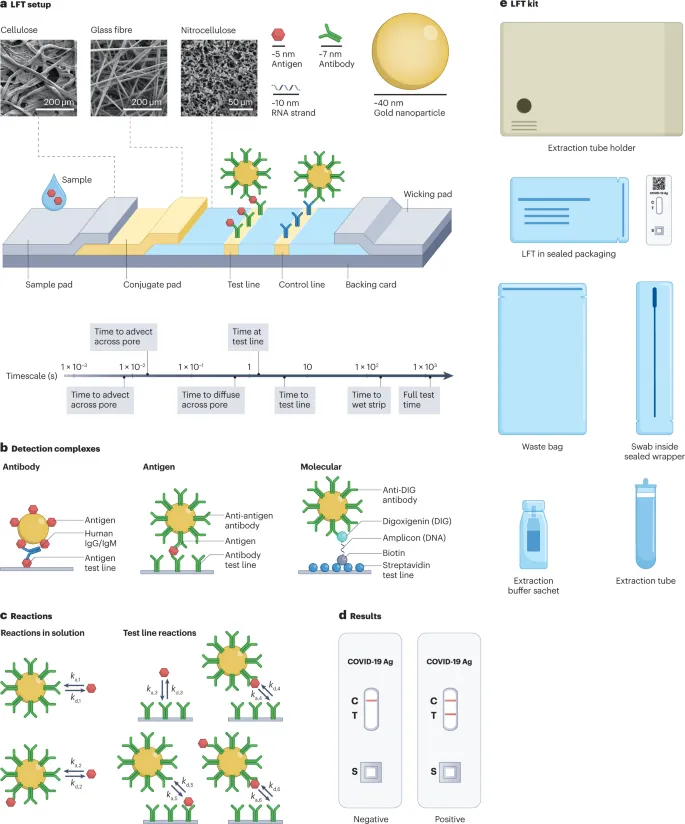
Rapid Diagnostic Tests: Immuno-RDTs - Antibody Avengers
- Immuno-RDTs: Detect microbial antigens (Ag) or host antibodies (Ab) swiftly.
- Lateral Flow Assays (LFAs): Most prevalent.
- Principle: Capillary action transports sample; specific Ag-Ab binding with colored particles (e.g., gold) creates visible lines.
- Strip: Sample pad → Conjugate pad (labeled Abs) → Nitrocellulose membrane (Test & Control lines) → Absorbent pad.
- Examples: Pregnancy (hCG), Malaria (HRP2, pLDH), Strep A, Dengue (NS1, IgM/IgG), HIV.

⭐ Most Lateral Flow Assays (LFAs) (e.g., pregnancy tests, malaria RDTs, Strep A) incorporate a control line to validate test strip integrity and proper sample flow; absence of control line invalidates the test.
Rapid Diagnostic Tests: Molecular & Other RDTs - Gene Genies & Quick Chems
- Molecular RDTs (Gene Genies): Detect pathogen-specific DNA/RNA.
- Nucleic Acid Amplification Tests (NAATs):
- PCR (Polymerase Chain Reaction): Amplifies target DNA.
- RT-PCR: For RNA targets (e.g., HIV, HCV, SARS-CoV-2).
- LAMP (Loop-mediated Isothermal Amplification): Rapid, isothermal, field use.
- Microarrays: Simultaneous detection of multiple genes/pathogens.
- NGS (Next-Generation Sequencing): Comprehensive analysis, outbreak investigation.
- Nucleic Acid Amplification Tests (NAATs):
- Other RDTs (Quick Chems):
- MALDI-TOF MS: Rapid ID of bacteria/fungi via protein profiling (minutes).
- Rapid Biochemical Tests: (e.g., API strips) for enzyme activity, metabolic profile.
⭐ CBNAAT (Cartridge-Based Nucleic Acid Amplification Test) like GeneXpert for MTB can detect M. tuberculosis and rifampicin resistance simultaneously from sputum within 2 hours, revolutionizing TB diagnosis.
Rapid Diagnostic Tests: RDTs in Action - Disease Detectives
- Immunochromatographic assays detecting specific antigens/antibodies.
- Point-of-care; results in ~15-30 min.
- Malaria:
- HRP2 for P. falciparum.
- pLDH for Pan-Plasmodium/species-specific.
- Dengue:
- NS1 Ag (early, 1-7 days).
- IgM/IgG Ab (later).
- HIV:
- Antibody detection (screening); confirmation needed.
- Tuberculosis (TB):
- Molecular: CBNAAT for M.tb & RIF resistance.
- Strep Throat:
- RADTs for Group A Strep (GAS) antigen.
- COVID-19:
- Antigen tests (active infection).
- Antibody tests (past exposure).
⭐ For Dengue diagnosis, NS1 antigen RDTs are useful in the early febrile phase (first 1-7 days), while IgM/IgG antibody tests become positive later in infection.
High‑Yield Points - ⚡ Biggest Takeaways
- RDTs provide rapid results (minutes-hours), vital for prompt clinical decisions.
- Most utilize antigen-antibody reactions (e.g., immunochromatography, ELISA, agglutination).
- Key examples: Strep A, malaria, influenza, COVID-19 antigen tests.
- Molecular RDTs (e.g., GeneXpert, CBNAAT) offer high accuracy for specific targets like MTB.
- Many are Point-of-Care Tests (POCT), enabling decentralized testing.
- Sensitivity may be lower than culture; specificity is generally good.
- Primarily for pathogen detection, not antimicrobial susceptibility testing (AST).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


