Microscopy Fundamentals - Lens & Light Logic
- Core Principles
- Magnification: Apparent ↑ size.
- Resolution: Clarity; ability to distinguish two close points. Smaller 'd' (resolving power) = better resolution.
- Contrast: Difference in intensity between object & background. Staining enhances.
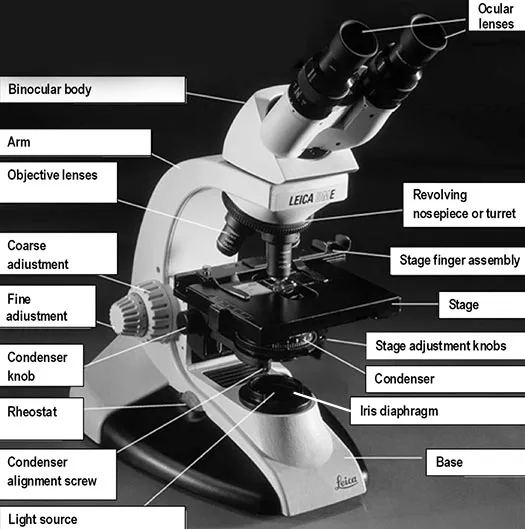
- Key Components & Light Path
- Light Source → Condenser (focuses light) → Specimen → Objective Lens → Eyepiece (Ocular Lens).
- Objective Lenses: Primary magnification (e.g., 4x, 10x, 40x, 100x). Immersion oil (refractive index n ≈ 1.5) used with 100x objective to ↑ NA & resolution.
- Eyepiece (Ocular): Secondary magnification (usually 10x).
- Total Magnification = Objective Magnification × Eyepiece Magnification.
- Optical Factors & Resolution
- Numerical Aperture (NA): Light-gathering ability of the lens. $NA = n \sin \theta$. Higher NA → ↑ resolution.
- Wavelength ($\{\lambda\}$) of light: Shorter $\{\lambda\}$ (e.g., blue light) → ↑ resolution (smaller 'd').
- Resolving power (d) is $d = \frac{0.61\lambda}{NA}$.
⭐ Better resolution (smaller 'd') is achieved with shorter light wavelength ($\lambda$) and higher numerical aperture (NA).
Light Microscopy & Stains - Colorful Clues
-
Microscopy Types:
- Bright-field: Standard; for stained specimens.
- Dark-field: For unstained, live spirochetes (e.g., Treponema). Background dark, specimen bright.
- Phase-contrast: For unstained, live cells; enhances contrast of internal structures.
- Fluorescence: Uses UV light; specimens autofluoresce or stained with fluorochromes (e.g., Auramine O for AFB).
-
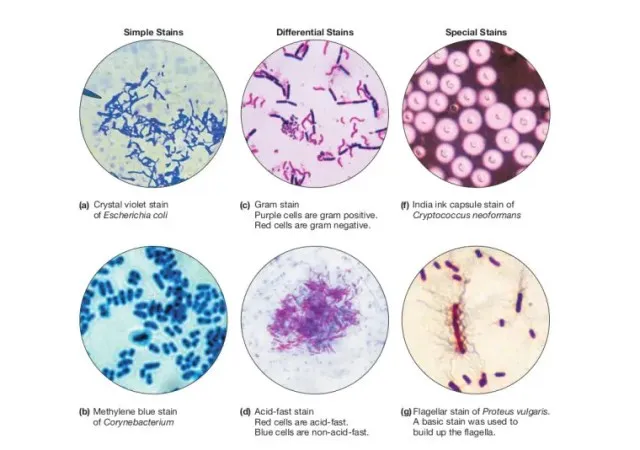
Common Stains:
- Gram Stain: Differentiates bacteria based on cell wall (Peptidoglycan).
- 📌 Mnemonic: Come In And Stain (Crystal Violet, Iodine, Acetone/Alcohol, Safranin).
- Gram +ve: Purple/Violet (thick peptidoglycan).
- Gram -ve: Pink/Red (thin peptidoglycan, outer membrane).
- Ziehl-Neelsen (ZN) Stain: For Acid-Fast Bacilli (AFB) (e.g., Mycobacterium, Nocardia).
- Primary stain: Carbolfuchsin; Decolorizer: Acid-alcohol; Counterstain: Methylene blue.
- AFB appear red; background blue.
- Albert's Stain: For Corynebacterium diphtheriae metachromatic granules (Volutin). Granules appear bluish-black, bacilli green.
- Gram Stain: Differentiates bacteria based on cell wall (Peptidoglycan).
⭐ Ziehl-Neelsen stain is crucial for identifying acid-fast bacilli like Mycobacterium tuberculosis due to their high mycolic acid content in the cell wall, resisting decolorization by acid-alcohol.
Electron Microscopy - Beyond the Light
⭐ Electron microscopy (TEM & SEM) uses an electron beam and electromagnetic lenses, achieving much higher magnification (> 100,000x) and resolution (e.g., 0.1-20 nm) than light microscopy, essential for virology and observing ultrastructures.
- Key Principle: Electrons (not light); electromagnetic lenses (not glass).
- Types & Characteristics:
- Transmission EM (TEM):
- Electrons pass through specimen.
- 2D image: internal ultrastructure (organelles, viruses).
- Requires ultrathin sections.
- Scanning EM (SEM):
- Electrons scan specimen surface.
- 3D image: surface topography.
- Sample coated with heavy metal.
- Transmission EM (TEM):
- Specimen Prep: Complex; non-living samples only.

- Clinical Significance: Viral identification, visualizing detailed microbial morphology beyond light microscopy.
High‑Yield Points - ⚡ Biggest Takeaways
- Ziehl-Neelsen stain is key for identifying acid-fast bacilli like Mycobacterium tuberculosis and Nocardia.
- Gram stain differentiates bacteria into Gram-positive (purple/violet) and Gram-negative (pink/red) based on cell wall structure.
- India ink (negative stain) is used for visualizing capsules, especially of Cryptococcus neoformans.
- Dark-field microscopy is essential for viewing thin, motile organisms like spirochetes (e.g., Treponema pallidum).
- Electron microscopy (TEM, SEM) provides ultra-structural details of microbes and viruses, not visible with light microscopy.
- Fluorescence microscopy utilizes fluorochromes (e.g., Auramine-Rhodamine for TB) for rapid and specific detection.
- Giemsa stain is valuable for detecting intracellular structures, blood parasites (e.g., Plasmodium, Leishmania), and Chlamydia inclusions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

