Spirochetes: Overview - Twisty Troublemakers
- General Characteristics:
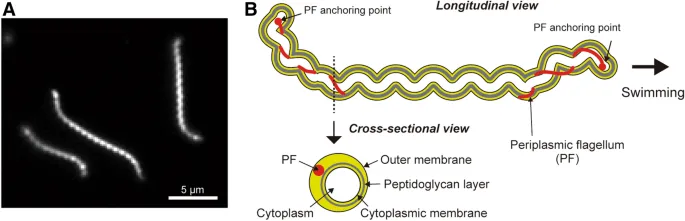
- Gram-negative, thin, flexible, spiral/helical-shaped bacteria.
- Possess endoflagella (axial filaments) in periplasmic space, enabling corkscrew motility.
- Classification: Order Spirochaetales.
- Microscopy:
- Difficult to visualize with Gram stain (too thin).
- Dark-field microscopy: Essential for live, unstained organisms.
- Silver impregnation stains: (e.g., Fontana-Tribondeau, Levaditi) for tissue sections.
- Giemsa or Wright stain: For Borrelia in blood smears.
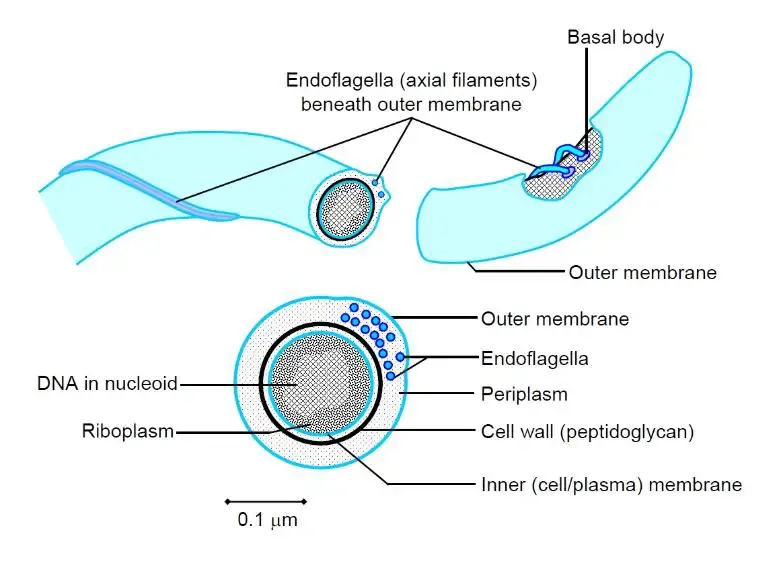
⭐ Spirochetes are notoriously difficult to Gram stain due to their thin cell wall and are best visualized using dark-field microscopy or special stains like silver impregnation (e.g., Fontana-Tribondeau).
Treponema: Syphilis - The Great Masquerader
- Treponema pallidum subsp. pallidum. Transmission: Sexual, congenital.
| Stage | Clinical Features | Diagnosis |
|---|---|---|
| Primary | Painless chancre. | Dark-field microscopy |
| Secondary | Maculopapular rash (palms/soles), condylomata lata, mucous patches. > ⭐ The Jarisch-Herxheimer reaction, an acute febrile reaction often with headache and myalgias, can occur within hours after treatment initiation for syphilis, especially with penicillin. | Serology |
| Latent | Early/Late. Asymptomatic. | Serology |
| Tertiary | Gummas, Cardiovascular (aortitis), Neurosyphilis (tabes dorsalis, general paresis). | Serology, CSF VDRL |
-
Congenital Syphilis: Hutchinson's triad (📌 Interstitial keratitis, Notched incisors, 8th nerve deafness).
-
Diagnosis Algorithm:
-
Serology:
- Non-treponemal (Screening/monitor): VDRL, RPR. 📌 VDRL False +ves: Viral, Drugs, Rheumatic fever, Lupus/Leprosy, Pregnancy.
- Treponemal (Confirmatory): FTA-ABS, TPPA, MHA-TP.
-
Treatment: Penicillin G (all stages). Jarisch-Herxheimer reaction.
Borrelia: Lyme & Relapsing Fever - Tick-Borne Terrors
Spirochetes transmitted by arthropods. Key differences:
| Feature | Lyme Disease (B. burgdorferi) | Relapsing Fever (B. recurrentis, others) |
|---|---|---|
| Vector | Ixodes ticks (hard) | Louse (epidemic), Ornithodoros ticks (soft, endemic) |
| Key Clinical Features | Stage 1: Erythema migrans (EM, "bull's-eye"). | Recurrent high fever, chills, headache. |
| Stage 2: Neuro (Bell's palsy), Cardiac (AV block). | Due to antigenic variation (key feature). | |
| Stage 3: Arthritis, Encephalopathy. | ||
| Diagnosis | Serology (ELISA, Western Blot, two-tier) | Blood smear (Giemsa/Wright) during fever. |
| Treatment | Doxycycline, Amoxicillin, Ceftriaxone | Tetracycline, Penicillin. |
📌 BAKE a Key Lyme pie: Bell's palsy, Arthritis, Karditis, Erythema migrans.

Leptospira: Leptospirosis - Weil's Wrath
- Organism: Leptospira interrogans (thin, coiled spirochete with characteristic hooked ends).
- Source: Zoonosis (rodents, domestic animals - urine).
- Transmission: Contaminated water/soil, direct contact with infected animal tissues.
- Clinical Syndromes:
- Anicteric Leptospirosis (90%): Biphasic, usually self-limited.
- Septicemic phase: Fever, myalgia (esp. calves), headache, conjunctival suffusion.
- Immune phase: Aseptic meningitis, uveitis.
- Icteric Leptospirosis / Weil's Disease (Severe, 5-10%): Characterized by jaundice, acute kidney injury (AKI), hemorrhage, and myocarditis.
⭐ Weil's disease, the severe form of leptospirosis, classically presents with a triad of jaundice, acute kidney injury, and hemorrhagic manifestations.
- Anicteric Leptospirosis (90%): Biphasic, usually self-limited.
- Diagnosis:
- Culture (Fletcher's medium): Blood/CSF (1st week), urine (after 1st week).
- Serology: MAT (Microscopic Agglutination Test) is gold standard.
- PCR: Useful for early diagnosis.
- Treatment:
- Mild disease / Prophylaxis: Doxycycline.
- Severe disease: Penicillin G or Ceftriaxone (IV).
High‑Yield Points - ⚡ Biggest Takeaways
- Spirochetes: Gram-negative, spiral-shaped bacteria with unique endoflagella for motility.
- Treponema pallidum causes syphilis; visualized by dark-field microscopy, non-culturable on artificial media.
- Borrelia burgdorferi causes Lyme disease (classic sign: erythema migrans), transmitted by Ixodes ticks.
- Leptospira interrogans causes leptospirosis (severe form: Weil's disease), from animal urine-contaminated water.
- Relapsing fever (Borrelia spp.) is characterized by recurrent fever due to antigenic variation.
- Treatments include Penicillin / Doxycycline; beware Jarisch-Herxheimer reaction with therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

