Enterobacteriaceae: General Properties - Gut Gang Basics
- Key features: Gram-negative rods, facultative anaerobes.
- Biochemical tests: Ferment glucose, oxidase-negative (key differentiator!), catalase-positive (most species).
- Metabolism: Reduce nitrates ($NO_3^-$) to nitrites ($NO_2^-$).
- Common habitats: Intestinal tract of humans/animals, also soil and water.
- Antigenic structure for serotyping:
- O antigen: Somatic, lipopolysaccharide (LPS).
- H antigen: Flagellar, protein.
- K antigen: Capsular, polysaccharide (Vi in Salmonella).

Classification by Lactose Fermentation (on MacConkey Agar):
⭐ All Enterobacteriaceae are oxidase-negative, a crucial diagnostic feature.
Escherichia coli - The Versatile Villain
- Most common facultative anaerobe in the human colon.
- Diarrheagenic E. coli (DEC) pathotypes:
- ETEC (Enterotoxigenic): Traveler's diarrhea; heat-labile (LT) & heat-stable (ST) toxins.
- EPEC (Enteropathogenic): Infantile diarrhea; attaching/effacing (A/E) lesions.
- EHEC/STEC (Enterohemorrhagic/Shiga toxin-producing): Hemorrhagic colitis, HUS; Shiga-like toxin; serotype O157:H7 is notorious.
- EIEC (Enteroinvasive): Invasive, dysentery-like illness.
- EAEC (Enteroaggregative): Persistent diarrhea, especially in children; biofilm formation.
- Extra-intestinal Infections (ExPEC):
- UTI (Uropathogenic E. coli - UPEC): Most common cause.
- Neonatal meningitis (NMEC).
- Sepsis.
- Key Virulence Factors: Adhesins (pili/fimbriae), toxins (e.g., LPS endotoxin), capsules (e.g., K1 in NMEC).

⭐ EHEC O157:H7 is associated with Hemolytic Uremic Syndrome (HUS) and characteristically does not ferment sorbitol (distinguished on sorbitol-MacConkey agar).
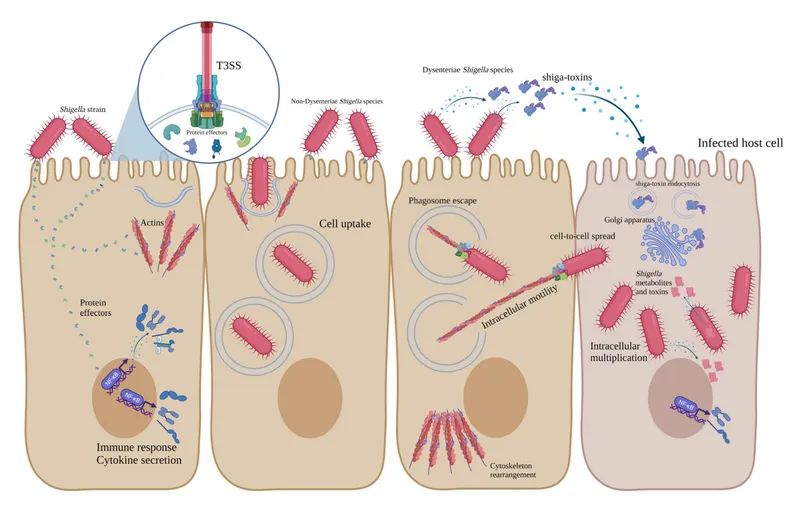
Salmonella & Shigella - Diarrhea Dynamos
Salmonella (motile, H₂S+) and Shigella (non-motile, H₂S-) are key Gram-negative bacilli causing distinct diarrheal illnesses. Differentiated by motility, H₂S production, and clinical syndromes.
| Feature | Salmonella | Shigella |
|---|---|---|
| Motility | Motile | Non-motile |
| H₂S Production | Yes (most) | No |
| Lactose Ferm. | NLF (usually) | NLF |
| Clinical | Enteric Fever (S. Typhi/Paratyphi: Vi Ag, systemic) Gastroenteritis (Non-typhoidal: local) | Bacillary Dysentery (bloody, mucoid stools) |
| Infective Dose | Higher | 10-100 organisms (very low) |
| Toxin/Virulence | Endotoxin, Vi Ag (Typhi) | Shiga toxin (S. dysenteriae), Invasiveness |
| Reservoir | Humans (Typhi), Animals (NTS e.g. poultry) | Humans |
⭐ Shigella: non-motile, H₂S negative, very low infective dose (10-100). Salmonella: motile, H₂S positive (most).
Other Enterobacteriaceae - The Notable Crew
- Klebsiella: K. pneumoniae. Capsule (mucoid). LF. Pneumonia (currant jelly sputum), UTI. 📌 '5 A's': Aspiration, Alcoholics, Abscesses, di-A-betics, current-jelly sput-A.

- Enterobacter: Motile, LF. UTI, nosocomial.
- Serratia: S. marcescens. Motile. Red pigment (prodigiosin). Nosocomial.
- Proteus: P. mirabilis/vulgaris. Highly motile (swarming). Urease +ve (struvite stones). NLF. Fishy odor. UTI.

⭐ P. mirabilis: swarming motility, urease +ve, forms struvite kidney stones.
- Yersinia:
- Y. pestis: Plague. Safety pin. Fleas.
- Y. enterocolitica/pseudotuberculosis: Enterocolitis, mesenteric adenitis (mimics appendicitis). Cold enrichment. NLF.
- Citrobacter: LF. UTI, neonatal sepsis/meningitis.
Lab Diagnosis & Treatment - ID & Attack Plan
- Specimens: Stool, urine, blood, CSF, depending on infection site.
- Culture:
- MacConkey Agar: Selective & differential (Lactose Fermenters - LF pink; Non-Lactose Fermenters - NLF colorless).
- EMB Agar: LF (E. coli - green metallic sheen), NLF.
- Hektoen Enteric (HE) / XLD Agar: For Salmonella ($H_2S$ positive → black colonies) & Shigella.
- Biochem Tests:
- Oxidase Test: Negative for all Enterobacteriaceae.
- TSI Agar: Glucose, lactose, sucrose fermentation; gas & $H_2S$ production.
- 📌 IMViC (Indole, Methyl Red, Voges-Proskauer, Citrate): E.g., E.coli (++--), Klebsiella/Enterobacter (--++).
- Serotyping: O, H, K antigens for epidemiological typing (e.g., Salmonella, E. coli).
- Treatment: Guided by susceptibility. Rising resistance (ESBLs, CRE) is a major concern.
⭐ E. coli typically shows a green metallic sheen on EMB agar.

High‑Yield Points - ⚡ Biggest Takeaways
- Gram-negative rods, oxidase-negative, glucose fermenters.
- Lactose fermentation (e.g., E. coli - LF; Salmonella - NLF) on MacConkey agar is key.
- Major pathogens: E. coli (UTI), Salmonella (typhoid), Shigella (dysentery), Klebsiella (pneumonia).
- Serotyping based on O (somatic), H (flagellar), K (capsular) antigens.
- Most are motile; exceptions: Klebsiella, Shigella, Yersinia (KSY).
- IMViC tests are vital for biochemical differentiation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

