One Health & AMR Intro - AMR's Triple Threat
- One Health: Interconnected health of humans, animals, and the environment. Essential for AMR control.
- AMR's Triple Threat:
- Humans: ↑ infections, treatment failures, mortality, healthcare costs.
- Animals: ↓ productivity, animal welfare; potential for zoonotic spread of resistant pathogens.
- Environment: Acts as a reservoir and dissemination route for resistant bacteria and antibiotic resistance genes.

⭐ The WHO has declared AMR as one of the top 10 global public health threats facing humanity.
Human Sector AMR - Hospital Hotbeds
-
Hospitals: Key AMR epicenters due to:
- High density of vulnerable, often immunocompromised, patients.
- Intensive antimicrobial use, creating strong selection pressure.
- Frequent invasive procedures & medical devices (e.g., catheters, ventilators).
-
Major Drivers of AMR in Hospitals:
- Suboptimal Infection Prevention & Control (IPC) practices (e.g., hand hygiene lapses, inadequate environmental sanitation).
- Over-prescription, incorrect dosage, or inappropriate duration of antibiotics.
- Presence and transmission of multidrug-resistant organisms (MDROs).
- Biofilm formation on indwelling medical devices.
-
Common Hospital-Acquired MDROs: MRSA (Methicillin-resistant Staphylococcus aureus), VRE (Vancomycin-resistant Enterococci), ESBL-producing Enterobacteriaceae (e.g., E. coli, Klebsiella pneumoniae), CRE (Carbapenem-resistant Enterobacteriaceae), MDR-Acinetobacter baumannii, MDR-Pseudomonas aeruginosa.
⭐ Carbapenem-resistant Enterobacteriaceae (CRE) infections are a critical concern, associated with high mortality rates (often >50%) and limited therapeutic options.
- Control Strategies: Robust Antimicrobial Stewardship Programs (ASP) and strict adherence to IPC measures are paramount for containment.
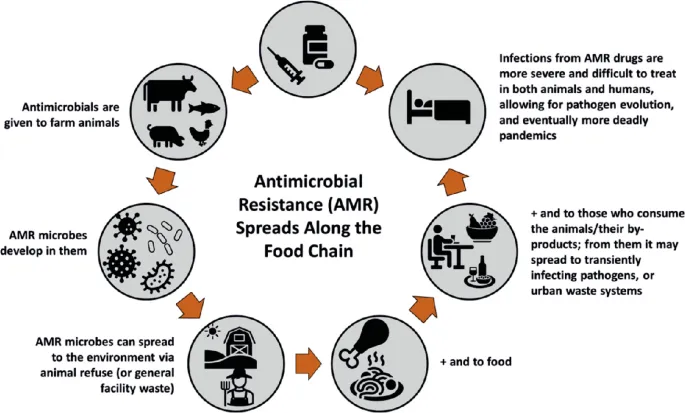
Animal Sector AMR - Farm-to-Fork Peril
- Livestock Antibiotic Use:
- Growth promotion (historical/illicit), prophylaxis, therapy.
- Leads to selection pressure for resistant strains.
- Transmission Pathways:
- Direct contact: Animal-to-human (farmers, vets).
- Foodborne: Contaminated meat, dairy, eggs.
- Environmental: Manure → soil/water → crops.
- Key Resistant Zoonotic Pathogens:
- Salmonella spp., Campylobacter spp.
- ESBL-E. coli, LA-MRSA (Livestock-Associated MRSA).
⭐ Colistin resistance (e.g., via mcr-1 gene) in E. coli from food animals is a major global concern due to its role as a last-resort antibiotic.
Environmental AMR - Silent Spreaders
- Major Contamination Sources:
- Untreated/poorly treated wastewater (hospitals, communities, pharmaceutical manufacturing).
- Agricultural runoff (livestock manure, aquaculture discharge).
- Dissemination Pathways:
- Water bodies (rivers, lakes, groundwater) → drinking water, irrigation.
- Soil → crop contamination.
- Wildlife acting as vectors.
- Key Drivers & Components:
- Sub-inhibitory antibiotic concentrations select for resistant strains.
- Presence of resistant bacteria & Antibiotic Resistance Genes (ARGs).
- Horizontal Gene Transfer (HGT) via Mobile Genetic Elements (MGEs) like plasmids.

⭐ Wastewater treatment plants (WWTPs), especially those receiving hospital or pharmaceutical effluent, are significant hotspots for the selection and dissemination of ARGs into aquatic environments globally, including India.
One Health Interventions - India's AMR Battleplan
India's National Action Plan on AMR (NAP-AMR) adopts a One Health approach, integrating human, animal, and environmental sectors. Key interventions focus on strengthening surveillance, antimicrobial stewardship (AMS), infection prevention & control (IPC), and regulating antibiotic use in livestock and agriculture.
⭐ NAP-AMR was launched in 2017 to combat AMR across India.
High‑Yield Points - ⚡ Biggest Takeaways
- One Health links human, animal, and environmental health to combat Antimicrobial Resistance (AMR).
- It demands a collaborative, multisectoral approach (human, veterinary, environmental).
- Antimicrobial overuse in humans, agriculture, and environmental contamination are key drivers.
- AMR spreads via the food chain, direct contact, and contaminated environments.
- Integrated surveillance and antimicrobial stewardship across sectors are vital interventions.
- The WHO's Global Action Plan (GAP) on AMR champions this unified strategy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

