MDR-TB 101 - Rogue Bacilli Basics
-
Definitions & Key Resistance Patterns:
Type Resistance Pattern MDR-TB Resistance to at least Isoniazid (H) AND Rifampicin (R) RR-TB Rifampicin Resistant TB; often a proxy for MDR-TB programmatically. Pre-XDR-TB MDR-TB + resistance to any Fluoroquinolone (e.g., Levofloxacin, Moxifloxacin) XDR-TB MDR-TB + resistance to any Fluoroquinolone + at least one other Group A drug (Bedaquiline or Linezolid) -
Epidemiology Snapshot:
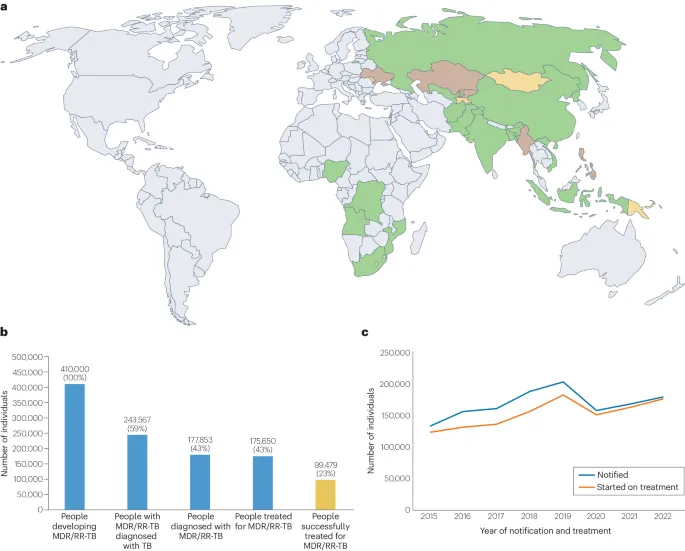
- Global: Approx. 450,000 incident RR-TB cases in 2021 (WHO).
- India: Highest MDR-TB burden; accounts for ~26% of global cases.
- Trend: ↑ drug resistance is a major public health threat.
-
High-Risk Groups for MDR-TB:
- Previously treated TB patients (especially relapse, treatment failure, default).
- Contacts of known MDR-TB/RR-TB patients.
- People living with HIV.
- Residents & staff of congregate settings (prisons, shelters).
⭐ The cornerstone definition: MDR-TB signifies resistance to at least Isoniazid (H) AND Rifampicin (R), the two most potent first-line anti-TB drugs.
Resistance & Reveal - TB's Dirty Tricks
MDR-TB: Resistance to ≥ Isoniazid (INH) & Rifampicin (RIF). Resistance via key genetic mutations.
- Rifampicin (RIF):
- Gene: rpoB (RNA polymerase B subunit)
- Mechanism: Altered drug target. >95% of RIF resistance.
- 📌 Really Bad Problem for Rifampicin.
- Isoniazid (INH):
- Gene: katG (catalase-peroxidase): High-level resistance; prevents prodrug activation.
- Gene: inhA (promoter/gene): Low-level INH & Ethionamide resistance.
- 📌 CATs Get IN High places.
Detection (NTEP Algorithm Focus):
- Genotypic (Rapid):
- NAATs: Xpert MTB/RIF (CBNAAT), LPA.
- Detects common resistance mutations.
- Phenotypic (Culture-based):
- Solid (LJ), Liquid (MGIT). Slower; confirms resistance.
⭐ CBNAAT/Xpert MTB/RIF detects M. tuberculosis and Rifampicin resistance (via rpoB gene mutations) rapidly, typically within 2 hours.
Treatment Tactics - Fighting Super TB
- Strict adherence to NTEP guidelines is paramount for MDR-TB.
- Key Regimens (NTEP-aligned):
- Shorter Oral Bdq-containing Regimen: ~9-11 months. Includes Bedaquiline (Bdq), fluoroquinolone, Linezolid (Lzd), and other agents.
- Longer All-Oral Regimens: 18-20 months. Individualized (DST-guided); uses newer (Bdq, Pa, Dlm, Lzd) & repurposed drugs.
- Crucial Newer Anti-TB Drugs:
- Bedaquiline (Bdq): Diarylquinoline; inhibits ATP synthase.
- Pretomanid (Pa): Nitroimidazole; key in BPaL/BPaLM regimens.
- Delamanid (Dlm): Nitroimidazole; inhibits mycolic acid synthesis.
- Linezolid (Lzd): Oxazolidinone; inhibits protein synthesis.
- Essential: Vigilant ADR monitoring & management. 📌 Key ADRs: QT prolongation (Bdq, Dlm, Mfx), myelosuppression (Lzd), hepatotoxicity (Pa, Bdq), optic/peripheral neuropathy (Lzd).
⭐ Bedaquiline, a diarylquinoline, inhibits mycobacterial ATP synthase (subunit c of F₀F₁ ATP synthase); crucial for MDR-TB treatment.

Contain & Conquer - TB Control Ops
- Infection Prevention & Control (IPC):
- Administrative: Triage, separation, ↓ overcrowding.
- Environmental: Ventilation (natural/mechanical).
- Personal: N95 respirators for HCWs.
- NTEP Programmatic Management (PMDT):
- Decentralized DR-TB centers.
- Nikshay portal: Case notification, tracking.
- Nutritional support (Nikshay Poshan Yojana).
- Key Challenges:
- Treatment adherence, social stigma.
- Limited access to rapid diagnostics.
⭐ Airborne infection control (AIC) measures are critical in preventing nosocomial transmission of MDR-TB.
High‑Yield Points - ⚡ Biggest Takeaways
- MDR-TB is defined by resistance to at least isoniazid (H) and rifampicin (R).
- XDR-TB is MDR-TB plus resistance to a fluoroquinolone AND a second-line injectable (e.g., amikacin).
- Rapid molecular tests (GeneXpert) detect rifampicin resistance (RR), indicating potential MDR-TB.
- Culture & DST (Drug Susceptibility Testing) confirms MDR-TB and guides therapy.
- Treatment involves shorter all-oral bedaquiline-containing regimens (9-12 months) or longer regimens (18-20 months).
- Key drugs include Bedaquiline, Pretomanid, Linezolid (BPaL), moxifloxacin, and clofazimine.
- Rifampicin Resistance (RR-TB) is generally managed as MDR-TB due to high co-occurrence rates.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

