AMS Fundamentals - Stewardship Savvy Start
- Antimicrobial Stewardship (AMS): A systematic approach to optimize antimicrobial use. Aims to improve patient outcomes, reduce microbial resistance, and decrease infection spread.
- Core Goals:
- Maximize cure, minimize toxicity.
- Prevent/slow AMR emergence.
- Reduce healthcare costs.
- The "Right" Principle: Right drug, dose, duration, route for the right patient. 📌
- Indian Imperative: Vital due to high infection rates, widespread irrational antibiotic use, & escalating AMR.

⭐ The 5 Ds of antimicrobial stewardship are crucial: Diagnosis (accurate), Drug (appropriate), Dose (optimal), Duration (shortest effective), De-escalation (when possible).
AMS Interventions - Smart Tactics Toolkit
- Core Strategies:
- Prospective Audit & Feedback (PAF): Real-time review of antimicrobial orders; direct prescriber communication for optimization.
- Formulary Restriction & Pre-authorization: Controls use of broad-spectrum/high-cost antimicrobials; requires prior approval.
- Therapy Optimization:
- IV-to-Oral (IVOTO) Switch: Early transition from IV to oral antibiotics when clinically stable.
- De-escalation: Narrowing antibiotic spectrum based on culture results and clinical improvement.
- Dose Optimization: Adjusting dose/interval based on patient factors (renal function), infection site, PK/PD.
- Supportive Interventions:
- Education & Guidelines: Regular updates; implementing evidence-based institutional pathways for common infections.
- Diagnostic Stewardship: Promoting optimal use of microbiology diagnostics (e.g., rapid tests, appropriate cultures).
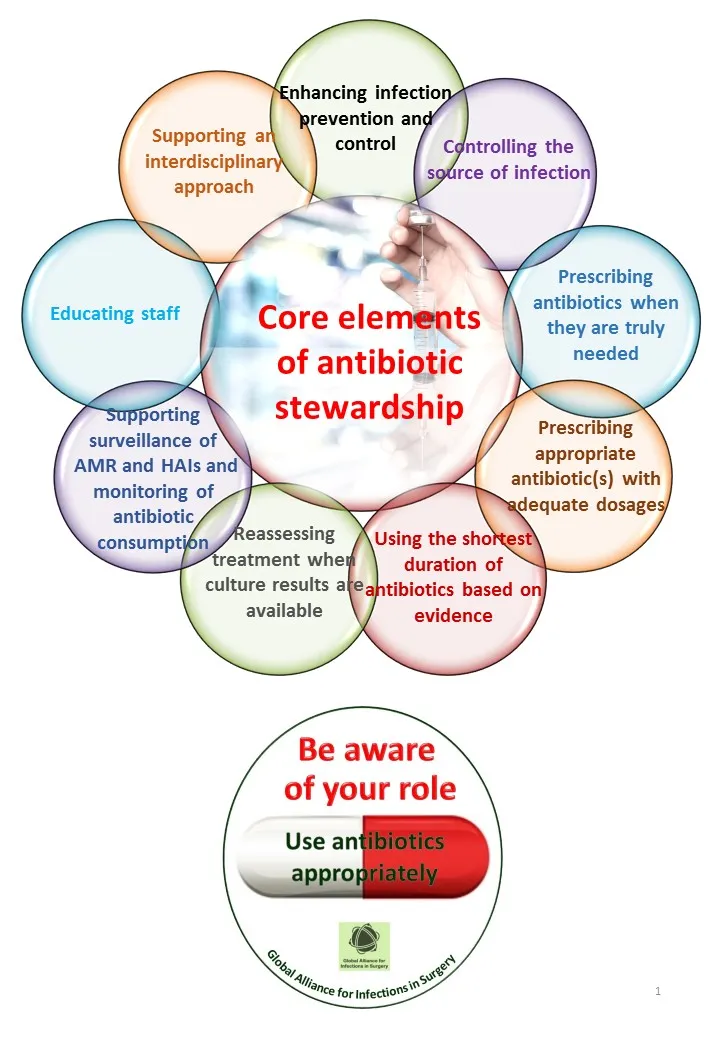
⭐ Prospective audit with intervention and feedback is a cornerstone of effective AMS.
Diagnostic & Clinical Pearls - Guiding Smart Use
Error generating content for this concept group: No object generated: the tool was not called.
AMS in India & Key Metrics - National & Numbers Game
- National Framework:
- National Action Plan on AMR (NAP-AMR): Core strategy for combating AMR.
- Indian Council of Medical Research (ICMR) AMR Surveillance Network: Tracks key resistance patterns nationally.
- State-level AMS programs & guidelines being implemented.
- Objectives: Optimize antibiotic use, ↓AMR development, improve patient safety & outcomes.
- Key Metrics for AMS Programs:
- Consumption: Defined Daily Dose (DDD)/1000 inhabitants/day or DDD/100 bed-days.
- Process: Adherence to antibiotic guidelines; pre-authorization success rates; IV-to-oral switch rates.
- Outcome: AMR rates (e.g., MRSA, CRE); Clostridioides difficile infection (CDI) rates; Length of Stay (LOS); mortality.
- WHO AWaRe (Access, Watch, Reserve) classification: Tool to guide appropriate antibiotic use.
⭐ India's National Action Plan on AMR (NAP-AMR) emphasizes strengthening Antimicrobial Stewardship (AMS) practices across all healthcare settings, including promoting rational use of antibiotics and diagnostics to curb resistance.
High‑Yield Points - ⚡ Biggest Takeaways
- AMS aims to optimize antimicrobial use, improve patient outcomes, and curb resistance.
- Core interventions: prospective audit & feedback, formulary restriction, and preauthorization.
- De-escalation (narrowing spectrum) based on culture results is vital.
- Focus on optimal dosing, shortest effective duration, and early IV-to-PO switch.
- Diagnostic stewardship (e.g., rapid diagnostics) guides therapy.
- The "5 Ds" of AMS: Right Drug, Dose, Duration, De-escalation, Diagnosis_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

