Phage Therapy & Lysins - Viral Vendetta
-
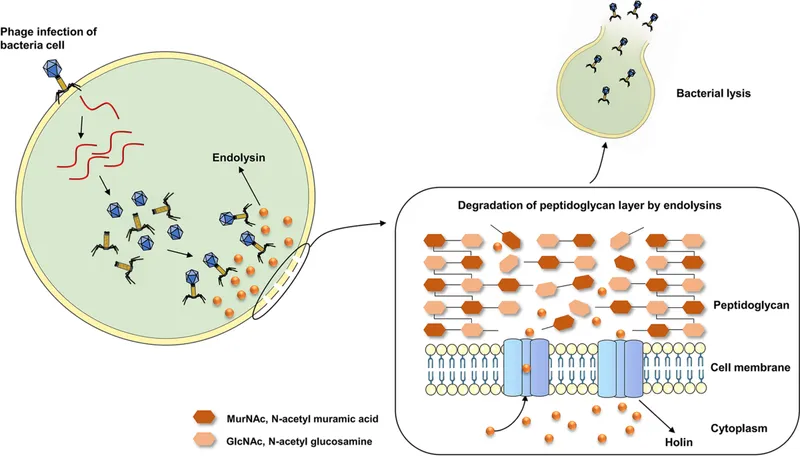
Phage Therapy: Uses bacteriophages (bacteria-specific viruses) to treat bacterial infections.
- Mechanism: Lytic phages attach, inject genetic material, replicate within, and lyse the host bacterium.
- Pros: High specificity (spares normal flora), self-replicating at infection site, effective vs. MDR strains, good biofilm penetration.
- Cons: Narrow host range (precise matching essential), potential immune response, endotoxin release (lysed Gram-negatives).
- Targets: P. aeruginosa, MRSA, A. baumannii, pathogenic E. coli.
-
Lysins (Endolysins): Phage-derived enzymes that degrade bacterial cell walls (peptidoglycan).
- Mechanism: Act rapidly externally, causing lysis on contact.
- Pros: Swift bactericidal action, broad lytic spectrum (esp. Gram+; Gram- may need permeabilizers), low resistance, anti-biofilm.
- Cons: Potential immunogenicity, challenges in systemic delivery.
- Example: Artilysins (engineered lysins).
⭐ Phages co-evolve with bacterial hosts, overcoming emerging resistance-a key advantage over static antibiotics.
Antimicrobial Peptides & Antibodies - Protein Protectors
- Antimicrobial Peptides (AMPs) / Host Defense Peptides (HDPs)
- Cationic, amphipathic molecules; part of innate immunity.
- Mechanism: Primarily disrupt microbial cell membranes (pore formation); also immunomodulatory.
- Examples: Defensins, Cathelicidin (LL-37), Colistin (Polymyxin E for MDR Gram-negatives).
- Pros: Broad-spectrum, rapid bactericidal action, low resistance development.
- Cons: Potential systemic toxicity, stability issues, production cost.
- Monoclonal Antibodies (mAbs)
- Engineered antibodies targeting specific microbial antigens or toxins with precision.
- Mechanism: Neutralize toxins/virulence factors, block pathogen entry, enhance opsonophagocytosis, ADCC (Antibody-Dependent Cell-mediated Cytotoxicity).
- Examples:
- Palivizumab (RSV F-protein; prophylaxis in high-risk infants).
- Bezlotoxumab (Clostridioides difficile toxin B; prevents recurrence).
- Raxibacumab (Anthrax protective antigen).
- Pros: High specificity, long half-life, reduced off-target effects.
- Cons: Narrow spectrum, high cost, parenteral administration.
⭐ Palivizumab, a humanized mAb, targets RSV F-protein for prophylaxis against severe RSV disease in high-risk pediatric groups.

Anti-Virulence & Microbiome - Eco-Tactics
- Anti-Virulence Therapy: Targets virulence (toxins, adhesins, QS), not growth. Disarms pathogens; ↓ resistance pressure.
- Quorum Sensing Inhibitors (QSIs): Block bacterial signals; disrupt coordinated virulence (e.g., biofilms, toxin production).
- Anti-Toxin Agents: Neutralize toxins (e.g., MABs for C. diff toxins A/B); reduce toxin-mediated damage.
- Adhesion/Biofilm Blockers: Prevent pathogen attachment to host; disrupt protective microbial communities (biofilms).
- Microbiome Modulation (Eco-Tactics): Restore/enhance protective host microbiota against pathogens.
- Probiotics: Live beneficial microbes (e.g., Lactobacillus, Bifidobacterium) to improve gut balance.
- Prebiotics: Non-digestible fibers (e.g., FOS, GOS) fueling beneficial gut bacteria.
- Synbiotics: Synergistic Probiotics + Prebiotics.
- Fecal Microbiota Transplantation (FMT): For recurrent C. difficile (rCDI); restores healthy gut flora.
- Phage Therapy: Bacteriophages specifically lyse pathogenic bacteria; re-emerging precision tool. 📌 Phages Phight Pests!
⭐ FMT shows >90% efficacy for recurrent Clostridioides difficile infection (rCDI), a major AMR concern.

High‑Yield Points - ⚡ Biggest Takeaways
- Phage therapy uses bacteriophages for specific bacterial lysis, bypassing resistance.
- Antimicrobial peptides (AMPs) offer broad-spectrum action via novel mechanisms from innate immunity.
- Monoclonal antibodies (mAbs) neutralize specific virulence factors or bacterial components.
- Probiotics and prebiotics modulate gut microbiota, enhancing host defense mechanisms.
- Vaccines are crucial for preventing infections, thereby reducing antimicrobial dependency.
- Quorum Sensing Inhibitors (QSIs) disrupt bacterial communication and virulence factor expression.
- CRISPR-Cas based antimicrobials can target resistance genes or achieve specific bacterial killing.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

