HIV Pathogenesis - Viral Villainy Unveiled
- HIV (retrovirus) infects CD4+ T-cells, macrophages, dendritic cells.
- Entry: gp120 binds CD4, then co-receptor (CCR5/CXCR4).
- CCR5: Early infection, M-tropic strains.
- CXCR4: Later infection, T-tropic strains, more cytopathic.
- Key Viral Enzymes: Reverse Transcriptase, Integrase, Protease.
- Replication Cycle:
- Outcome: Progressive ↓CD4 cell count, immune deficiency (AIDS).

⭐ HIV primarily utilizes the CCR5 co-receptor for entry in early infection (M-tropic), while CXCR4 usage (T-tropic) often emerges later and is associated with faster disease progression.
HIV Clinical & Diagnosis - Spotting The Enemy
- Acute Retroviral Syndrome (ARS): Flu/mono-like illness, high viral load (2-4 wks post-exposure).
- Clinical Latency: Asymptomatic, CD4 count gradually ↓.
- AIDS: CD4 < 200/µL or AIDS-defining illness (e.g., PCP, Kaposi Sarcoma). WHO Stage 4.
- Diagnosis:
- Initial: 4th Gen (p24 Ag + HIV Ab) test. Window period: 2-6 weeks.
- Confirmatory: HIV-1/HIV-2 differentiation assay or NAT.
- NAT: Detects HIV RNA. Shortest window (1-4 weeks); for acute/neonatal Dx.
⭐ Most common opportunistic infection in HIV patients in India is Tuberculosis.
HIV Management - Fighting Back Smart
- ART Initiation: Start immediately for all PLHIV, regardless of CD4 count. Goal: viral suppression.
- Monitoring: VL at 6, 12 months, then annually if suppressed (<50 copies/mL). CD4 if advanced/unsuppressed.
- PEP: ASAP (<2h ideal, max 72h) post-exposure; TDF + 3TC + DTG for 28 days.
- PrEP: Daily TDF/FTC or TDF/3TC for high-risk individuals.
- IRIS: Paradoxical worsening on ART; manage OI, continue ART.
⭐ Preferred first-line ART (NACO): Tenofovir (TDF) + Lamivudine (3TC) + Dolutegravir (DTG) as a fixed-dose combination.
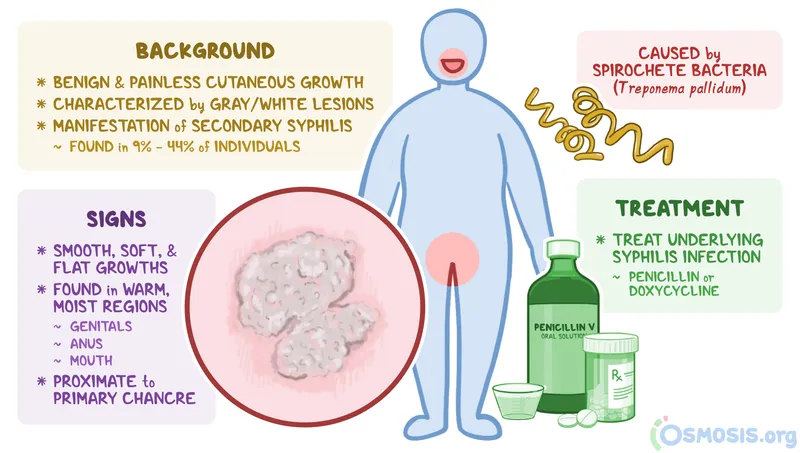
Syphilis Spotlight - The Ancient Foe
- Agent: Treponema pallidum.
- Stages:
- Primary: Painless chancre.
- Secondary: Rash (palms/soles), condyloma lata.
⭐ Jarisch-Herxheimer Reaction: Post-Rx fever, chills, myalgia from treponemal lysis; self-limiting. Usually within 2-12h.
- Latent: Asymptomatic (early/late).
- Tertiary: Gummas, neurosyphilis, cardiovascular.
- Diagnosis: Screen: VDRL/RPR. Confirm: TPPA/FTA-ABS.
- Treatment (Penicillin G):
- Early (1°, 2°, Early Latent): Benzathine 2.4 MU IM x1.
- Late Latent/Tertiary: Benzathine 2.4 MU IM weekly x3.
- Neurosyphilis: Aqueous Crystalline 18-24 MU IV daily x10-14d.
Gonorrhea & Chlamydia - Dual Trouble Duo
- Co-infection common. Dx: NAAT.
- Dual Tx for co-infection.
| Feature | Gonorrhea (GC) | Chlamydia (CT) |
|---|---|---|
| Organism | Gram -ve diplococci | Obligate intracellular |
| Symptoms | Purulent D/C, PID, DGI | Often Asx, PID |
| Tx (Uncomp.) | Ceftriaxone 500mg IM + Azithro 1g PO | Azithro 1g PO or Doxy 100mg BD x7d |
⭐ Fitz-Hugh-Curtis: perihepatitis (RUQ pain, violin-string adhesions) with PID (GC/CT).
Other STIs - Rapid Roundup Reel
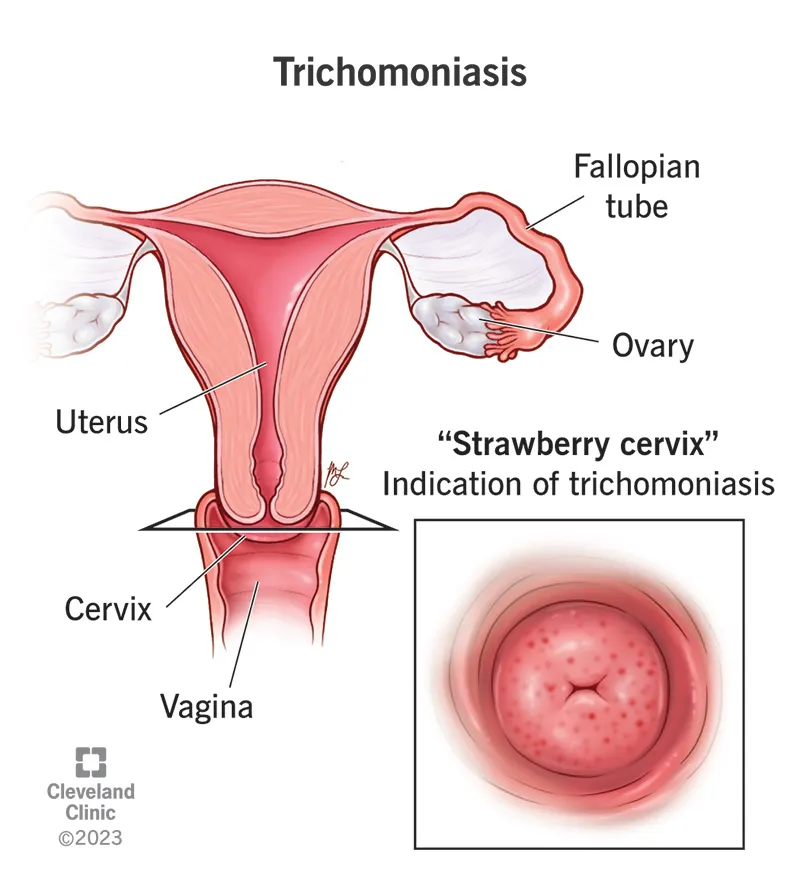
- Trichomoniasis: T. vaginalis; frothy discharge, strawberry cervix. Metronidazole 2g PO single.
- HPV (Warts): HPV; condylomata acuminata. Podophyllin, Imiquimod.
- HSV (Herpes): HSV; painful vesicles. Acyclovir.
- Chancroid: H. ducreyi; painful ulcer. Azithromycin 1g PO single.
- LGV: C. trachomatis L1-L3; adenopathy. Doxycycline.
⭐ LGV: C. trachomatis L1-L3; pathognomonic "groove sign".
- Donovanosis: K. granulomatis; beefy-red ulcer, Donovan bodies. Azithromycin.
High‑Yield Points - ⚡ Biggest Takeaways
- HIV primarily targets CD4+ T-lymphocytes; HAART is crucial for management.
- Syphilis (Treponema pallidum) presents with a painless chancre; screen with VDRL/RPR, confirm with FTA-ABS/TPHA.
- Gonorrhea (Neisseria gonorrhoeae) shows Gram-negative diplococci; causes urethritis and cervicitis.
- Chlamydia (Chlamydia trachomatis) is often asymptomatic; can lead to PID and infertility.
- Genital Herpes (mainly HSV-2) is characterized by painful vesicular lesions.
- HPV serotypes 16 & 18 are linked to cervical cancer; 6 & 11 cause genital warts (condyloma acuminata).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

