Chlamydial Infections - The Obligate Intruder
- Obligate intracellular bacteria; energy parasites (cannot synthesize ATP). Poorly Gram-staining.
- Chlamydia trachomatis is the most common species.
- Serovars A, B, Ba, C: Trachoma (chronic keratoconjunctivitis).
- Serovars D-K: Urogenital infections (urethritis, cervicitis, PID), neonatal conjunctivitis, infant pneumonia.
- Serovars L1, L2, L3: Lymphogranuloma Venereum (LGV).
- Unique biphasic lifecycle:
- Elementary Body (EB): Small, dense, infectious, extracellular. Metabolically inert. 📌 Elementary = Enters cell.
- Reticulate Body (RB): Larger, metabolically active, replicative, intracellular. 📌 Reticulate = Replicates.
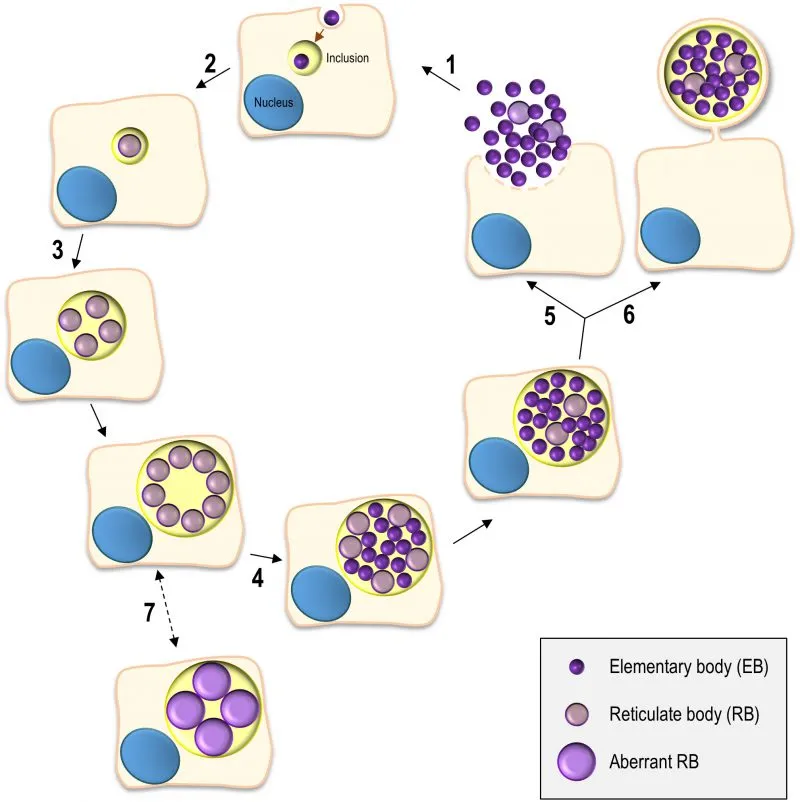
⭐ C. trachomatis lacks a typical peptidoglycan layer but possesses penicillin-binding proteins (PBPs), rendering it susceptible to certain β-lactam antibiotics despite its "atypical" nature.
Chlamydial Infections - Silent Spread & Sequelae
- Chlamydia trachomatis: Obligate intracellular; often asymptomatic, enabling silent spread and delayed diagnosis.
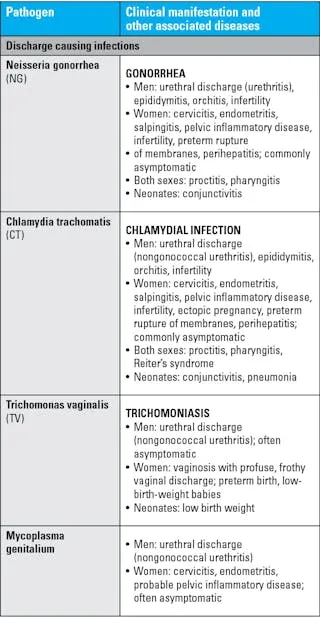
- Urogenital Manifestations:
- Males: Urethritis (mucoid discharge), epididymitis.
- Females: Cervicitis, Pelvic Inflammatory Disease (PID); frequently subclinical, risking severe sequelae.
- Neonatal:
- Conjunctivitis: 5-14 days post-birth; mucopurulent.
- Pneumonia: Afebrile, staccato cough; 4-12 weeks post-birth.
- Key Sequelae:
- PID leads to: Infertility, ectopic pregnancy, chronic pelvic pain.
- Reactive Arthritis (Reiter's): Urethritis, arthritis, conjunctivitis. 📌 "Can't see, can't pee, can't climb a tree."
- Lymphogranuloma Venereum (LGV): Serovars L1-L3.
⭐ Up to 40% of untreated chlamydial infections in women progress to Pelvic Inflammatory Disease (PID), a leading cause of preventable infertility.
Chlamydial Infections - Beyond the Belt
- Lymphogranuloma Venereum (LGV): C. trachomatis L1-L3.
- Primary: Evanescent ulcer. Secondary: Painful inguinal buboes.
- Tertiary: Genital elephantiasis, strictures.
- Rx: Doxycycline 100mg BD for 21 days.
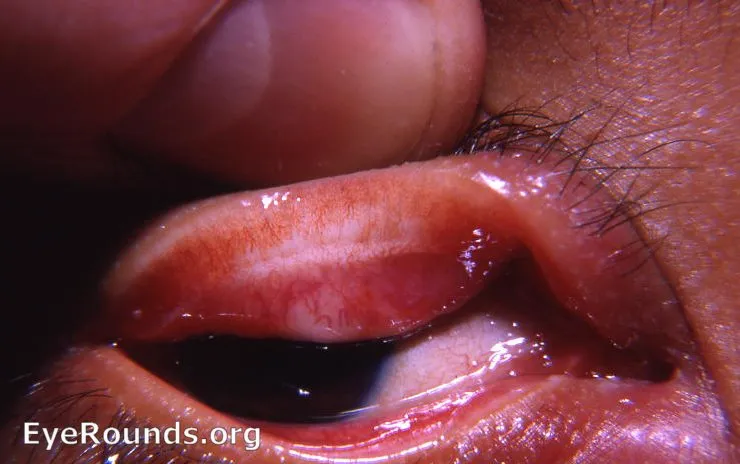
- Trachoma: C. trachomatis A-C.
- Leading preventable infectious blindness.
- Signs: Follicles, Arlt's line (scarring), trichiasis, corneal opacity.
- 📌 SAFE strategy: Surgery, Antibiotics, Facial cleanliness, Environmental hygiene.
- Reactive Arthritis (Reiter's Syndrome):
- Aseptic arthritis post-Chlamydia.
- 📌 Triad: Conjunctivitis/uveitis, urethritis, arthritis.
- HLA-B27 associated.
⭐ The "Groove sign" in LGV is pathognomonic, formed by inguinal ligament separating inflamed lymph node groups.
Chlamydial Infections - Detective Work & Takedown
- Diagnosis (Dx):
- Gold Standard: Nucleic Acid Amplification Tests (NAATs).
- Samples: First-catch urine (men), endocervical/vaginal swabs (women). Rectal/pharyngeal swabs if indicated.
- Management (Rx):
- Uncomplicated Genital Chlamydia:
- Azithromycin 1g single dose OR
- Doxycycline 100mg BD for 7 days.
- Partner Management: Treat all sexual partners from the last 60 days. Expedited Partner Therapy (EPT) if available.
- Screening: Annually for sexually active women <25 yrs & older women with risk factors. MSM at least annually.
- Test of Cure: Not routinely needed; consider in pregnancy (3-4 wks post-Rx).
- Uncomplicated Genital Chlamydia:
⭐ Chlamydia trachomatis is a leading cause of preventable blindness (trachoma) and reactive arthritis (Reiter's syndrome).
High-Yield Points - ⚡ Biggest Takeaways
- Most common bacterial STI; C. trachomatis serovars D-K (urogenital), L1-L3 (LGV).
- Frequently asymptomatic, especially in women, risking PID, infertility, ectopic pregnancy.
- Males: Non-gonococcal urethritis (NGU), epididymitis.
- Neonates: Inclusion conjunctivitis, afebrile pneumonia.
- NAAT (e.g., PCR) is the gold standard for diagnosis.
- Treatment: Azithromycin (1g single dose) or Doxycycline (100mg BD, 7 days).
- Associated with Reactive Arthritis (Reiter's syndrome).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

