Chancroid - Ducreyi's Painful Dagger
- Causative Agent: Haemophilus ducreyi (Gram-negative coccobacillus).
- Microscopy: "School of fish" or "railroad track" appearance.
- Clinical Features: 📌 'Ducreyi makes you cry' (painful).
- Ulcer: Painful, soft, non-indurated, ragged/undermined edges. Base often has grey/yellow exudate.

- Bubo: Tender, unilateral, suppurative inguinal lymphadenopathy (bubo) in ~50% cases; may rupture.
- Ulcer: Painful, soft, non-indurated, ragged/undermined edges. Base often has grey/yellow exudate.
- Diagnosis:
- Primarily clinical + exclusion of other causes (syphilis, HSV).
- Definitive: Culture (special media, difficult) or NAAT/PCR (most sensitive & specific).
- Gram stain: Low sensitivity.
- Treatment (Single Dose Regimens Preferred):
- Azithromycin 1g PO single dose.
- Ceftriaxone 250mg IM single dose.
- Alternatives: Ciprofloxacin, Erythromycin.
⭐ Co-infection with HIV is common, and chancroid ulcers facilitate HIV transmission.
Syphilitic Chancre - Treponema's Tricky Ulcer
- Organism: Treponema pallidum (spirochete).
- Clinical Features:
- Typically single, painless, indurated ulcer ("Hunterian chancre") with clean base, raised firm (cartilaginous) borders.

- Bilateral non-tender, rubbery lymphadenopathy.
- Incubation: 9-90 days (average 3 weeks).
- Typically single, painless, indurated ulcer ("Hunterian chancre") with clean base, raised firm (cartilaginous) borders.
- Diagnosis:
- Dark-field microscopy: Gold standard from lesion exudate (shows motile spirochetes).

- Serology:
- Non-treponemal (VDRL/RPR): May be negative in early primary syphilis.
- Treponemal (FTA-ABS/TPPA): More specific, confirm reactivity.
- Dark-field microscopy: Gold standard from lesion exudate (shows motile spirochetes).
- Treatment:
- Benzathine Penicillin G 2.4 million units IM single dose.
- 📌 Mnemonic: T. pallidum = Painless primary ulcer. Penicillin G is the cure.
⭐ A syphilitic chancre is highly infectious, even if painless.
Genital Herpes - Vexing Viral Vesicles
- Etiology & Presentation: Caused by Herpes Simplex Virus (HSV), predominantly HSV-2 > HSV-1. Characterized by multiple, painful vesicles on an erythematous base, progressing to shallow ulcers. Associated with dysuria and tender inguinal adenopathy. Recurrences are common, often heralded by a prodrome (e.g., tingling, burning).
- Diagnosis:
- Primarily clinical.
- Confirmation: Viral culture (from active lesions), PCR (most sensitive).
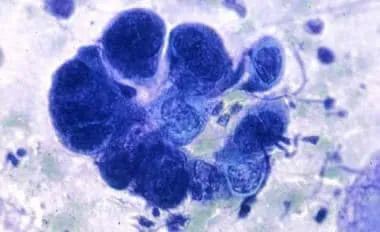
- Supportive: Tzanck smear (reveals multinucleated giant cells; supportive, not specific).
- Management: Antivirals like Acyclovir, Valacyclovir, Famciclovir for episodic or suppressive therapy.
- First episode: e.g., Acyclovir 400mg TID for 7-10 days.
⭐ Most genital herpes infections are transmitted by individuals unaware they have the infection or who are asymptomatic at the time of transmission.
Rare Rivals - LGV & Donovanosis
| Feature | Lymphogranuloma Venereum (LGV) | Donovanosis (Granuloma Inguinale) |
|---|---|---|
| Organism | Chlamydia trachomatis (L1-L3) | Klebsiella granulomatis |
| Primary Lesion | Transient, painless ulcer/papule. | Painless, progressive, 'beefy-red', friable ulcer. 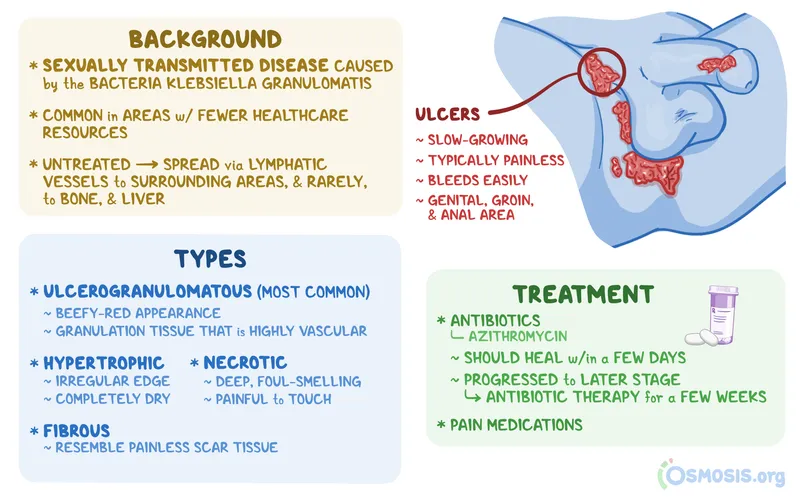 |
| Lymphadenopathy | Painful buboes (true adenitis); 'Groove sign'.  | Pseudobuboes (subcutaneous granulomas). |
| Other Features | Proctocolitis. | Ulcers bleed easily; tissue destruction. |
| Diagnosis | NAAT, Serology. | Tissue smear: Donovan bodies (macrophages). |
| Rx (Treatment) | Doxycycline 100mg BID for 21 days. | Azithromycin 1g weekly for ≥3 weeks. |
High‑Yield Points - ⚡ Biggest Takeaways
- Chancroid (H. ducreyi): Painful ulcer, suppurative buboes; "school of fish" microscopy. Rx: Azithromycin.
- Syphilis (T. pallidum): Painless, indurated chancre. Rx: Penicillin G.
- Genital Herpes (HSV): Painful vesicles then ulcers; recurrent. Rx: Acyclovir.
- LGV (C. trachomatis L1-L3): Transient ulcer, painful lymphadenopathy ("groove sign"). Rx: Doxycycline.
- Granuloma Inguinale (K. granulomatis): Painless, progressive, beefy-red ulcer; Donovan bodies. Rx: Azithromycin.
- Pain differentiates: Chancroid/Herpes (painful); Syphilis/LGV/Donovanosis (painless).
- Always test for HIV co-infection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

