OSA Fundamentals - Snore Wars Patho
- Sleep-Disordered Breathing (SDB): Spectrum of abnormalities; Obstructive Sleep Apnea (OSA) is most common, featuring recurrent upper airway collapse during sleep leading to ↓ or absent airflow.
- Prevalence (India): Estimated ~4-13.7% in adults.
- Key Risk Factors: 📌 OSA COMICS
- Obesity: BMI > 30 kg/m²
- Male gender
- Age: ↑ risk
- Craniofacial: Retrognathia, micrognathia, tonsillar/adenoidal hypertrophy
- Ingestants: Alcohol, sedatives
- Circumference (Neck): > 17 inches (men), > 16 inches (women)
- Smoking, Family history
- Pathophysiology: Recurrent upper airway collapse → intermittent hypoxia/hypercapnia → sleep fragmentation → sympathetic activation.
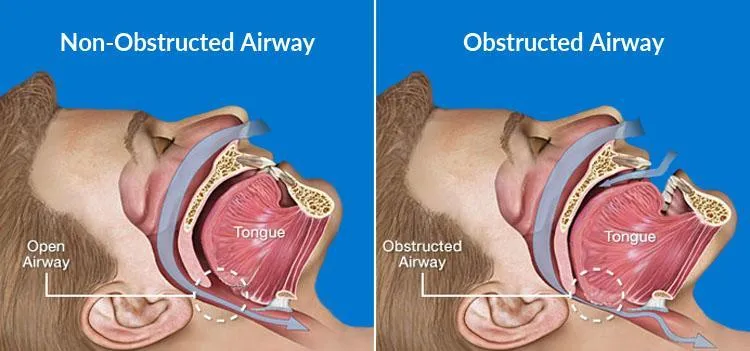
⭐ The most significant modifiable risk factor for OSA is obesity, particularly visceral adiposity.
OSA Diagnosis - Catching Zzz's Clues
- Clinical Features:
- Nighttime: Loud snoring, witnessed apneas, gasping/choking, nocturia.
- Daytime: Excessive Daytime Sleepiness (EDS) - assess with Epworth Sleepiness Scale (ESS), morning headaches, poor concentration, mood changes.
- Screening Tools:
- 📌 STOP-BANG: Snoring, Tired, Observed apnea, Pressure (BP), BMI >35 kg/m$^2$, Age >50yrs, Neck circumference >40cm, Gender (Male). Score ≥3 → high risk.
- Diagnostic Standard: Polysomnography (PSG)
- Gold standard. Key parameters: Apnea-Hypopnea Index (AHI), Respiratory Disturbance Index (RDI), Oxygen Desaturation Index (ODI), arousal index.
- Apnea: ≥90% airflow reduction for ≥10s.
- Hypopnea: ≥30% airflow reduction for ≥10s + ≥3% $O_2$ desaturation or arousal.
- Home Sleep Apnea Testing (HSAT):
- Indications: High pre-test probability of moderate-severe uncomplicated OSA.
- Limitations: Cannot rule out OSA if negative; not for complex cases (e.g., CHF, COPD).
⭐ An Epworth Sleepiness Scale (ESS) score >10 suggests clinically significant daytime sleepiness.
AHI Severity Classification (Adults)
| Severity | AHI (events/hr) |
|---|---|
| Normal | <5 |
| Mild | 5-14 |
| Moderate | 15-29 |
| Severe | ≥30 |
OSA Management - Breathing Easy Again
Goals: Normalize AHI/RDI, ↑sleep quality & alertness, ↓symptoms & complications.
- Lifestyle: Weight loss (10% or BMI <25 kg/m²), positional therapy (avoid supine), avoid alcohol/sedatives pre-sleep, smoking cessation.
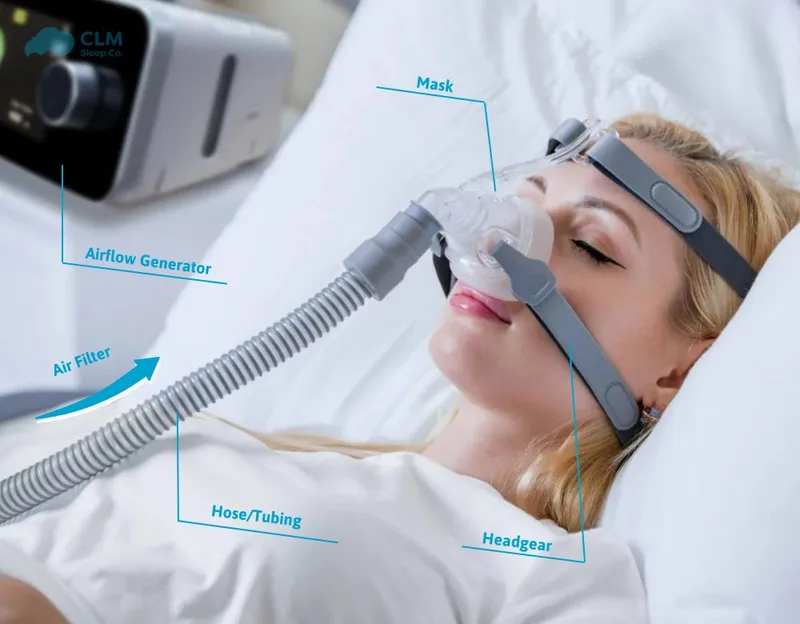
- PAP Therapy: 📌 PAP Smear (CPAP, APAP, BiPAP).
- CPAP: 1st line (mod-severe OSA & symptomatic mild). Compliance >4hrs/night on >70% of nights.
⭐ CPAP is the gold standard treatment for moderate to severe OSA.
- APAP/BiPAP: For CPAP intolerance, high pressure needs, or comorbid hypoventilation.
- Oral Appliances: Mandibular advancement devices (MADs), tongue-retaining devices. For mild-moderate OSA or CPAP failure/intolerance.
- Surgical Options: UPPP, MMA, genioglossus advancement, hypoglossal nerve stimulation, tracheostomy. For specific anatomical issues or CPAP failure.
- Pharmacotherapy: Limited role. E.g., modafinil/solriamfetol for residual EDS despite optimal CPAP.
- Complications (Untreated): CV (HTN, CAD, AF, Stroke), Metabolic (T2DM, Insulin Resistance), Neurocognitive (↓Memory, ↑Accidents), NAFLD.
CSA & OHS - Central & Weighty Woes
- Central Sleep Apnea (CSA): No airflow & no respiratory effort (≥10s).
- Types: Cheyne-Stokes (CHF LVEF ≤45%), high-altitude, drug-induced (e.g., opioids).
- Dx: PSG shows absent thoracoabdominal effort.
- Rx: Treat cause, CPAP/BiPAP, ASV (⚠️ HFrEF LVEF ≤45% & predominant CSA).
- Obesity Hypoventilation Syndrome (OHS): BMI ≥30 kg/m², awake PaCO₂ >45 mmHg.
- Rx: Weight loss (primary), PAP (often BiPAP).
| Feature | OSA | CSA | OHS |
|---|---|---|---|
| Effort during apnea | Present (paradoxical) | Absent | Variable (often present if OSA coexists) |
| Awake PaCO₂ | Normal | Low/Normal | >45 mmHg |
| Common Assoc. | Obesity, craniofacial | CHF, stroke, opioids | Obesity |
⭐ Adaptive Servo-Ventilation (ASV) is contraindicated in patients with chronic heart failure (LVEF ≤45%) and predominant central sleep apnea due to increased mortality risk (SERVE-HF trial).
High‑Yield Points - ⚡ Biggest Takeaways
- Obstructive Sleep Apnea (OSA): Most common SDB, from recurrent upper airway collapse during sleep.
- Apnea-Hypopnea Index (AHI): Key for diagnosis/severity: Mild (5-15), Moderate (15-30), Severe (>30 events/hr).
- Polysomnography (PSG): Gold standard diagnostic investigation.
- CPAP: First-line treatment for symptomatic moderate-severe OSA.
- Central Sleep Apnea (CSA): Due to impaired central respiratory drive; Cheyne-Stokes respiration is a classic pattern.
- Obesity Hypoventilation Syndrome (OHS): Obesity (BMI ≥30 kg/m²), daytime hypercapnia (PaCO2 >45 mmHg), sleep disordered breathing.
- Untreated OSA significantly increases risk of hypertension, cardiovascular disease, and stroke.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

