Pulmonary Hypertension - Pressure Cooker Lungs
-
Definition: Mean Pulmonary Arterial Pressure (mPAP) > 20 mmHg at rest, confirmed by Right Heart Catheterization (RHC). Pulmonary Vascular Resistance (PVR) > 3 Wood units is also significant. $PVR = (mPAP - PAWP) / CO$.
-
Pathophysiology: Vasoconstriction, vascular remodeling (medial hypertrophy, intimal proliferation, fibrosis), in-situ thrombosis, inflammation.
-
Symptoms: Progressive dyspnea (most common), fatigue, exertional chest pain, lightheadedness, syncope.
-
Signs: Loud P2 (often palpable), RV heave/lift, tricuspid regurgitation murmur, ↑JVP (prominent 'a' or 'v' waves), hepatomegaly, peripheral edema, ascites.
-
WHO Classification (Simplified):
Group Category Key Examples 1 Pulmonary Arterial Hypertension (PAH) Idiopathic (IPAH), Heritable, CTD-PAH, Drug-induced 2 PH due to Left Heart Disease (LHD) HFrEF, HFpEF, Valvular heart disease 3 PH due to Lung Diseases &/or Hypoxia COPD, ILD, Sleep-disordered breathing, Alveolar hypoventilation 4 PH due to PA Obstructions (CTEPH) Chronic Thromboembolic Pulmonary Hypertension 5 PH with Unclear/Multifactorial Mechanisms Hematologic, Systemic, Metabolic disorders, Misc. 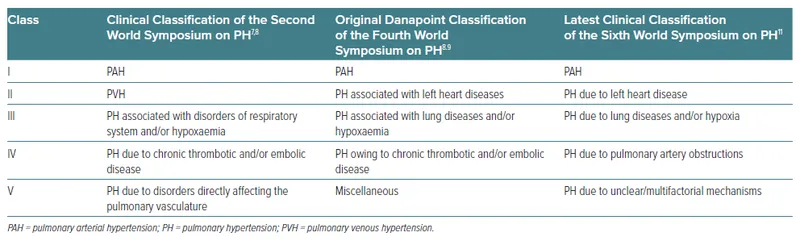
-
Simplified Diagnostic Algorithm:
-
Key Investigations: ECG (RV hypertrophy/strain, RAE), CXR (enlarged PAs, RVH), Echocardiogram (initial non-invasive screening & PAP estimation), RHC (gold standard for diagnosis, severity & vasoreactivity), V/Q scan (essential to rule out CTEPH), PFTs, HRCT chest.
-
Management Goals:
- Treat underlying cause (e.g., LHD, lung disease).
- Supportive therapy: Oxygen (if hypoxic), diuretics (for RV failure), anticoagulation (esp. IPAH, HPAH, CTEPH).
- Targeted therapies (primarily for PAH Group 1): Prostanoids (e.g., epoprostenol), Endothelin Receptor Antagonists (ERAs, e.g., bosentan, ambrisentan), PDE5 inhibitors (e.g., sildenafil, tadalafil), soluble Guanylate Cyclase (sGC) stimulators (e.g., riociguat).
⭐ Right Heart Catheterization (RHC) is mandatory for the diagnosis of pulmonary hypertension and to guide therapy, especially in PAH (Group 1).
Pulmonary Embolism - Clot on the Block
Thrombus obstructs pulmonary artery. Pathophys: Virchow's Triad (endothelial injury, stasis, hypercoagulability).
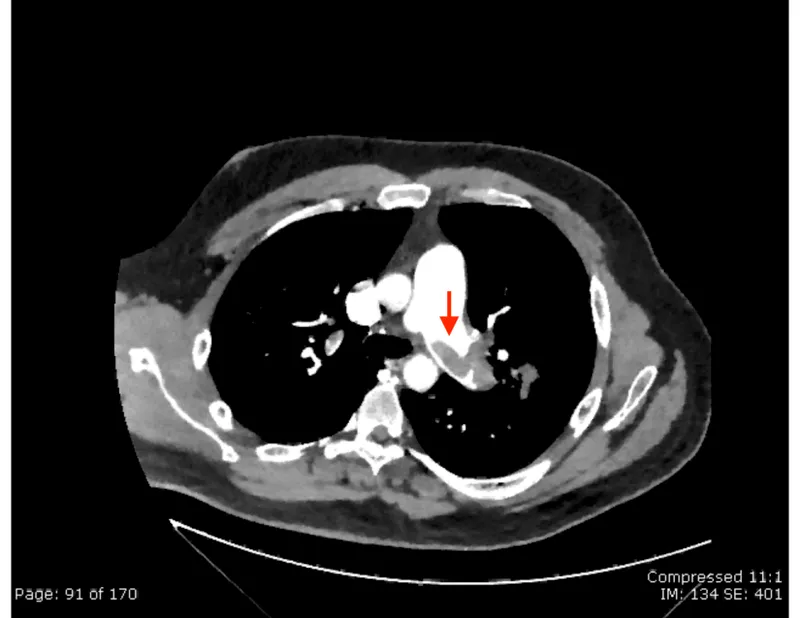
- Risk Factors: Prior VTE, surgery (ortho), cancer, immobility, OCPs/HRT, pregnancy, thrombophilias (Factor V Leiden).
- Features: Sudden dyspnea, pleuritic pain, cough, hemoptysis. Signs: tachypnea, tachycardia, DVT signs; hypotension (massive PE).
- Diagnosis:
- Wells' Score (PE likely >4):
Criteria Pts DVT signs 3 PE #1 Dx 3 HR >100 1.5 Immob/Surg <4wk 1.5 Prev DVT/PE 1.5 Hemoptysis 1 Malignancy 1 - D-dimer (rules out in low prob.), CTPA (gold standard), V/Q scan (if CTPA C/I).
- ECG: S1Q3T3 (📌), RBBB, sinus tachy. CXR: Often normal; Westermark sign, Hampton's hump.
- Wells' Score (PE likely >4):
- Management:
- Supportive: O2, fluids/pressors.
- Anticoagulation: LMWH/UFH then DOACs/VKA (≥3 months).
- Thrombolysis (alteplase): For massive PE.
- Catheter-directed therapy/embolectomy: Severe cases. IVC filter if anticoagulation C/I.
⭐ The S1Q3T3 pattern on ECG, though classic, is neither sensitive nor specific for pulmonary embolism.
Cor Pulmonale & CTEPH - Right Heart's Burden
- Cor Pulmonale: RV hypertrophy/dilation from lung structure/function diseases or pulmonary vasculature (excludes LHD).
- Causes: COPD (most common), ILD, cystic fibrosis, severe kyphoscoliosis, chronic PE, primary PH.
- Pathophysiology: Pulmonary hypertension → ↑RV afterload → RV dysfunction.
- Clinical Features: Underlying lung disease symptoms + dyspnea, fatigue, exertional syncope, peripheral edema, ascites, JVD, loud P2, RV heave, tricuspid regurgitation.
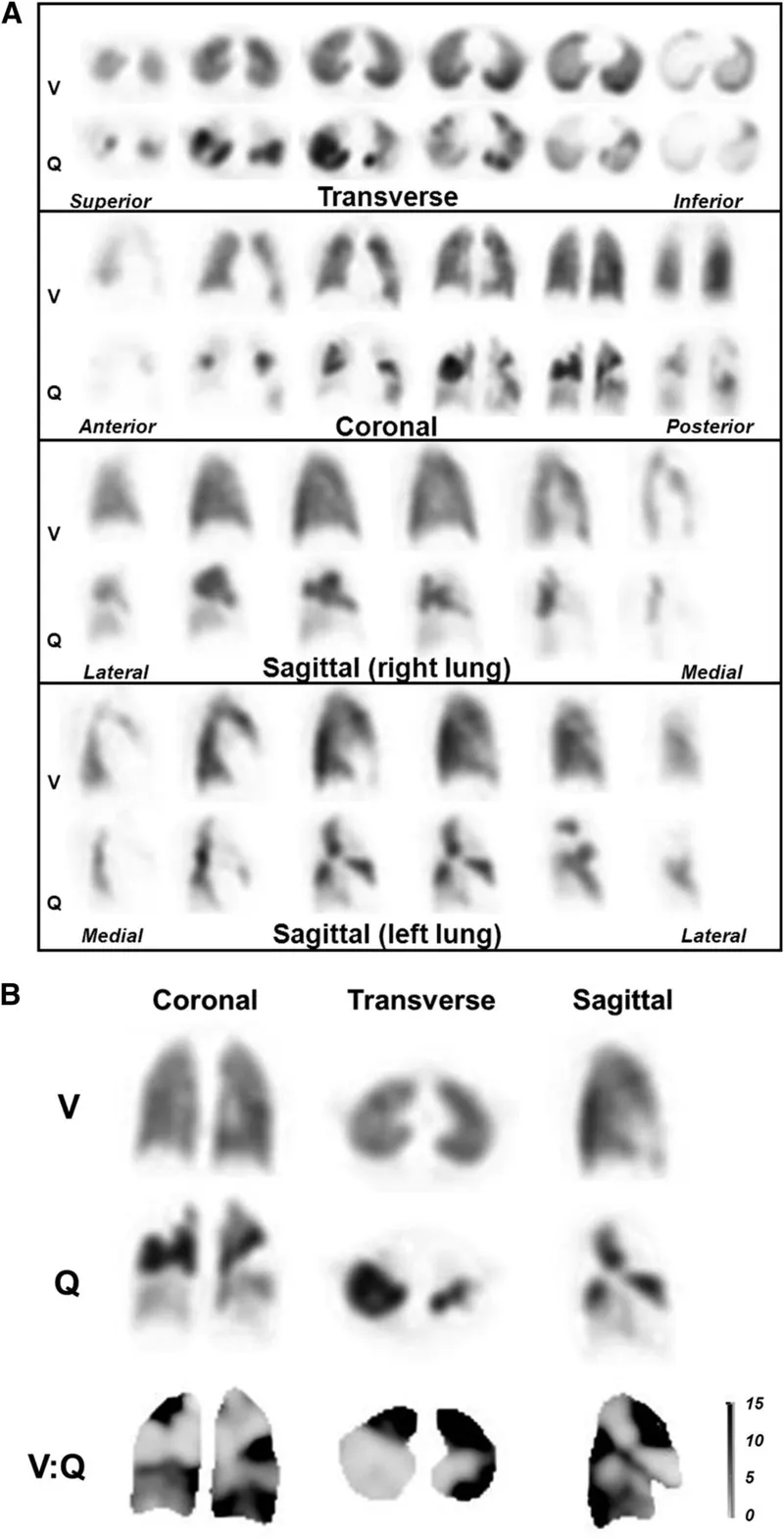
- CTEPH (Chronic Thromboembolic Pulmonary Hypertension): PH Group 4; unresolved PE leads to obstruction.
- Diagnosis: V/Q scan (key screening: mismatched perfusion defects); confirm: RHC, CTPA, pulmonary angiography.
- Management:
- Lifelong anticoagulation.
- Pulmonary Endarterectomy (PEA) - potentially curative if eligible.
- Balloon Pulmonary Angioplasty (BPA) - for non-operable distal disease.
- Medical: Riociguat.
⭐ Pulmonary endarterectomy (PEA) is the treatment of choice and offers a potential cure for eligible patients with CTEPH.
- Diagnosis: V/Q scan (key screening: mismatched perfusion defects); confirm: RHC, CTPA, pulmonary angiography.
High‑Yield Points - ⚡ Biggest Takeaways
- Pulmonary Embolism (PE): CTPA for diagnosis; anticoagulation for treatment. Wells score stratifies risk.
- Pulmonary Arterial Hypertension (PAH): Mean PAP ≥25 mmHg; right heart catheterization for diagnosis.
- Cor Pulmonale: RV failure from chronic lung disease, typically COPD.
- Fat Embolism Syndrome: Triad: respiratory distress, neurological deficits, petechial rash post-trauma.
- Massive PE: Presents with hypotension; requires thrombolysis or embolectomy.
- D-dimer: High negative predictive value helps exclude PE in low-risk individuals.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

