Pleural Effusion Essentials - Fluid Follies
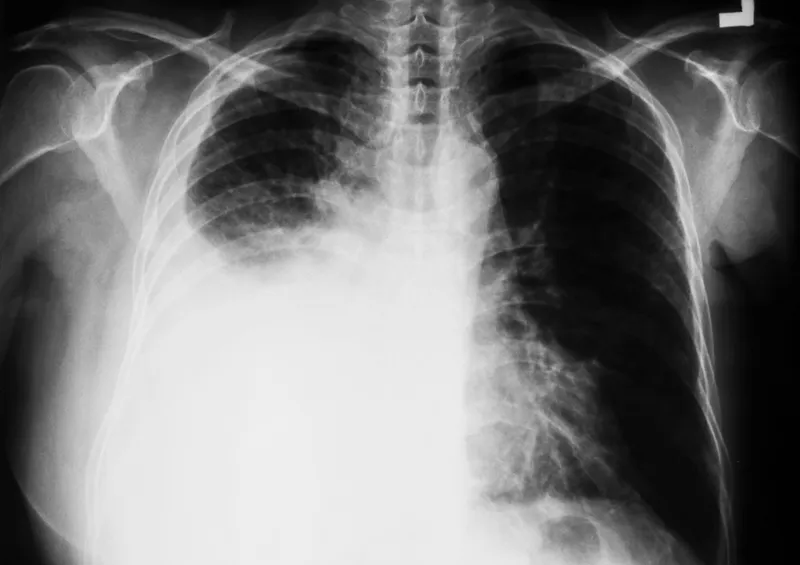
Excess fluid in pleural space.
-
Types:
Feature Transudate Exudate Mechanism Systemic (↑ hydrostatic, ↓ oncotic P) Local (↑ permeability, ↓ drainage) Appearance Clear Cloudy/Bloody Protein (Pleural/Serum) < 0.5 > 0.5 LDH (Pleural/Serum) < 0.6 > 0.6 LDH (Pleural) < 2/3 ULN Serum > 2/3 ULN Serum Causes CCF, Cirrhosis, Nephrotic Pneumonia, TB, Malignancy -
📌 Light's Criteria (Exudate if $\ge \mathbf{1}$):
- Pleural fluid protein / Serum protein > 0.5 (i.e., $P_{prot}/S_{prot} > \mathbf{0.5}$)
- Pleural fluid LDH / Serum LDH > 0.6 (i.e., $P_{LDH}/S_{LDH} > \mathbf{0.6}$)
- Pleural fluid LDH > 2/3 ULN Serum LDH (i.e., $P_{LDH} > \frac{2}{3} \times \text{ULN Serum LDH}$)
⭐ India: Commonest transudate - CCF. Commonest exudate - TB/Parapneumonic.
- Dx:
- CXR: Costophrenic angle blunting (~200 mL), meniscus. Lateral decubitus (~50 mL).
- USG: Sensitive (detects ~5-20 mL), guides thoracentesis.
- Thoracentesis: Diagnostic (biochem, cytology, micro) & therapeutic.
Effusion Varieties - The Usual Suspects
-
Parapneumonic Effusion & Empyema: Associated with pneumonia.
- Uncomplicated: Free-flowing; pH >7.2, Gluc >60 mg/dL, LDH <1000 IU/L. Rx: Antibiotics.
- Complicated: Loculated OR pH <7.2, Gluc <60 mg/dL, LDH >1000 IU/L. Rx: ICD + antibiotics.
- Empyema: Pus; +ve Gram/Culture. Rx: ICD, fibrinolytics (e.g. streptokinase), surgery if needed (decortication).
- 📌 Stages: 1. Exudative → 2. Fibrinopurulent → 3. Organising.

-
Tuberculous Pleural Effusion: Common extrapulmonary TB.
- Exudative, straw-coloured; lymphocytes >80%.
- ADA >40 IU/L highly suggestive. Pleural biopsy if doubt. Rx: ATT (6 months).
⭐ Adenosine Deaminase (ADA) >40 IU/L is a key diagnostic marker for tuberculous pleural effusion, especially in high TB prevalence areas.
-
Malignant Pleural Effusion: Primary (mesothelioma) or metastases (lung, breast, lymphoma).
- Large, recurrent, often hemorrhagic. Dx: Cytology/pleural biopsy.
- Rx: Therapeutic tap, pleurodesis (talc), IPC.
Air & Agony - Pneumothorax Puzzles
-
Types & Features:
Type Cause Key Feature Spontaneous - Primary (PSP) Ruptured subpleural bleb/bulla Young, tall, thin males; smokers - Secondary (SSP) Underlying lung disease (e.g., COPD) More severe symptoms Traumatic Penetrating/blunt trauma, iatrogenic History of trauma/procedure Tension Air entry > air exit (one-way valve) Life-threatening; shock -
Tension Pneumothorax: Medical emergency!
- 📌 TRACHEA Mnemonic: Tracheal deviation (away), Respiratory distress (severe), Absent breath sounds (ipsilateral), Cyanosis, Hypotension, Engorged neck veins (JVD), Acute.
- Immediate needle decompression: 2nd ICS mid-clavicular line OR 5th ICS mid-axillary line, then Intercostal Drain (ICD).

⭐ Tension pneumothorax is a clinical diagnosis; immediate needle thoracostomy should precede radiographic confirmation if suspected due to its life-threatening nature.
Other Pleural Pathologies - Thoracic Troubles
- Hemothorax: Blood in pleural space.
- Causes: Trauma, iatrogenic, malignancy.
- Dx: Pleural Hct > 0.5 × blood Hct.
- Rx: Chest tube; thoracotomy if >1500mL initial or >200mL/hr for 2-4 hrs.
- Chylothorax: Chyle (lymph) in pleural space.
- Causes: Trauma (surgical), malignancy (lymphoma).
- Dx: Milky fluid; ↑Triglycerides (>110 mg/dL), chylomicrons.
- Rx: Treat cause, low-fat/MCT diet, octreotide.
- Mesothelioma: Pleural malignancy.
- 📌 Risk: Asbestos exposure (primary).
- Imaging: Unilateral effusion, rind-like pleural thickening.
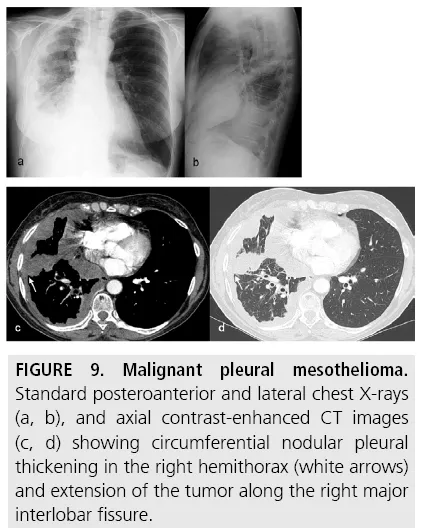
⭐ Strongly linked to occupational asbestos exposure; long latency (20-40 yrs).
- Light's criteria are crucial for differentiating exudative from transudative pleural effusions.
- Tuberculous pleural effusion is typically exudative, lymphocyte-predominant, with high ADA (>40 U/L).
- Malignant pleural effusion is often exudative, hemorrhagic, and cytology is key for diagnosis.
- Empyema requires drainage (thoracostomy); characterized by pus or positive Gram stain/culture.
- Pneumothorax types: spontaneous (primary/secondary), traumatic, tension (medical emergency, needle decompression).
- Mesothelioma is strongly associated with asbestos exposure; presents with pleural thickening/effusion.
- Chylothorax shows milky fluid with high triglycerides (>110 mg/dL) and cholesterol/triglyceride ratio <1.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

