Intro to Radiotherapy - Zap That Tumor!
- Principle: Uses ionizing radiation (photons or particles) to induce lethal DNA damage in cancer cells, minimizing harm to normal tissue.
- Intents: Curative (definitive), Adjuvant (post-op), Neoadjuvant (pre-op), Palliative (symptom relief).
- Radiation Types:
- Photons (X-rays, γ-rays): Most common; deep tissue penetration.
- Particles (electrons, protons, neutrons): Electrons for superficial lesions (e.g., skin, keloids).
- Units:
- Absorbed Dose: Gray (Gy). $1 \text{ Gy} = 1 \text{ J/kg}$.
- Equivalent Dose: Sievert (Sv) (accounts for biological effectiveness).
- Mechanism: Direct action (DNA strand breaks) & Indirect action (free radical formation from water radiolysis).
⭐ Indirect action, via hydroxyl radicals (•OH), accounts for ~2/3 of DNA damage by X-rays.
Radiobiology - Cells Under Fire
- The 4 R's (Fractionated Radiotherapy):
- Repair: Sublethal damage repair (SLDR), esp. in normal tissues.
- Redistribution: Surviving cells progress to more sensitive cycle phases.
- Repopulation: Cell proliferation between fractions (normal & tumor).
- Reoxygenation: Improved oxygenation of hypoxic tumor cells, ↑radiosensitivity.
- Cell Cycle Sensitivity:
- Most Sensitive: M (Mitosis), G2 phases.
- Most Resistant: Late S phase (higher repair).
- 📌 Order (Sensitive→Resistant): M > G2 > G1 > S.
- Oxygen Effect:
- $O_2$ presence significantly ↑ radiation damage (free radical fixation).
- Oxygen Enhancement Ratio (OER): Ratio of doses (hypoxic / aerobic) for isoeffect.
- OER (X-rays/γ-rays): Typically 2.5-3.5.
⭐ Hypoxic tumor cells are a major cause of radioresistance; OER for X-rays is typically 2.5-3.5.

Delivery Techniques - Precision Strikes
- External Beam RT (EBRT): Radiation from external source.
- 2D RT: Basic, X-ray guided, large margins.
- 3D-CRT: CT-planned, conforms to tumor.
- IMRT (Intensity-Modulated RT): Highly conformal, varied beam intensity. Spares OARs. 📌 IMRT: I M Really Targeting.
- VMAT (Volumetric Modulated Arc Therapy): Rotational IMRT; faster delivery.
- IGRT (Image-Guided RT): On-board imaging (e.g., CBCT) for accuracy.
- Stereotactic RT:
- SRS (Radiosurgery): Single high dose, intracranial.
- SBRT/SABR (Ablative): 1-5 fractions, high dose, extracranial.
- Particle Therapy: Protons (Bragg peak), Carbon ions (↑RBE).
- Brachytherapy: Internal source, rapid dose fall-off due to inverse square law ($I \propto 1/d^2$).
⭐ Brachytherapy's efficacy hinges on this rapid dose fall-off: high tumor dose, sharp gradient, spares normal tissue.
- Types: Intracavitary, Interstitial, Surface.
- Dose Rates: LDR (0.4-2 Gy/hr), HDR (>12 Gy/hr), PDR.
Toxicity & Management - The Aftermath
- Acute Toxicity (within 90 days of RT):
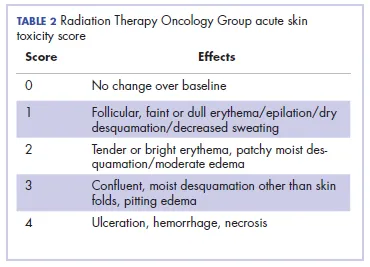
- Skin: Erythema, dry/moist desquamation.
- Mucositis (oral, GI), esophagitis.
- Systemic: Fatigue, nausea/vomiting.
- Bone marrow suppression (site-dependent).
- Late Toxicity (> 90 days post-RT, often irreversible):
- Fibrosis, necrosis (e.g., osteoradionecrosis).
- Organ-specific: Pneumonitis, proctitis, cystitis, myelopathy, xerostomia.
- Secondary malignancies (long-term risk).
- Endocrine dysfunction.
- Management Principles:
- Grading: Common Terminology Criteria for Adverse Events (CTCAE) / RTOG scales.
- Supportive care: Analgesia, antiemetics, hydration, nutrition.
- Specific agents: Amifostine (radioprotector), sucralfate, topical steroids.
- Radiation Recall: Inflammatory reaction in previously irradiated field upon new chemotherapy.
⭐ Lhermitte's sign: Electric shock-like sensation down the spine on neck flexion, indicates transient radiation myelopathy (usually resolves spontaneously within months).
High‑Yield Points - ⚡ Biggest Takeaways
- Radiosensitivity: High in lymphoid, bone marrow, gonads; low in nerve, muscle.
- Teletherapy (external) & brachytherapy (internal) are main radiation delivery methods.
- Fractionation exploits the 4 R's: Repair, Repopulation, Reoxygenation, Redistribution.
- Gray (Gy) is the SI unit of absorbed dose; 1 Gy = 100 rads.
- Acute effects (mucositis, dermatitis) within 90 days; late effects (fibrosis) after.
- OER is ~3 for X-rays; hypoxic cells radioresistant.
- Goal: Max tumor kill, min normal tissue toxicity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


