Intro & Mechanisms - Cancer's Covert Ops
- Systemic disorders triggered by cancer, not due to direct tumor invasion, metastasis, or side effects of therapy.
- Caused by tumor-secreted hormones, peptides, cytokines, or aberrant immune responses.
- Common Mechanisms:
- Ectopic hormone/peptide production (e.g., ACTH, ADH).
- Immune cross-reactivity: Antibodies or T-cells against tumor also target normal tissues.
- Cytokine release (e.g., TNF-α, IL-6) leading to systemic inflammation/cachexia.
⭐ Paraneoplastic syndromes can be the first manifestation of an underlying malignancy, often preceding cancer diagnosis by months or years.
Endocrine Syndromes - Hormone Hijack
- SIADH (Hyponatremia): Ectopic ADH secretion.
- Associated with: Small Cell Lung Cancer (SCLC), CNS disorders, drugs.
- Clinical: ↓Na+, ↓serum osmolality, ↑urine osmolality.
- Cushing's Syndrome: Ectopic ACTH secretion.
- Associated with: SCLC, pancreatic cancer, bronchial carcinoids.
- Clinical: HTN, hyperglycemia, hypokalemia, muscle weakness, central obesity.
- Hypercalcemia: PTHrP (PTH-related peptide) most common; also ectopic PTH, calcitriol.
- Associated with: Squamous cell (lung, head/neck), renal, breast, ovarian cancer.
- Clinical: "Stones, bones, groans, thrones, psychiatric overtones".
- Hypoglycemia: Ectopic Insulin or IGF-2.
- Associated with: Fibrosarcoma, mesenchymal tumors, hepatocellular carcinoma.
- Carcinoid Syndrome: Serotonin, bradykinin.
- Associated with: Metastatic carcinoid tumors (bronchial, GI).
- Clinical: Flushing, diarrhea, bronchospasm, right-sided heart valve lesions.
- Polycythemia: Ectopic erythropoietin.
- Associated with: Renal cell carcinoma, hepatocellular carcinoma, hemangioblastoma.
⭐ Small Cell Lung Cancer (SCLC) is notorious for causing SIADH (hyponatremia) and ectopic ACTH production (Cushing's syndrome).
 Word count: 98
Word count: 98
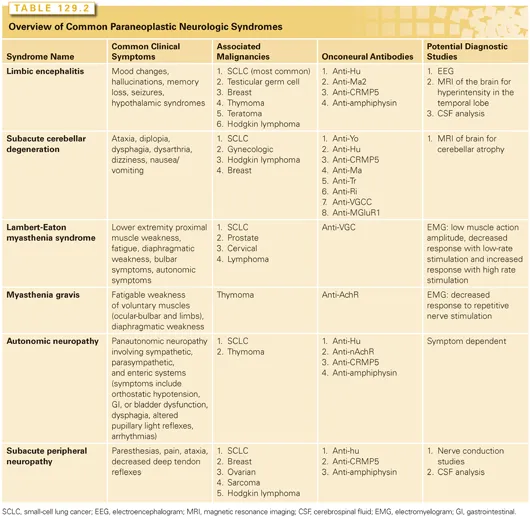
Neurological Syndromes - Nervous System Mayhem
- Central Nervous System (CNS):
- Limbic Encephalitis: Confusion, seizures, memory loss. Assoc: SCLC (Anti-Hu), testicular (Anti-Ma2).
- Paraneoplastic Cerebellar Degeneration: Ataxia, dysarthria. Assoc: Ovarian/Breast (Anti-Yo), Hodgkin (Anti-Tr), SCLC (Anti-Hu).
- Opsoclonus-Myoclonus Syndrome: "Dancing eyes, dancing feet". Assoc: Neuroblastoma (children), SCLC/Breast (adults, Anti-Ri).
- Brainstem Encephalitis: Cranial neuropathies, gaze palsies.
- Peripheral Nervous System & Neuromuscular Junction (NMJ):
- Lambert-Eaton Myasthenic Syndrome (LEMS):
⭐ Associated with SCLC, classically presents with proximal muscle weakness that improves with repeated muscle contraction. (📌 LEMS: Lungs, Exercise-improves, Myasthenic Syndrome)
- Antibodies: Voltage-gated Ca²⁺ channels (VGCC).
- Myasthenia Gravis: Fluctuating weakness, worse with exertion. Assoc: Thymoma. Antibodies: AChR.
- Peripheral Neuropathy: Sensory, motor, or mixed. Often painful.
- Stiff-Person Syndrome: Muscle rigidity, spasms. Assoc: Breast Ca, SCLC (Anti-amphiphysin), GAD Ab.
- Lambert-Eaton Myasthenic Syndrome (LEMS):

Other Key Syndromes - Systemic Shenanigans
- Hematological:
- Trousseau's syndrome (migratory thrombophlebitis): Pancreas, Lung
- Granulocytosis (↑WBCs): Lung, GI (G-CSF mediated)
- Eosinophilia: Hodgkin lymphoma
- Pure red cell aplasia: Thymoma
- NBTE (marantic endocarditis): AdenoCa (mucinous)
- Dermatological:
- Leser-Trélat sign (abrupt seborrheic keratoses): GI adenoCa
- Dermatomyositis/Polymyositis: Ovary, Lung, GI, Lymphoma
- Sweet's syndrome (acute febrile neutrophilic dermatosis): AML
- Necrolytic migratory erythema: Glucagonoma
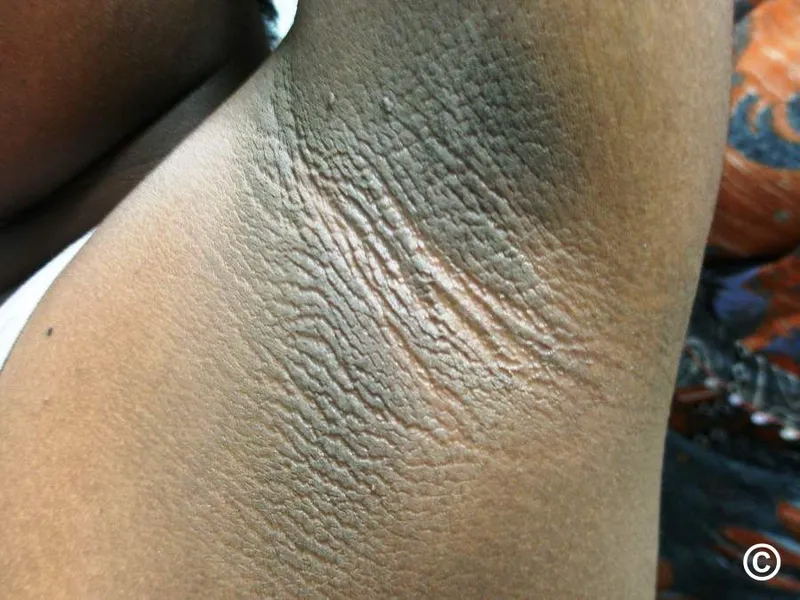
⭐ Acanthosis nigricans in a non-obese adult, especially with rapid onset and extensive involvement, strongly suggests an underlying GI adenocarcinoma.
- Rheumatological:
- Hypertrophic osteoarthropathy (HOA; clubbing, periostitis): Lung (NSCLC)
- Palmar fasciitis & polyarthritis ("puffy hand syndrome"): Ovary, Breast
Diagnosis & Management - Cracking the Case
- Diagnostic Approach
- High suspicion; rule out mimics (metastasis, metabolic, infection).
- Tests: Paraneoplastic antibody panels (anti-Hu, Yo, Ri), imaging (CT, PET-CT) for occult tumor.
- Management Strategy
- Primary: Treat underlying cancer (curative intent if possible).
- Adjunctive: Symptomatic relief; immunosuppression (steroids, IVIG, PLEX) for autoimmune types.
⭐ The definitive treatment for most paraneoplastic syndromes is successful treatment of the underlying cancer.
High‑Yield Points - ⚡ Biggest Takeaways
- SCLC: Key for SIADH (hyponatremia), ectopic ACTH (Cushing's), LEMS.
- Squamous cell lung ca: Produces PTHrP, leading to hypercalcemia.
- LEMS: Anti-presynaptic Ca2+ channels; weakness improves with activity.
- MG: Anti-postsynaptic AChR; linked to thymoma; weakness worsens with activity.
- Acanthosis nigricans: Velvety skin plaques; strong association with gastric/GI adenocarcinoma.
- Dermatomyositis/Polymyositis: High risk of underlying occult malignancy (ovarian, lung, GI).
- Hypertrophic Osteoarthropathy (HOA): Digital clubbing, periostitis; frequently linked to lung cancer.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

