Heme Malignancies Overview - Blood Cell Chaos
- Cancers of blood, bone marrow, lymphoid system; uncontrolled proliferation of abnormal hematopoietic/lymphoid cells.
- Broadly classified by:
- Cell Lineage: Myeloid (affecting RBCs, granulocytes, monocytes, platelets) vs. Lymphoid (affecting lymphocytes).
- Maturity & Onset:
- Acute: Rapid progression, immature cells (blasts). WHO defines AML/ALL with ≥20% blasts in marrow/blood.
- Chronic: Slower progression, more differentiated cells.
- Common presentations: Cytopenias (anemia, infections, bleeding), B-symptoms (fever, night sweats, weight loss), organomegaly.
- Diagnosis: CBC, peripheral smear, bone marrow aspiration & biopsy, immunophenotyping, cytogenetics, molecular studies.
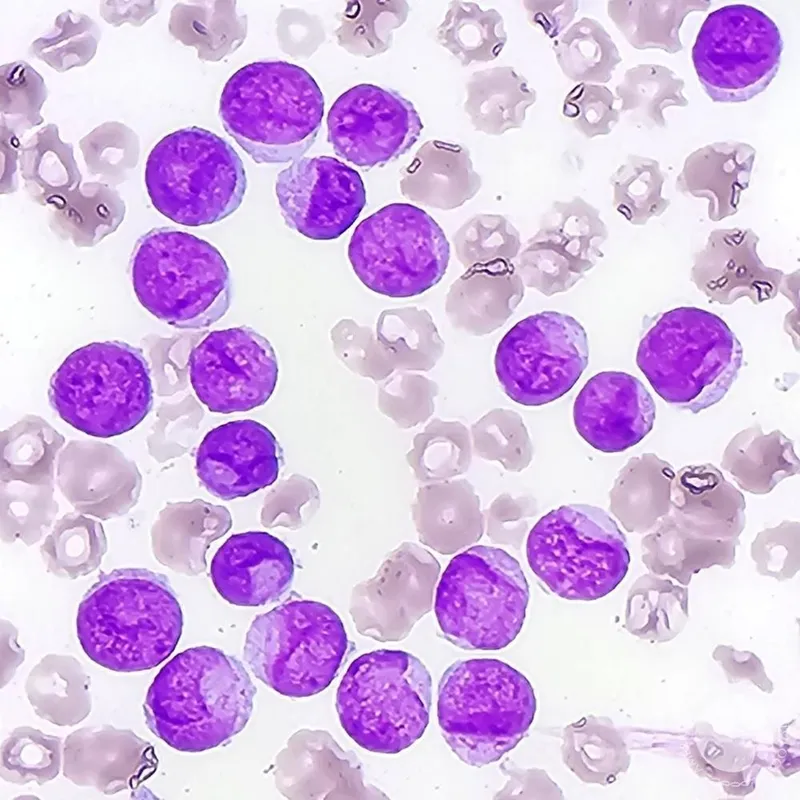
⭐ Auer rods (needle-like granules in cytoplasm) are pathognomonic for Acute Myeloid Leukemia (AML), especially Acute Promyelocytic Leukemia (APML).
Leukemias Unmasked - Proliferation Pandemonium
Uncontrolled WBC precursor proliferation. Acute (>20% marrow blasts) vs. Chronic. Myeloid vs. Lymphoid origin.
- AML (Acute Myeloid Leukemia): Adults. Auer rods (MPO+). 📌 Auer Makes Leukemia. APML t(15;17) responsive to ATRA. Gingival hypertrophy (M4/M5).
- ALL (Acute Lymphoblastic Leukemia): Children. TdT+. CNS prophylaxis crucial. Good prognosis. Philadelphia chr. t(9;22) variant = poor outcome.
- CML (Chronic Myeloid Leukemia): Adults. Hallmark: Philadelphia chr. t(9;22) (BCR-ABL1). TKIs mainstay. ↓LAP score. Blast crisis risk.
⭐ The Philadelphia chromosome t(9;22), creating BCR-ABL1 fusion, is pathognomonic for CML.
- CLL (Chronic Lymphocytic Leukemia): Elderly. Most common adult leukemia (West). Mature B-cells. Smudge cells on smear. Often indolent. Richter's transformation (DLBCL).

Lymphoma Lowdown - Nodal Nightmares
- Clonal proliferations of mature lymphocytes; nodal/extranodal.
- Hodgkin Lymphoma (HL):
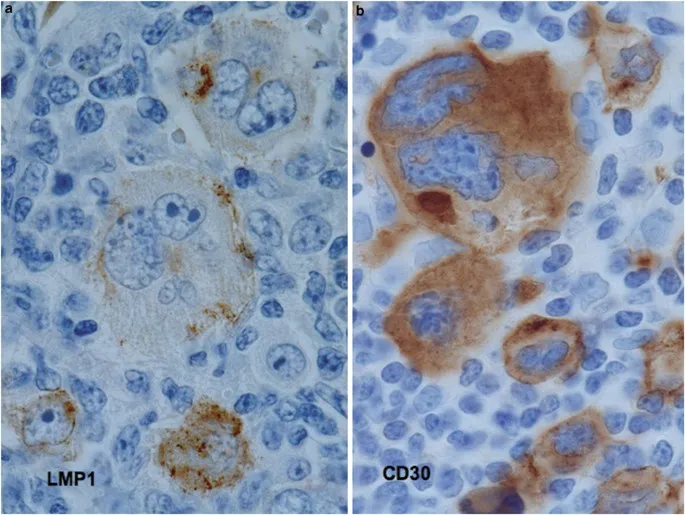
- Key: Reed-Sternberg (RS) cells (CD15+, CD30+).
- Age: Bimodal (15-35 & >50 yrs).
- Spread: Contiguous, orderly. Staging: Ann Arbor.
- Rx: ABVD regimen. Generally good prognosis.
- Non-Hodgkin Lymphoma (NHL):
- More common, diverse (B-cell ~85%, T-cell ~15%).
- Spread: Non-contiguous, often widespread at diagnosis.
- Types: Aggressive (e.g., DLBCL - Rx: R-CHOP) vs. Indolent (e.g., Follicular - t(14;18) BCL2).
⭐ Burkitt Lymphoma (NHL): "Starry sky" histology; t(8;14) c-MYC. Endemic (jaw), Sporadic (abdomen).
📌 B-Symptoms: Unexplained Fever >38°C, Drenching Night Sweats, Weight Loss >10% in 6 months.
Myeloma & MPN/MDS Mix - Marrow Madness Medley
-
Multiple Myeloma (MM): Malignant plasma cells in marrow.
- CRAB criteria: ↑Ca²⁺ (>11mg/dL), Renal insufficiency (CrCl <40mL/min), Anemia (Hb <10g/dL), Bone lesions (lytic).
- Myeloma Defining Events (MDEs): ≥60% marrow plasma cells, Serum Free Light Chain (FLC) ratio ≥100, >1 focal lesion on MRI.
- M-spike (IgG>IgA), Bence-Jones proteinuria. Rouleaux formation.

-
Myeloproliferative Neoplasms (MPN): Clonal myeloid cell overproduction.
- Key mutations: JAK2 V617F (Polycythemia Vera (PV) >95%; Essential Thrombocythemia (ET)/Primary Myelofibrosis (PMF) ~50%), CALR, MPL.
- PV: ↑RBC mass, ↓EPO. ET: ↑Platelets. PMF: Marrow fibrosis, splenomegaly, teardrop cells.
⭐ Philadelphia chromosome (t(9;22), BCR-ABL1) defines Chronic Myeloid Leukemia (CML), an MPN responsive to Tyrosine Kinase Inhibitors (e.g., Imatinib).
-
Myelodysplastic Syndromes (MDS): Ineffective hematopoiesis, cytopenias, marrow dysplasia.
- Risk of Acute Myeloid Leukemia (AML) transformation.
- Features: Pseudo-Pelger-Huët anomaly (bilobed neutrophils), ring sideroblasts.
- 5q- syndrome: specific subtype with isolated del(5q), good prognosis, Lenalidomide-sensitive.
High‑Yield Points - ⚡ Biggest Takeaways
- Hodgkin Lymphoma: Reed-Sternberg cells (CD15+, CD30+) are pathognomonic.
- Multiple Myeloma: Defined by CRAB criteria, M-spike, and Bence Jones proteins.
- CML: Philadelphia chromosome t(9;22) (BCR-ABL1) is characteristic; Imatinib is key therapy.
- AML: >20% blasts in bone marrow for diagnosis; Auer rods are specific.
- ALL: Most common childhood leukemia; lymphoblasts are TdT positive.
- CLL: Most common adult leukemia; features Smudge cells, potential Richter's transformation.
- Burkitt Lymphoma: Associated with EBV, t(8;14) (c-myc), shows starry sky histology.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

