Acute Stroke Management - Brain Attack Blitz
- Types: Ischemic (85%), Hemorrhagic (15%). 📌 FAST: Face, Arms, Speech, Time.
- NIHSS score: Quantifies deficit, guides therapy.
- Ischemic Stroke:
- tPA (Alteplase): Window <4.5 hrs. BP pre: <185/110 mmHg; post: <180/105 mmHg for 24h.
- Key tPA CIs: Active bleed, recent major surgery/trauma, uncontrolled HTN (BP >185/110 mmHg), platelets <100,000, INR >1.7.
- Mechanical Thrombectomy (MT): For Large Vessel Occlusion (LVO). Window <24 hrs.
- Hemorrhagic Stroke (ICH):
- Management: BP control (target SBP <140-160 mmHg), reverse anticoagulation.
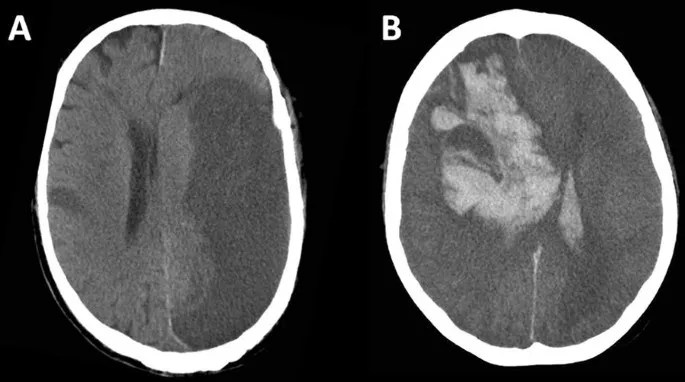
⭐ Permissive hypertension (up to 220/120 mmHg) is allowed in acute ischemic stroke if no tPA is given, to maintain cerebral perfusion. Stricter control post-tPA or in hemorrhagic stroke.
Seizure Emergencies - Thunderstorm Takedown
- Status Epilepticus (SE): Seizure ≥5 min OR ≥2 seizures without full recovery.
- Types: Convulsive, Non-convulsive.
- Initial (0-5 min): ABCs, IV access, O2, check glucose.
⭐ Always check and correct hypoglycemia in seizures/AMS; common reversible cause.
- Management Stages: 📌 LPM (Lorazepam, Phenytoin/Fosphenytoin, Midazolam/Propofol infusion)
- 1st Line (5-20 min): Benzodiazepines
- IV Lorazepam: 0.1 mg/kg (max 4mg).
- IM Midazolam: 10mg (if no IV).
- IV Diazepam: 0.15-0.2 mg/kg (max 10mg).
- 2nd Line (20-40 min): Non-BZD AEDs
- IV Fosphenytoin/Phenytoin: 20 mg/kg.
- IV Valproate: 20-40 mg/kg.
- IV Levetiracetam: 20-60 mg/kg.
- 3rd Line (>40-60 min): Refractory SE
- Anesthetic coma (Midazolam, Propofol, Pentobarbital).
- 1st Line (5-20 min): Benzodiazepines
CNS Infections - Cranial Invasion Control
- Acute Bacterial Meningitis (ABM):
- Triad: fever, nuchal rigidity, AMS (<50%). Kernig's/Brudzinski's.
- LP Contraindications: Raised ICP signs (papilledema, focal deficits, new seizure, GCS <11), coagulopathy.
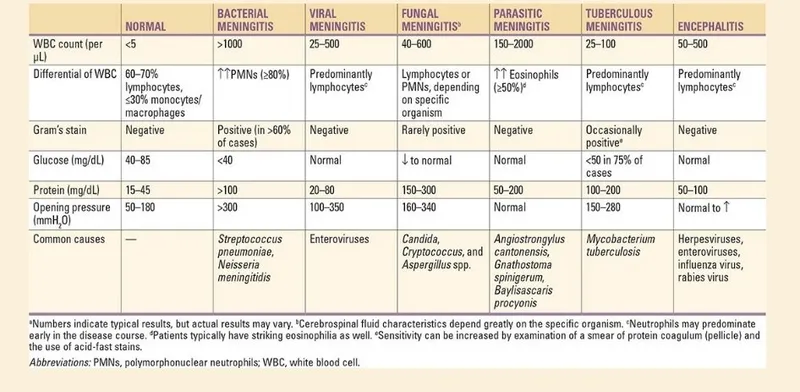
- CSF: OP >200-300 mmH2O; WBC >100-1000s (PMNs ↑); Glucose <40 mg/dL (↓); Protein >100-500 mg/dL (↑).
- Empirical Rx: Ceftriaxone + Vancomycin. Add Ampicillin (extremes age/immunocompromised for Listeria).
- Dexamethasone: 0.15 mg/kg IV Q6H x 4 days (before/with 1st antibiotic, esp. S. pneumoniae).
- 📌 CSF: Bacterial - PMNs & ↓sugar; Viral - Lymphocytes & normal sugar.
⭐ If LP delayed for CT in suspected ABM, give empirical antibiotics & dexamethasone post blood cultures.
Raised ICP & Cord Compression - Pressure Cooker & Cord Crisis
Raised Intracranial Pressure (ICP):
- Monro-Kellie doctrine. Causes: mass lesion, cerebral edema, hydrocephalus, venous obstruction.
- Clinical Features: headache, vomiting, papilledema, Altered Mental Status (AMS).
- Cushing's triad (late sign): ↑BP, ↓HR, irregular respirations. 📌 "High BP, Low HR, Funny RR".
- Management: Head elevation 30-45°, maintain CPP 60-70 mmHg ($CPP = MAP - ICP$). Hyperosmolar therapy (Mannitol 0.5-1 g/kg, Hypertonic Saline 3%). Controlled hyperventilation (PaCO2 30-35 mmHg - temporary bridge). CSF drainage, sedation/analgesia, decompressive craniectomy.
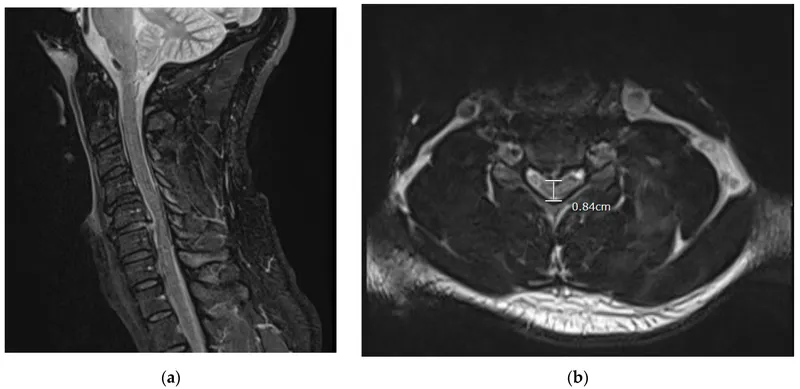
Acute Spinal Cord Compression:
- Causes: malignancy, trauma, epidural abscess/hematoma, disc herniation.
- Red Flags: severe back pain, progressive motor/sensory loss, sphincter dysfunction, saddle anesthesia.
- Management: STAT MRI. High-dose Dexamethasone (10mg IV bolus then 4-6mg Q6H). Urgent neurosurgical/oncological consult for decompression/radiotherapy.
⭐ In suspected acute spinal cord compression with neurological deficits, high-dose corticosteroids (e.g., Dexamethasone) should be administered immediately, even before definitive imaging, unless contraindicated.
High‑Yield Points - ⚡ Biggest Takeaways
- Status epilepticus: Benzodiazepines (e.g., lorazepam) first-line, then phenytoin/fosphenytoin.
- Acute Ischemic Stroke: IV alteplase within 4.5 hours; mechanical thrombectomy for LVO up to 24 hours.
- Subarachnoid Hemorrhage (SAH): Sudden "thunderclap headache"; non-contrast CT head is initial imaging; nimodipine prevents vasospasm.
- Bacterial Meningitis: Prompt empirical antibiotics and dexamethasone (especially for pneumococcal).
- Guillain-Barré Syndrome (GBS): Ascending paralysis and areflexia; treat with IVIG or plasmapheresis.
- Raised ICP: Management includes mannitol, hypertonic saline, head elevation; address underlying cause.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

