Brain Tumor Basics - Skull Invaders
- Primary (originate in CNS) vs. Secondary (metastases; commonest overall brain tumors).
- Commonest Primary Adult Tumors (WHO CNS5):
- Meningioma (most common overall primary, usually Grade 1-2)
- Glioblastoma, IDH-wildtype (Grade 4, most common primary malignant)
- Pituitary adenoma
- WHO 2021 Updates: Emphasizes molecular markers for classification & grading (CNS WHO Grades 1-4).
- Key Molecular Markers:
- IDH1/2 mutations: Better prognosis in gliomas.
- 1p/19q co-deletion: Hallmark of oligodendroglioma (Grade 2-3); predicts chemosensitivity & better prognosis.
- MGMT promoter methylation: In glioblastoma, predicts better response to temozolomide.
⭐ Glioblastoma (CNS WHO Grade 4) is the most common and most aggressive primary malignant brain tumor in adults. Despite its name, it rarely metastasizes outside the CNS.
Clinical Features - Brain's Distress Signals
- Raised Intracranial Pressure (ICP):
- Headache (worse morning/Valsalva), nausea/vomiting, papilledema.
- Cushing's triad (HTN, bradycardia, irregular respiration) - late, ominous.
- Altered sensorium, diplopia (CN VI palsy).
- Focal Neurological Deficits (FNDs) - Location Dependent:
- Frontal: Motor weakness, personality Δ, Broca's aphasia (dominant).
- Parietal: Sensory loss, neglect, apraxia.
- Temporal: Seizures, memory loss, Wernicke's aphasia (dominant).
- Occipital: Visual field defects (e.g., homonymous hemianopia).
- Cerebellum: Ataxia, dysmetria, nystagmus.
- Brainstem: Cranial nerve palsies, vital sign instability.
- Seizures:
- Common presenting symptom; often focal onset, may generalize.
- Headache Red Flags (📌 SNOOP4):
- Systemic symptoms, Neurologic deficits, Onset (sudden/new, esp. >50 yrs), Pattern change/Progressive/Papilledema/Positional/Precipitated by cough/Valsalva.
- Systemic symptoms, Neurologic deficits, Onset (sudden/new, esp. >50 yrs), Pattern change/Progressive/Papilledema/Positional/Precipitated by cough/Valsalva.
⭐ New-onset seizure in an adult is a brain tumor until proven otherwise.
Major Tumor Types - Rogues' Gallery
| Feature | Glioblastoma (GBM) | Meningioma | Metastases | Pituitary Adenoma |
|---|---|---|---|---|
| Typical Age | 50-70 yrs | 40-70 yrs (♀ > ♂) | >50 yrs | 30-50 yrs |
| Location | Cerebral hemispheres (frontal, temporal) | Dural attachment (parasagittal, convexity, sphenoid wing) | Grey-white junction, multiple | Sella turcica |
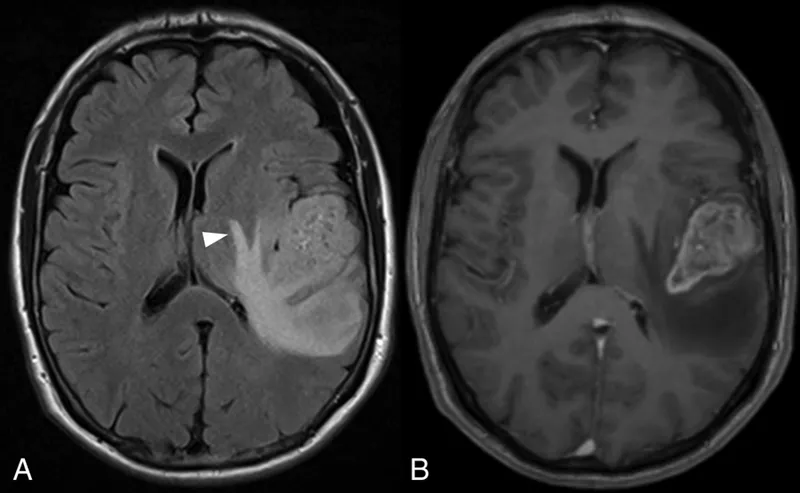
| Imaging Buzzwords | Butterfly glioma, ring-enhancing, central necrosis, peritumoral edema | Dural tail, homogeneously enhancing, extra-axial | Multiple, well-circumscribed, vasogenic edema | Snowman/figure-of-8 (suprasellar extension), sellar mass |
| Key Histology | Pseudopalisading necrosis, GFAP+, microvascular proliferation | Psammoma bodies, whorls, EMA+ | Mimics primary tumor; IHC for origin | Monomorphic cells, hormone stains (PRL, GH, ACTH) |
| Prognosis/Fact | Poor (median survival ~15 months); IDH mutation (better prognosis) | Usually benign (WHO Grade I); recurrence if incompletely resected | Primary: Lung, Breast, Melanoma, Renal, Colon | Functional vs. Non-functional; Bitemporal hemianopia |
Treatment Strategies - Counter Attack
Key goals: Maximize tumor control, preserve neurological function, maintain quality of life.
- Surgery:
- Maximal safe resection: Aim for gross total resection (GTR) if feasible.
- Obtain tissue for diagnosis.
- Relieve mass effect, ↓ Intracranial Pressure (ICP).
- Radiotherapy (RT):
- Types: External Beam RT (EBRT), Stereotactic Radiosurgery (SRS).
- Indications: Adjuvant post-surgery, primary for unresectable tumors, palliative.
- Chemotherapy:
- Temozolomide (TMZ): Standard for Glioblastoma (GBM).
- Steroids (e.g., Dexamethasone): Manage vasogenic edema. Dose: 4-8 mg IV/PO QID.
- PCV (Procarbazine, Lomustine, Vincristine) for certain oligodendrogliomas.
- Targeted Therapy:
- E.g., Bevacizumab (anti-VEGF) for recurrent GBM.
- Palliative Care: Integral for symptom management & QoL at all stages.
⭐ The "Stupp Protocol" for Glioblastoma involves concurrent Temozolomide and radiotherapy, followed by adjuvant Temozolomide, significantly improving median survival.
High‑Yield Points - ⚡ Biggest Takeaways
- Glioblastoma (GBM): Most common adult primary; butterfly glioma appearance.
- Pilocytic Astrocytoma: Most common pediatric primary; Rosenthal fibers, often cerebellar.
- Meningioma: Common in females; psammoma bodies, dural tail sign.
- Medulloblastoma: Malignant pediatric tumor (cerebellum); Homer Wright rosettes, radiosensitive.
- Ependymoma: Fourth ventricle (children), spinal cord (adults); perivascular pseudorosettes.
- NF2: Associated with bilateral acoustic schwannomas, multiple meningiomas, ependymomas.
- Metastases: Most common intracranial tumors overall; often from lung, breast, melanoma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

