Meningitis - Brain's Fiery Blanket
Meningeal inflammation: fever, headache, nuchal rigidity. Prompt Lumbar Puncture (LP) & treatment vital.
CSF Analysis: Key Differentiators
| Feature | Bacterial (Pyogenic) | Viral (Aseptic) | Tubercular (TBM) | Fungal (Crypto) |
|---|---|---|---|---|
| Appearance | Turbid | Clear | Fibrin web / Xanthochromic | Viscous, Clear/Turbid |
| Cells/µL (Type) | >1000 (PMN) | 10-1000 (Lymph) | 100-500 (Lymph early PMN) | 20-500 (Lymph) |
| Protein (mg/dL) | >100 (↑↑) | Normal/<100 (N/↑) | >100-500 (↑↑↑) | >45 (↑) |
| Glucose (mg/dL) | <40 (↓) ($CSF/BG < \mathbf{0.4}$) | Normal ($CSF/BG > \mathbf{0.6}$) | <45 (↓↓) ($CSF/BG < \mathbf{0.4}$) | <40 (↓) ($CSF/BG < \mathbf{0.4}$) |
| Specific Tests | Gram stain, Culture | PCR | AFB stain, GeneXpert, Culture | India Ink, Crypto Ag |
Empirical Antibiotics (Bacterial):
- Neonate (<1m): Ampicillin + Cefotaxime/Gentamicin.
- 1m-50y: Ceftriaxone + Vancomycin.
-
50y/ImmunoComp: Add Ampicillin.
⭐ Streptococcus pneumoniae: Most common bacterial cause in adults.
Complications: Hydrocephalus, cranial nerve palsies, seizures, hearing loss.
Encephalitis & Myelitis - Cord & Cortex Chaos
- Viral Encephalitis: Brain parenchyma inflammation.
- HSV-1: Commonest sporadic fatal encephalitis.
⭐ Predilection for temporal lobes (hemorrhagic necrosis).
- Rx: Acyclovir 10 mg/kg IV q8h for 14-21 days.
- Japanese Encephalitis (JE): Flavivirus; rural Asia. Vector: Culex.
- Features: Parkinsonism, dystonia, seizures, flaccid paralysis.
- Rabies: Lyssavirus; animal bites.
- Clinical: Hydrophobia, aerophobia, pharyngeal spasms.
- Pathology: Negri bodies (intracytoplasmic inclusions).
- HSV-1: Commonest sporadic fatal encephalitis.
- Acute Disseminated Encephalomyelitis (ADEM):
- Immune-mediated demyelination, post-infectious/post-vaccinial.
- Monophasic illness; encephalopathy common.
- MRI: Multiple, bilateral, asymmetric, large (>1-2 cm) white matter lesions.
- Transverse Myelitis (TM):
- Focal spinal cord segment inflammation.
- Clinical triad:
- Symmetric motor weakness (paraparesis).
- Clear sensory level.
- Sphincter dysfunction (urinary retention).
- Causes: Idiopathic, post-infectious, MS, NMO.
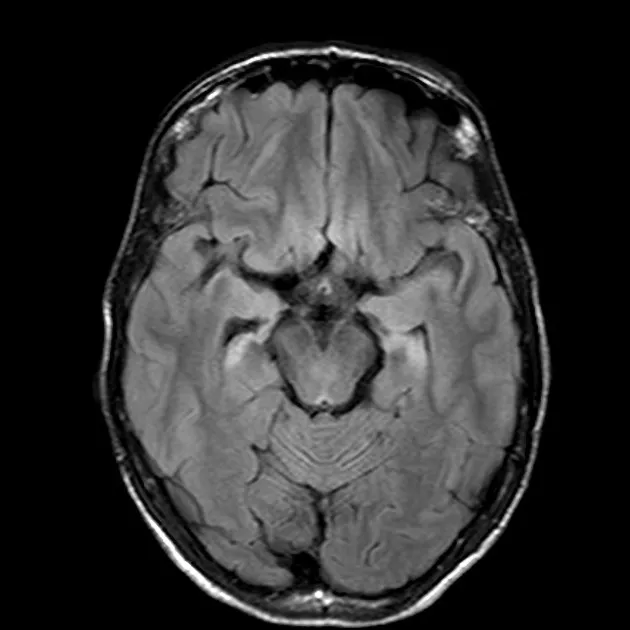
Focal CNS Suppurations - Pus Pockets Peril
- Brain Abscess: Localized CNS pus.
- Etiology: Direct spread (sinusitis, otitis, dental), hematogenous (lung, heart).
- Organisms: Streptococci, Staphylococci, anaerobes. Nocardia (immunocompromised).
- Imaging: Ring-enhancing lesion (CT/MRI).
⭐ Triad of brain abscess (fever, headache, focal neurological deficit) is seen in <50% cases.
- Subdural Empyema: Pus between dura & arachnoid. Rapid decline. Neurosurgical emergency.
- Epidural Abscess: Pus between dura & skull/vertebrae. Often spinal. Urgent.
- Management:
- Antibiotics: Empirical (e.g., Ceftriaxone + Metronidazole ± Vancomycin), then targeted.
- Surgical Drainage: Indicated if >2.5 cm, neurological compromise, or no improvement.
📌 Antibiotics, Brain imaging, Consult neurosurgery, Drainage if needed.
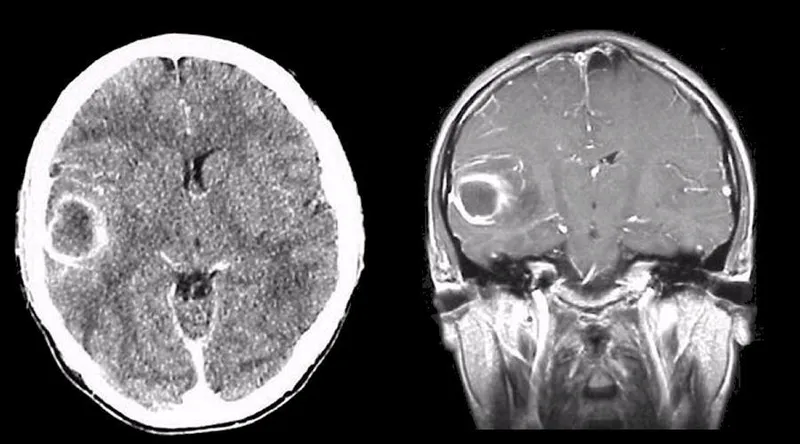
Chronic & Specific CNS Infections - Slow Burn Scourges
-
Neurocysticercosis (NCC):
- Etiology: Taenia solium larvae.
- Stages: Vesicular → colloidal → granular → calcified.
- Imaging: CT/MRI (cysts, edema, calcification).
- Rx: Albendazole; Steroids for inflammation.
⭐ Neurocysticercosis: most common parasitic CNS infection globally.
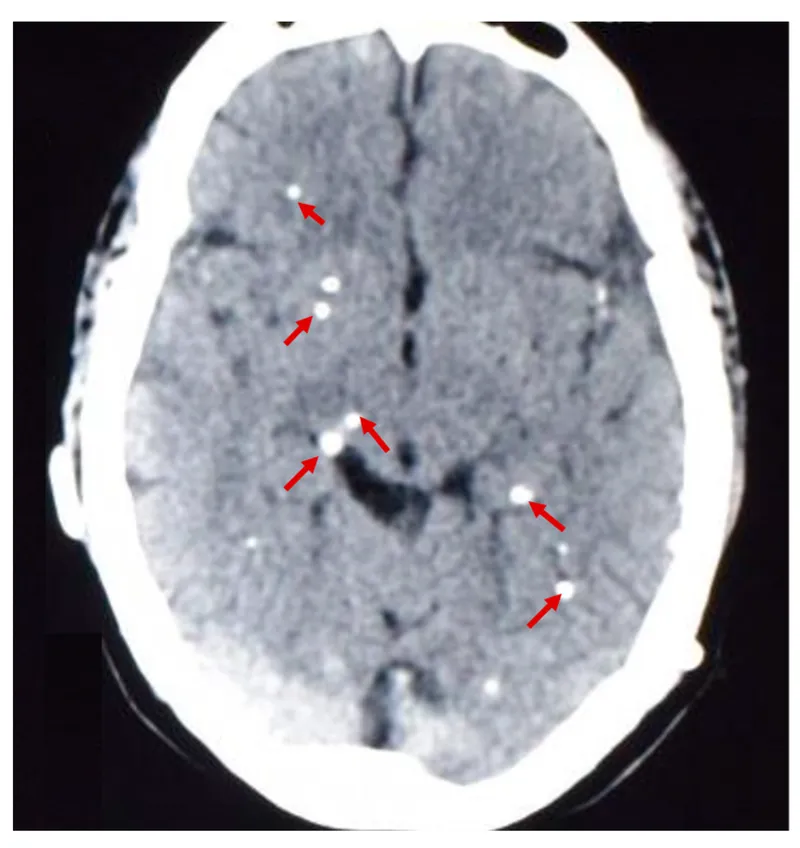
-
Neurosyphilis:
- Etiology: Treponema pallidum.
- Forms: Meningovascular (stroke-like), General Paresis (dementia), Tabes Dorsalis (sensory ataxia, Argyll Robertson pupil).
- Dx: CSF VDRL (specific).
-
Prion Diseases (e.g., CJD):
- Patho: Misfolded PrPSc.
- Features: Rapid dementia, myoclonus.
- Dx: EEG (periodic sharp waves), CSF (14-3-3 protein), MRI (DWI/FLAIR hyperintensities).
-
Progressive Multifocal Leukoencephalopathy (PML):
- Etiology: JC virus (reactivation).
- Risk: Immunocompromised (HIV, CD4 < 200/µL).
- MRI: Asymmetric, non-enhancing white matter lesions_._
High‑Yield Points - ⚡ Biggest Takeaways
- Bacterial meningitis CSF: Shows ↑Protein, ↓Glucose, ↑Neutrophils, and ↑Opening Pressure.
- Tuberculous meningitis CSF: Features ↓↓Glucose, ↑↑Protein, ↑Lymphocytes, ↑ADA, and cobweb coagulum.
- Viral meningitis CSF: Presents with ↑Lymphocytes, Normal Glucose, and Normal/Slightly ↑Protein.
- Cryptococcal meningitis: Common in HIV patients; India ink positive; markedly ↑Opening Pressure.
- Herpes Simplex Encephalitis (HSE): Temporal lobe involvement characteristic; treat with IV Acyclovir.
- Neurocysticercosis (NCC): Most common parasitic CNS infection; causes seizures; shows ring-enhancing lesions or calcified granulomas.
- Japanese Encephalitis: Viral cause; presents with extrapyramidal symptoms (parkinsonism); endemic areas.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

