Cerebral Circulation & Stroke Basics - Vascular Roadmap
- Key Arteries:
- Anterior Circulation: Internal Carotid Artery (ICA) → Anterior Cerebral Artery (ACA) & Middle Cerebral Artery (MCA).
- Posterior Circulation: Vertebral Arteries → Basilar Artery → Posterior Cerebral Artery (PCA).
- Circle of Willis: Anastomotic arterial ring at brain base; connects anterior & posterior systems.

- Stroke: Acute neurological deficit of vascular origin.
- Ischemic: Due to ↓ blood flow (e.g., thrombosis, embolism).
- Hemorrhagic: Due to bleeding.
- Transient Ischemic Attack (TIA): Brief episode of neurological dysfunction; no acute infarction; typically < 1 hour.
⭐ Most common artery involved in ischemic stroke is the Middle Cerebral Artery (MCA).
Ischemic Stroke - Clot Chaos
-
Patho: Arterial occlusion → focal brain ischemia; central core (irreversible infarct) vs. surrounding penumbra (salvageable tissue).
-
Etiology: Thrombotic (atherosclerosis), Embolic (e.g., AFib, valvular), Lacunar (small vessel, chronic HTN, DM).
-
Sx: Sudden focal deficit. 📌 FAST (Face, Arm, Speech, Time). Common syndromes: MCA, ACA, PCA, Vertebrobasilar.
-
Dx: NCCT (r/o bleed); MRI (DWI confirms); CTA/MRA (vascular occlusion).
-
Acute Management Algorithm:
⭐ The therapeutic window for IV thrombolysis (tPA) in acute ischemic stroke is typically <4.5 hours from symptom onset.
-
Key Meds: IV Alteplase. Aspirin 160-325mg (if no tPA, or 24h post-tPA). Statins.

Hemorrhagic Stroke - Bleed Breakdown
- Intracerebral Hemorrhage (ICH): Bleeding within brain parenchyma.
- Causes: Hypertension (commonest), AVMs, amyloid angiopathy.
- Sites: Basal ganglia, thalamus, pons, cerebellum.
- Management: BP control (SBP <140 mmHg), reverse anticoagulation, surgery if indicated.
- Subarachnoid Hemorrhage (SAH): Bleeding into subarachnoid space.
- Causes: Ruptured berry aneurysm (85%), AVM.
- Presentation: Sudden "thunderclap" headache.
- Dx: CT head; LP (xanthochromia if CT neg).
- Management: Nimodipine, secure aneurysm (coiling/clipping).

⭐ Subarachnoid Hemorrhage (SAH) classically presents with a sudden, severe "thunderclap" headache, often described as the "worst headache of my life".
TIA, Mimics & Diagnostics - Fleeting Shadows & Clear Views
- Transient Ischemic Attack (TIA): Focal neurological deficit, symptoms resolve typically <1 hour, no acute infarction on imaging.
- Key Mimics: Seizure, migraine aura, hypoglycemia, syncope, labyrinthitis.
- Diagnostics:
- Initial: Non-Contrast CT (NCCT) head to exclude hemorrhage.
- MRI Brain (especially DWI) confirms ischemia.
⭐ Diffusion-Weighted Imaging (DWI) on MRI is the most sensitive modality for detecting acute cerebral ischemia within minutes of onset.
- Vascular imaging (Carotid Doppler, CTA/MRA); Cardiac workup (ECG, Echo).
- Risk Stratification: 📌 ABCD2 Score:
- Age (≥60 years = 1 pt)
- Blood Pressure (≥140/90 mmHg = 1 pt)
- Clinical Features (Unilateral Weakness = 2 pts; Speech disturbance without weakness = 1 pt)
- Duration of symptoms (≥60 min = 2 pts; 10-59 min = 1 pt)
- Diabetes Mellitus (1 pt)
- Interpretation: Score 0-3 (low risk); 4-5 (moderate risk, consider hospitalization); ≥6 (high risk, urgent hospitalization).
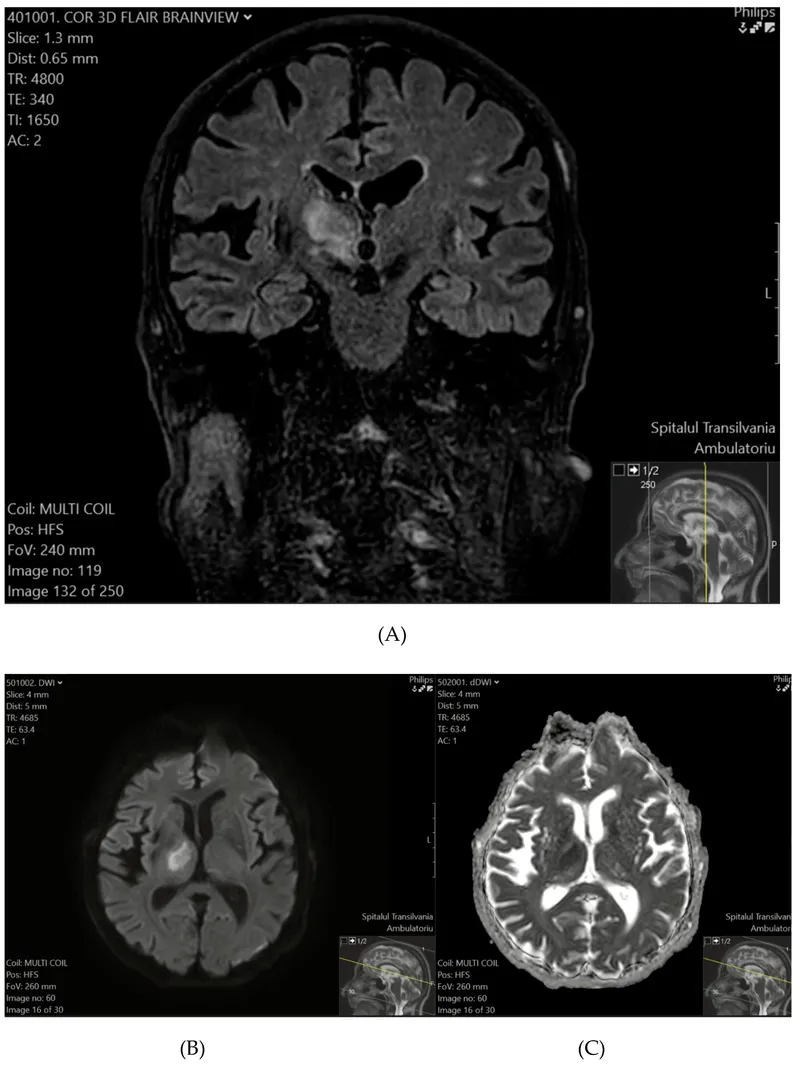
Brainstem Stroke Syndromes - Crossed Signs & Cranial Nerves
Brainstem strokes often present with characteristic crossed syndromes - ipsilateral cranial nerve deficits with contralateral motor/sensory deficits due to the compact anatomy of the brainstem.
Foville Syndrome & Millard-Gubler Syndrome
Both syndromes result from pontine lesions affecting the facial nerve nucleus/fascicle and corticospinal tract, but differ in their specific anatomical involvement:
| Feature | Foville Syndrome | Millard-Gubler Syndrome |
|---|---|---|
| Anatomical Location | Dorsal pons (tegmentum) | Ventral pons (base) |
| Cranial Nerves Affected | CN VI (abducens) + CN VII (facial) | CN VII (facial) only |
| Ipsilateral Signs | • Facial paralysis (CN VII) • Lateral gaze palsy (CN VI) • Possible hearing loss | • Facial paralysis (CN VII) |
| Contralateral Signs | • Hemiparesis • Hemisensory loss | • Hemiparesis |
| Key Distinguishing Feature | Lateral gaze palsy (cannot look toward lesion side) | No gaze palsy |
| Vascular Territory | Paramedian pontine branches | Paramedian pontine branches |
| Clinical Mnemonic | "Foville = Facial + gaze Failure" | "Millard = just Motor + facial" |
- Weber Syndrome (Midbrain): Ipsilateral CN III palsy + contralateral hemiparesis
- Benedikt Syndrome (Midbrain): Ipsilateral CN III palsy + contralateral tremor/ataxia
- Wallenberg Syndrome (Lateral medulla): Ipsilateral facial sensory loss + contralateral body sensory loss + ataxia
⭐ Key Clinical Pearl: In brainstem strokes, the presence or absence of gaze palsy is crucial for differentiating Foville syndrome (gaze palsy present) from Millard-Gubler syndrome (gaze palsy absent).
Stroke Sequelae & Prevention - Road to Recovery
- Common Sequelae: Motor deficits (hemiparesis), sensory loss, aphasia, cognitive impairment, depression, spasticity, dysphagia.
- Secondary Prevention:
- Antiplatelets (e.g., aspirin, clopidogrel).
- Statins (target LDL < 70 mg/dL).
- Strict BP control (target < 130/80 mmHg).
- Diabetes management (HbA1c < 7%).
- Lifestyle changes: diet, exercise, smoking cessation.
⭐ For patients with ischemic stroke or TIA and atrial fibrillation, long-term anticoagulation (e.g., with DOACs or warfarin) is crucial for secondary prevention.
- Rehabilitation: Multidisciplinary approach including physiotherapy, occupational therapy, and speech therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- MCA stroke is most common: contralateral weakness/sensory loss, aphasia (dominant), neglect (non-dominant).
- Lacunar infarcts: small, deep; pure motor/sensory deficits; linked to hypertension.
- SAH: "worst headache of life"; berry aneurysm rupture; xanthochromia in CSF.
- Ischemic stroke: IV thrombolysis (alteplase) within 4.5 hrs; thrombectomy up to 24 hrs for large vessel occlusion.
- TIA: transient deficit <1 hr, no infarct; high stroke risk (use ABCD2 score).
- Key modifiable risk factors: Hypertension, diabetes, atrial fibrillation, smoking.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

