Kidney Stones: Types & Risks - Stone Cold Facts
-
Types & Radiopacity:
- Calcium Oxalate (≈80%): Radiopaque. Risks: ↓Fluids, ↑Oxalate/Na/Animal protein, hypercalciuria, hypocitraturia.
- Struvite (MAP) (≈10-15%): Staghorn, radiopaque. Risks: UTI (urease+ (Proteus)), alkaline urine.
- Uric Acid (≈5-10%): Radiolucent. Risks: Gout, acidic urine, ↑purines.
- Cystine (≈1-2%): Faintly radiopaque. Risks: Cystinuria, acidic urine.
-
Major Risk Factors:
- ↓ Fluid intake (primary).
- Diet: ↑Oxalate, ↑Sodium, ↑Animal protein.
- Family Hx, metabolic (e.g., hyperpara).
⭐ Most common kidney stones are Calcium Oxalate (≈80%); key dietary risk factor is low fluid intake & high oxalate/sodium/animal protein diet.
Kidney Stones: Clinical Picture & Diagnosis - Symptom & Scan
- Symptoms (Clinical Picture):
- Renal Colic: Severe, acute, intermittent flank pain.
- Radiation: "Loin to groin", testes/labia.
- Hematuria: Gross or microscopic; common (~90%).
- Nausea/Vomiting: Common.
- Irritative Voiding: Dysuria, urgency, frequency (stone at VUJ/bladder).
- Fever/Chills: Suspect infection (obstructive pyelonephritis = emergency!).
- Renal Colic: Severe, acute, intermittent flank pain.
- Diagnosis (Investigations & Scans):
- Urinalysis: Hematuria, pyuria, crystals, pH.
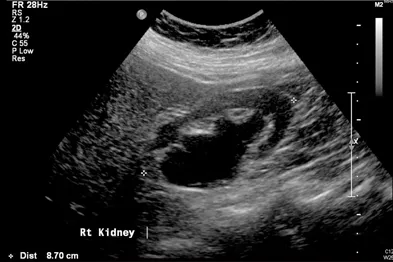
- Imaging:
- USG KUB: First-line in pregnancy & children. Detects hydronephrosis, stones.
- X-ray KUB: Shows radio-opaque stones (Calcium, Struvite). Limited for small/lucent stones.
- ⭐ > Non-contrast CT (NCCT) KUB is the gold standard. Highly sensitive for most stones (except pure indinavir). Details size, location, density (HU).
Kidney Stones: Management Strategies - Crush & Conquer
- Conservative:
- Analgesia (NSAIDs), Hydration (>2.5L/day).
- Medical Expulsive Therapy (MET): For stones <10mm (e.g., Tamsulosin 0.4mg).
- Interventions (Size/Symptom-Driven):
- ESWL: Renal stones <2cm, proximal ureteric <1cm.
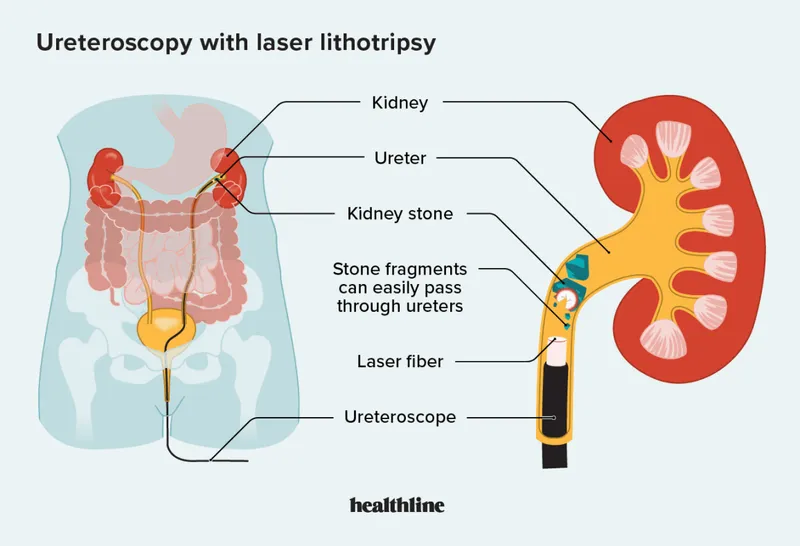
- URS: Ureteric stones, smaller renal stones; laser lithotripsy.
- PCNL: Large stones >2cm, staghorn, complex, lower pole.
- Open surgery: Rare.
- Specific Stone Management:
- Uric Acid: Allopurinol, K-citrate (urine pH 6.5-7.0).
- Struvite: Antibiotics, complete removal (often PCNL).
- Cystine: ↑Fluids, D-penicillamine/Tiopronin, K-citrate (urine pH >7.5).
⭐ For stones <10mm likely to pass, Medical Expulsive Therapy (MET) with alpha-blockers (e.g., Tamsulosin) is often used. Stones >2cm or complex staghorn calculi often require PCNL.
Obstructive Uropathy: Causes, Effects & Fixes - Flow Failures
Blockage to urine flow from calyces to urethra.
- Causes:
- Intrinsic: Stones, tumors, strictures, BPH.
- Extrinsic: Retroperitoneal fibrosis, external tumors, pregnancy.
- Functional: Neurogenic bladder.
- Effects:
- ↑ Pressure → hydroureter/hydronephrosis.
- Prolonged: Tubular damage, fibrosis, ↓ GFR, atrophy.
- Complications: AKI, CKD, infection.
- Features: Pain (flank/suprapubic), anuria/oliguria, voiding issues.
- Diagnosis: Ultrasound (hydronephrosis), CT (level/cause), RFTs.
- Fixes: Relieve obstruction (catheter, PCN, stent), treat cause.
⭐ In elderly males, Benign Prostatic Hyperplasia (BPH) is the most common cause of bilateral hydronephrosis and post-renal acute kidney injury.
High‑Yield Points - ⚡ Biggest Takeaways
- Calcium oxalate: Most common kidney stone type.
- Struvite stones: Associated with UTIs (Proteus); form staghorn calculi.
- Uric acid stones: Radiolucent; manage with urine alkalinization.
- Cystine stones: Hexagonal crystals, genetic (autosomal recessive).
- Renal colic investigation: NCCT KUB is the investigation of choice.
- Obstructive uropathy: Leads to hydronephrosis and post-renal AKI.
- BPH: Common cause of bilateral urinary obstruction in older men.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

