CKD Basics - Kidney's Slow Fade
- Progressive, irreversible decline in kidney function.
- Diagnostic criteria (must persist ≥3 months):
- GFR < 60 $mL/min/1.73m^2$
- OR presence of kidney damage markers.
⭐ CKD is defined by chronicity (≥3 months) of either critically low GFR or evidence of kidney damage (e.g., albuminuria, structural issues).
- Key Kidney Damage Markers:
- Albuminuria: ACR ≥ 30 mg/g
- Urine sediment abnormalities
- Electrolyte/tubular disorders
- Structural abnormalities (imaging)
- History of kidney transplantation
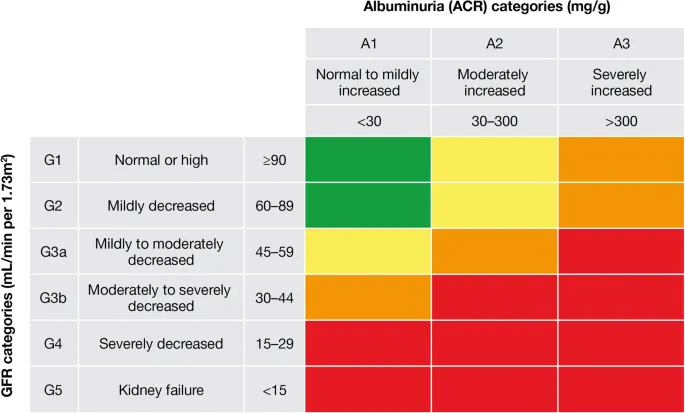
- Staging (KDIGO): GFR (G1-G5) & Albuminuria (A1-A3) categories.
CKD Culprits - Usual Suspects
⭐ Diabetes Mellitus (DM) and Hypertension (HTN) are overwhelmingly the two most common causes of CKD worldwide and in India, responsible for over two-thirds of cases.
- Other Significant Causes:
- Glomerulonephritis (GN): e.g., IgA nephropathy, FSGS.
- Polycystic Kidney Disease (ADPKD): Inherited cystic disorder.
- Chronic Tubulointerstitial Nephritis: From drugs (NSAIDs), infections, reflux.
- Obstructive Uropathy: Due to BPH, stones, strictures.
- Autoimmune Diseases: Systemic Lupus Erythematosus (SLE).
CKD Chaos - System Breakdown
- Key Progression Drivers: Vicious cycle of Glomerular hyperfiltration → Proteinuria → Tubulointerstitial inflammation & fibrosis (TGF-β mediated) → Further nephron loss. Intrarenal RAAS activation amplifies damage.
- Systemic Complications: 📌 A WET BED
- Acidosis (Metabolic)
- Water-Electrolyte Imbalance: ↑$K^+$, ↑$PO_4^{3-}$, ↓$Ca^{2+}$, Fluid overload
- EPO Failure: Anemia
- Toxin Accumulation: Uremia (encephalopathy, pericarditis, coagulopathy)
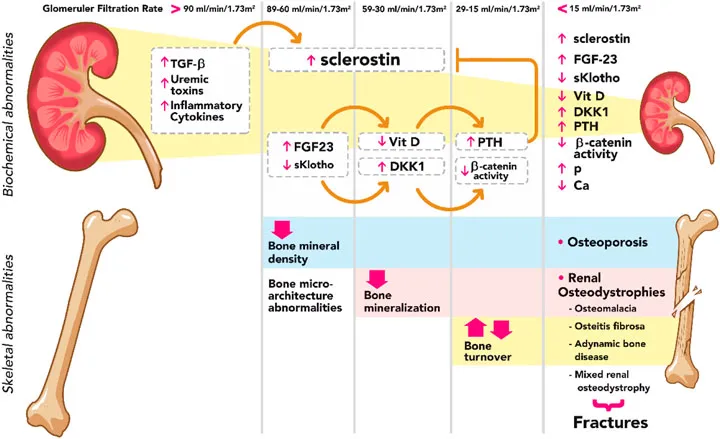
- Bone Disease (CKD-MBD): ↓Active Vit D, ↑PTH, ↑FGF23. Target PTH 150-300 pg/mL (Stage 5D)
- Endocrine: Insulin resistance, ↓ T4 to T3 conversion
- Dyslipidemia: ↑Triglycerides
⭐ Anemia in CKD is primarily due to decreased erythropoietin (EPO) production by the failing kidneys.
CKD Clues - Spotting Signs
- Clinical Features:
- Early: Often asymptomatic.
- Progressive: Fatigue, edema, HTN.
- Advanced (Uremia): Nausea, vomiting, pruritus, encephalopathy.
- Key Investigations:
- eGFR: Persistent ↓ <60 ml/min/1.73m² for >3 months ($MDRD$/$CKD-EPI$).
- Albuminuria (Urine ACR): A1 (<30mg/g), A2 (30-300mg/g), A3 (>300mg/g).
- Renal USG: Small, echogenic kidneys (exceptions: PCKD, diabetic).
- Labs: Anemia, ↑$K^+$, ↑$PO_4^{3-}$, ↓$Ca^{2+}$.
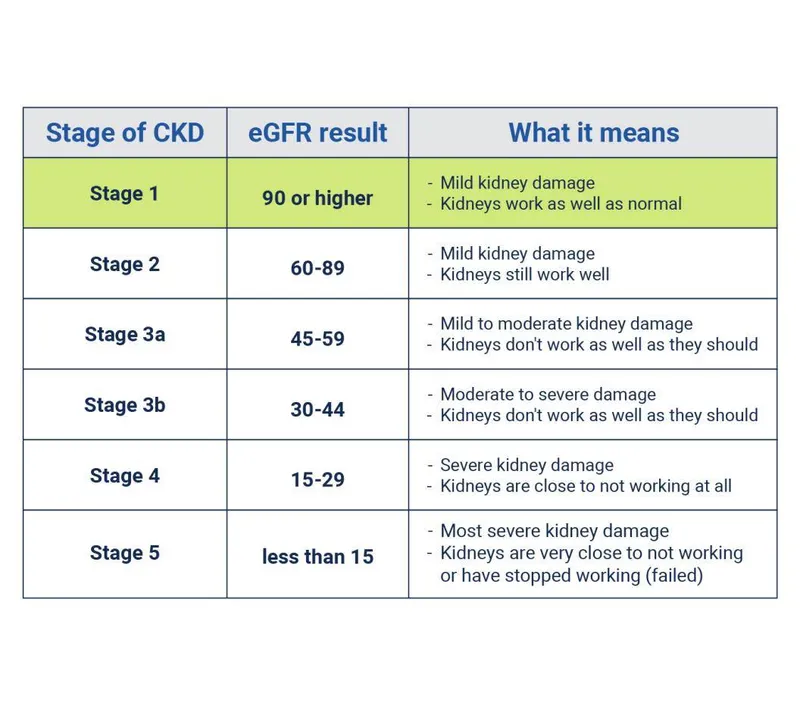
⭐ Urine Albumin-to-Creatinine Ratio (ACR) is a key investigation for detecting and monitoring kidney damage in CKD, and for risk stratification.
CKD Combat - Holding Line
- Goals: Slow progression, manage complications, RRT prep.
- Slow Progression:
- BP: <130/80 mmHg.
- RAASi: ACEi/ARB (esp. albuminuria).
⭐ ACE inhibitors or ARBs are recommended for most patients with CKD, especially those with albuminuria, to slow disease progression and reduce cardiovascular risk.
- Glucose: HbA1c <7%; SGLT2i.
- Lifestyle: ↓Protein, ↓Na, ↓K, ↓P; stop smoking.
- Manage Complications:
- Anemia: Hb 10-11.5 g/dL (Iron, ESAs).
- CKD-MBD: ↓PO₄, Vit D.
- Acidosis: NaHCO₃.
- RRT Prep:
- AV fistula (eGFR <20-25 $mL/min/1.73m^2$).
High‑Yield Points - ⚡ Biggest Takeaways
- CKD: GFR < 60 mL/min/1.73m² for > 3 months or kidney damage.
- Top causes: Diabetes Mellitus, Hypertension.
- Complications: Anemia (↓EPO), CKD-MBD (↑PO₄, ↓Ca, ↑PTH), metabolic acidosis, hyperkalemia.
- ESRD (End-Stage Renal Disease) is GFR < 15 mL/min/1.73m² (Stage G5).
- Manage by slowing progression, treating anemia (ESAs, iron) & CKD-MBD (phosphate binders, Vit D).
- Broad waxy casts in urine sediment suggest advanced CKD.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

