International and Global Health

On this page
🌍 Global Health Architecture: The Planetary Medicine Blueprint
You'll explore how nations coordinate to detect outbreaks before they cross borders, enforce binding health regulations that function as a global constitution, and deploy targeted initiatives against diseases that respect no passport. This lesson reveals the architecture behind planetary medicine-from surveillance networks that serve as humanity's early warning system to programs strengthening health infrastructure and protecting mothers and children in resource-limited settings. You'll understand not just what these systems do, but why coordinated global action often means the difference between contained threats and worldwide crises.
📌 Remember: GLOBAL - Governance systems, Low-income focus, Outbreak prevention, Border-crossing diseases, Access equity, Lifelong population health

The World Health Organization coordinates health responses across 6 regional offices, managing 13,000+ staff members in 150+ countries. Global health initiatives target the 17 Sustainable Development Goals, with specific focus on reducing maternal mortality by 75%, child mortality by 67%, and achieving 90% vaccination coverage by 2030.
- Primary Global Health Actors
- WHO: 194 member states, annual budget $6.12 billion, coordinates 150+ health emergencies annually
- GAVI Alliance: Immunized 822 million children, prevented 14.4 million deaths, operates in 73 countries
- Global Fund: Invested $50+ billion, saved 44 million lives, fights 3 major diseases
- Malaria programs: $15.8 billion invested, 1.5 billion bed nets distributed
- TB programs: $9.2 billion invested, 5.4 million lives saved
- HIV programs: $19.8 billion invested, 17.5 million on treatment
⭐ Clinical Pearl: Countries with <$1,000 per capita health spending show 5-10x higher maternal mortality rates (>300 per 100,000) compared to high-income nations (<10 per 100,000), demonstrating the direct correlation between health system investment and outcomes.
| Organization | Annual Budget | Countries Served | Primary Focus | Lives Impacted | Success Metric |
|---|---|---|---|---|---|
| WHO | $6.12 billion | 194 | Disease surveillance | 7.8 billion | Emergency response time |
| GAVI | $4.3 billion | 73 | Immunization | 822 million children | Vaccination coverage |
| Global Fund | $4.2 billion | 120+ | HIV/TB/Malaria | 44 million saved | Mortality reduction |
| PEPFAR | $6.9 billion | 50+ | HIV/AIDS | 20 million on treatment | Treatment access |
| USAID | $27 billion | 100+ | Development aid | 1+ billion | Health outcomes |
The global disease burden demonstrates stark inequalities: low-income countries experience 60% higher disability-adjusted life years (DALYs) per capita, with communicable diseases accounting for 40% of total burden compared to <5% in high-income nations. Non-communicable diseases now represent 71% of global deaths (41 million annually), requiring coordinated international responses.

Understanding global health architecture provides the foundation for examining specific disease control mechanisms and international cooperation frameworks that enable coordinated planetary health responses.
🌍 Global Health Architecture: The Planetary Medicine Blueprint
⚡ Disease Surveillance Networks: The Global Early Warning System
📌 Remember: DETECT - Disease monitoring, Early warning systems, Threat assessment, Emergency response, Cross-border coordination, Technology integration
The International Health Regulations (2005) mandate that 196 countries develop core surveillance capacities, including 24/7 emergency operations centers, laboratory networks capable of identifying priority pathogens within 24-48 hours, and rapid response teams deployable within 72 hours of outbreak detection.
- Global Surveillance Architecture
- WHO Global Outbreak Alert and Response Network (GOARN): 500+ institutions, 24/7 monitoring, 150+ technical partners
- Global Influenza Surveillance Network: 144 National Influenza Centers, 6 WHO Collaborating Centers, monitors 300,000+ specimens annually
- Laboratory Network: 59 WHO Collaborating Centers, 144 National Reference Labs, 1,500+ sentinel sites
- Pathogen identification: <24 hours for priority diseases
- Genetic sequencing: <48 hours for novel variants
- International sharing: <72 hours via GISAID platform

⭐ Clinical Pearl: The R0 threshold of 1.3 triggers international concern for respiratory pathogens, while case fatality rates >10% combined with human-to-human transmission automatically qualify for Public Health Emergency of International Concern (PHEIC) consideration under IHR protocols.
| Surveillance System | Coverage | Response Time | Detection Capacity | Annual Cost | Success Rate |
|---|---|---|---|---|---|
| GOARN | 196 countries | <24 hours | 1,400+ pathogens | $500 million | 95% detection |
| FluNet | 144 centers | <48 hours | Influenza variants | $50 million | 98% coverage |
| GLASS | 87 countries | Weekly | AMR patterns | $25 million | 85% reporting |
| EBS | 100+ countries | Real-time | Event-based signals | $100 million | 90% sensitivity |
| PolioPLUS | 200+ countries | <72 hours | Poliovirus | $150 million | 99.9% reduction |
💡 Master This: Digital disease detection now identifies outbreaks 2-3 weeks earlier than traditional surveillance through social media monitoring, search engine queries, and mobile phone data, revolutionizing global health security response times and enabling preemptive interventions.

Effective surveillance networks create the foundation for understanding how international health regulations coordinate global responses to emerging threats.
⚡ Disease Surveillance Networks: The Global Early Warning System
🚨 International Health Regulations: The Global Health Constitution
📌 Remember: RESPOND - Rapid detection, Emergency operations, Surveillance systems, Point of entry controls, Outbreak investigation, Notification protocols, Decision instruments
The Decision Instrument Algorithm provides systematic criteria for determining whether events constitute Public Health Emergencies of International Concern (PHEIC). Since 2005, 6 PHEICs have been declared, affecting 4.2 billion people and mobilizing $47 billion in international response funding.
- IHR Core Capacity Requirements
- Surveillance Systems: 24/7 reporting capacity, <24-hour notification for urgent events, epidemiological investigation within 48 hours
- Laboratory Networks: Biosafety Level 2 minimum, pathogen identification within 24-48 hours, specimen transport within 72 hours
- Emergency Response: National emergency operations center, rapid response teams, risk communication protocols
- Response team deployment: <72 hours domestic, <7 days international
- Resource mobilization: $50-100 million emergency funding available
- Communication reach: 80%+ population within 24 hours
⭐ Clinical Pearl: Article 12 requires countries to notify WHO within 24 hours of events that may constitute PHEICs, with Article 15 mandating immediate information sharing for events involving novel pathogens, antimicrobial resistance, or international spread potential.
| PHEIC Declaration | Year | Duration | Countries Affected | Response Cost | Lives Saved |
|---|---|---|---|---|---|
| H1N1 Pandemic | 2009 | 14 months | 214 countries | $18.5 billion | 200,000+ |
| Polio Resurgence | 2014 | Ongoing | 3 countries | $2.8 billion | 1.8 million |
| Ebola West Africa | 2014 | 22 months | 10 countries | $12.1 billion | 11,000+ |
| Zika Virus | 2016 | 9 months | 84 countries | $1.8 billion | Unknown |
| Ebola DRC | 2019 | 11 months | 4 countries | $1.6 billion | 2,200+ |
| COVID-19 | 2020 | Ongoing | 195 countries | $16+ trillion | Millions |
💡 Master This: Points of Entry (PoE) regulations require designated airports and ports to maintain public health emergency contingency plans, isolation facilities, and 24/7 qualified personnel, with 319 designated PoE worldwide managing 4.5 billion annual international travelers.

Understanding IHR frameworks enables examination of how global health initiatives address specific disease burdens and population health challenges.
🚨 International Health Regulations: The Global Health Constitution
🎯 Global Disease Control Initiatives: The Planetary Health Offensive
📌 Remember: IMPACT - Immunization programs, Malaria control, Prevention strategies, Access to treatment, Community engagement, Technology innovation
The Global Fund to Fight AIDS, Tuberculosis and Malaria represents the largest disease-specific financing mechanism, investing $50+ billion since 2002, saving 44 million lives, and reducing combined deaths from the three diseases by 46% in supported countries.
- HIV/AIDS Global Response
- PEPFAR Program: $85+ billion invested, 20 million people on treatment, 2.5 million babies born HIV-free
- UNAIDS 95-95-95 Targets: 95% diagnosed, 95% on treatment, 95% virally suppressed by 2030
- Global Coverage: 28.7 million on antiretroviral therapy, 1.5 million new infections annually (down from 3.2 million in 1997)
- Treatment access: 75% of people living with HIV globally
- Mother-to-child transmission: <2% in high-coverage programs
- AIDS-related deaths: 690,000 annually (down from 1.9 million peak)
⭐ Clinical Pearl: Treatment as Prevention (TasP) demonstrates that achieving viral load <50 copies/mL reduces transmission risk by >96%, making universal test and treat strategies both therapeutic and preventive interventions with population-level impact.
| Disease Initiative | Annual Investment | Countries | Population Reached | Lives Saved | Reduction Target |
|---|---|---|---|---|---|
| Global Fund | $4.2 billion | 120+ | 1.8 billion | 44 million | 46% mortality |
| PEPFAR | $6.9 billion | 50+ | 20 million | 21 million | 75% incidence |
| GAVI Alliance | $4.3 billion | 73 | 822 million children | 14.4 million | 90% coverage |
| Malaria Control | $3.1 billion | 87 | 2.3 billion | 7.6 million | 75% incidence |
| TB Partnership | $1.3 billion | 134 | 58 million treated | 63 million | 90% reduction |
💡 Master This: Vaccine-preventable disease control through GAVI Alliance has achieved 86% global coverage for DTP3, preventing 4-5 million deaths annually, with new vaccine introductions (rotavirus, pneumococcal, HPV) adding $150 billion in economic benefits through 2030.
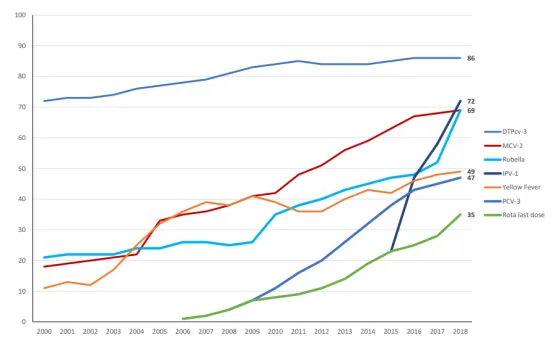
Successful disease control initiatives provide models for addressing emerging health challenges through coordinated international responses and sustainable health system strengthening.
🎯 Global Disease Control Initiatives: The Planetary Health Offensive
🏥 Health Systems Strengthening: The Infrastructure Revolution
📌 Remember: BLOCKS - Building workforce capacity, Leadership and governance, Operations and service delivery, Commodities and technologies, Knowledge and information systems, Sustainable financing
The WHO Health Systems Framework identifies six building blocks requiring coordinated strengthening to achieve health outcomes, responsiveness, social and financial risk protection, and improved efficiency. Countries with strong health systems achieve 2-3x better health outcomes per dollar invested.
- Health Workforce Development
- Global Shortage: 18 million health workers needed by 2030, 70% in Africa and Southeast Asia
- Density Targets: 4.45 skilled health workers per 1,000 population for SDG achievement
- Training Scale-Up: 1 million additional health workers annually, $10 billion investment required
- Medical schools: 3,000+ institutions globally, 500,000 graduates annually
- Nursing programs: 5,000+ schools, 1.2 million graduates annually
- Community health workers: 5+ million deployed, target 10 million by 2030

⭐ Clinical Pearl: Countries with >2.5 health workers per 1,000 population achieve >80% skilled birth attendance and <50 maternal deaths per 100,000 births, demonstrating the direct correlation between workforce density and maternal health outcomes.
| Building Block | Investment Need | Current Gap | Target 2030 | Success Metric | ROI Estimate |
|---|---|---|---|---|---|
| Health Workforce | $10 billion | 18 million workers | 4.45 per 1,000 | Coverage rates | 9:1 |
| Service Delivery | $50 billion | 50% coverage | 90% UHC | Access equity | 7:1 |
| Health Information | $5 billion | 60% systems | 100% digital | Data quality | 12:1 |
| Medical Products | $25 billion | 30% access | 80% availability | Supply security | 8:1 |
| Health Financing | $200 billion | $371B total need | Sustainable funding | Financial protection | 4:1 |
| Leadership/Governance | $15 billion | Weak institutions | Strong governance | System performance | 15:1 |
💡 Master This: Primary Health Care strengthening yields highest return on investment (10:1 ratio), preventing 60-70% of premature deaths through basic interventions costing <$50 per person annually, making it the foundation strategy for achieving Universal Health Coverage.
Strong health systems create the platform for addressing specific population health challenges, particularly maternal and child health outcomes worldwide.
🏥 Health Systems Strengthening: The Infrastructure Revolution
👶 Maternal and Child Health: The Future Generation Imperative
📌 Remember: MOTHERS - Maternal mortality reduction, Optimal nutrition, Trained birth attendants, Health facility delivery, Emergency obstetric care, Reproductive health access, Skilled care coverage
Sustainable Development Goal 3 targets <70 maternal deaths per 100,000 births and <25 neonatal deaths per 1,000 births by 2030. Current global rates of 211 maternal deaths and 18 neonatal deaths require accelerated progress in 68 high-burden countries accounting for 95% of maternal and 90% of child deaths.
- Maternal Mortality Interventions
- Skilled Birth Attendance: 81% global coverage, target >90% by 2030
- Emergency Obstetric Care: 15 facilities per 500,000 population standard, 60% countries meet target
- Family Planning Access: 842 million women need contraception, 218 million unmet need
- Contraceptive prevalence: 63% globally, 24% in least developed countries
- Maternal deaths prevented: 308,000 annually with universal access
- Economic benefit: $7 return per $1 invested in family planning

⭐ Clinical Pearl: "Three delays model" identifies critical intervention points: delay in seeking care (33% of deaths), delay in reaching facility (25% of deaths), and delay in receiving care (42% of deaths), with skilled birth attendance reducing mortality by >50% when combined with emergency obstetric care.
| MCH Intervention | Global Coverage | Target 2030 | Lives Saved Annually | Cost per Life Saved | ROI Ratio |
|---|---|---|---|---|---|
| Skilled Birth Attendance | 81% | 90% | 180,000 maternal | $1,400 | 12:1 |
| Emergency Obstetric Care | 60% | 80% | 115,000 maternal | $2,100 | 8:1 |
| Immunization (DTP3) | 86% | 95% | 4.5 million child | $50 | 44:1 |
| Exclusive Breastfeeding | 44% | 70% | 820,000 child | $35 | 35:1 |
| ORS for Diarrhea | 47% | 80% | 525,000 child | $15 | 60:1 |
💡 Master This: Nutrition interventions during the first 1,000 days (pregnancy through age 2) prevent 45% of child deaths, with exclusive breastfeeding for 6 months reducing diarrhea by 50% and respiratory infections by 36%, making nutrition the highest-impact MCH intervention.
Maternal and child health improvements create the foundation for examining how global health initiatives address health equity and access challenges across diverse populations.
👶 Maternal and Child Health: The Future Generation Imperative
🎯 Global Health Mastery: The Planetary Care Command Center
📌 Remember: MASTERY - Multi-sector coordination, Access equity, Surveillance integration, Technology leverage, Evidence-based policy, Resource optimization, Yield measurement
- Essential Global Health Arsenal
- Surveillance Metrics: R0 <1.0 for outbreak control, <24-hour detection time, >95% reporting completeness
- Health System Indicators: >4.45 health workers per 1,000, >90% service coverage, <10% out-of-pocket spending
- Disease Control Targets: 95-95-95 for HIV, <10 cases per 100,000 for TB, <1 case per 1,000 for malaria
- Maternal mortality: <70 per 100,000 births
- Child mortality: <25 per 1,000 births
- Vaccination coverage: >90% for all antigens
⭐ Clinical Pearl: Health security preparedness requires $1-2 per person annually but yields $7-10 return through pandemic prevention, making global health investment one of the highest-ROI public policy interventions for economic stability and human development.
| Global Health Domain | Success Threshold | Current Global Status | Investment Required | Expected ROI | Timeline |
|---|---|---|---|---|---|
| Disease Surveillance | 95% detection <24h | 75% average | $2 billion annually | 15:1 | 2025 |
| Health Systems | 90% UHC coverage | 68% average | $200 billion annually | 7:1 | 2030 |
| Disease Control | 75% mortality reduction | 45% average | $15 billion annually | 12:1 | 2030 |
| Emergency Preparedness | 100% IHR compliance | 35% average | $7 billion annually | 10:1 | 2027 |
| Health Equity | <2x mortality ratio | 5-10x current | $50 billion annually | 8:1 | 2035 |
Pattern Recognition for Global Health Mastery: When you see outbreak reports, think surveillance system performance; when you see health inequities, think system strengthening needs; when you see cross-border spread, think international coordination requirements; when you see resource constraints, think innovative financing mechanisms; when you see population health challenges, think multi-sectoral approaches combining clinical care, public health, and social determinants interventions.
🎯 Global Health Mastery: The Planetary Care Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























