Sepsis and Septic Shock - Sepsis Unmasked
- Sepsis: A syndrome of life-threatening organ dysfunction caused by a dysregulated host response to infection.
- Organ dysfunction: Acute ↑ in Sequential Organ Failure Assessment (SOFA) score by ≥2 points.
- qSOFA (Quick SOFA, suspect sepsis if ≥2 criteria met):
- Respiratory Rate (RR) ≥22/min
- Altered Mentation (Glasgow Coma Scale <15)
- Systolic Blood Pressure (SBP) ≤100 mmHg
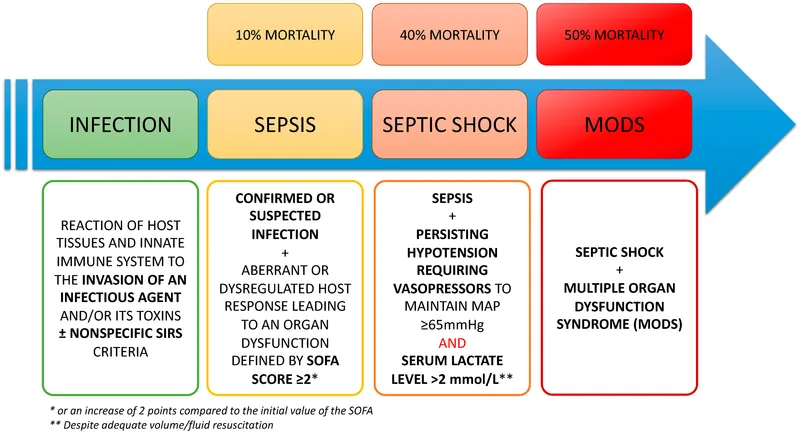
- Septic Shock: A subset of sepsis with critical increases in mortality due to severe circulatory, cellular, and metabolic abnormalities.
- Criteria: Persisting hypotension requiring vasopressors to maintain Mean Arterial Pressure (MAP) ≥65 mmHg AND serum lactate level >2 mmol/L despite adequate fluid resuscitation.
- Pathogenesis: Infection triggers inflammatory cascade (cytokine storm) → endothelial dysfunction, vasodilation, microvascular thrombosis, and coagulopathy → tissue hypoperfusion → multi-organ dysfunction syndrome (MODS).
⭐ Early recognition and prompt initiation of the "Hour-1 Bundle" (including lactate measurement, blood cultures, broad-spectrum antibiotics, rapid fluid administration, and vasopressors if hypotensive) significantly improves outcomes in sepsis and septic shock.
Sepsis and Septic Shock - Spotting the Enemy
- Suspect with known/presumed infection + signs of new organ dysfunction.
- Screening (qSOFA): 📌 HAT (Hypotension, Altered Mental Status, Tachypnoea)
- Respiratory Rate (RR) $\ge$ 22/min
- Altered Mentation (e.g., GCS < 15)
- Systolic BP (SBP) $\le$ 100 mmHg
- Score $\ge$ 2 suggests sepsis; prompts full SOFA assessment.
- Sepsis (Sepsis-3): Suspected infection + acute increase in total SOFA score $\ge$ 2 points.
- Septic Shock: Sepsis + (need for vasopressors to maintain MAP $\ge$ 65 mmHg) + (serum lactate > 2 mmol/L despite adequate fluid resuscitation).
- Initial Investigations: Serum lactate, blood cultures (before antibiotics, without delaying therapy), site-specific cultures, CBC, renal/liver function, coagulation panel, procalcitonin.
⭐ A serum lactate level > 2 mmol/L despite adequate fluid resuscitation is a critical criterion for defining septic shock and indicates tissue hypoperfusion.
Sepsis and Septic Shock - The Rescue Mission
Goals: Restore perfusion, treat infection, modulate host response.
Hour-1 Bundle (SSC Critical Actions):
- Measure lactate (remeasure if initial > 2 mmol/L).
- Blood cultures before antibiotics.
- Broad-spectrum antibiotics (promptly, within 1 hr).
- Rapid 30 mL/kg crystalloid for hypotension or lactate ≥ 4 mmol/L.
- Vasopressors if MAP < 65 mmHg despite adequate fluids.
Key Interventions:
- Vasopressors: NE 1st line. Add vasopressin or epinephrine if needed.
- Corticosteroids: IV hydrocortisone 200 mg/day for refractory shock.
- Ventilation (ARDS): Low tidal volume (6 mL/kg PBW), Pplat < 30 cm H2O.
- Glucose: Target < 180 mg/dL.
- Source Control: Identify & manage infection.
⭐ > Early appropriate antibiotics (within 1 hour of recognition) significantly reduce sepsis mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- Sepsis: Life-threatening organ dysfunction from dysregulated infection response.
- qSOFA (≥2 points): For high-risk sepsis (AMS, SBP ≤100 mmHg, RR ≥22/min).
- Septic Shock: Sepsis + hypotension (MAP <65 mmHg despite fluids) needing vasopressors + lactate >2 mmol/L.
- Hour-1 Bundle: Lactate, cultures, antibiotics, fluids, vasopressors for MAP ≥65 mmHg.
- Key Pathogens: S. aureus, Strep. pneumoniae, E. coli, Klebsiella.
- Norepinephrine: First-line vasopressor.
- Lactate: Crucial marker for hypoperfusion and prognosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

