HAIs Overview - Hospital's Hidden Foes
- Definition: Infections acquired in a healthcare setting, typically after ≥48 hours of admission, not present or incubating at admission.
- Common Types:
- Catheter-Associated Urinary Tract Infection (CAUTI)
- Central Line-Associated Bloodstream Infection (CLABSI)
- Ventilator-Associated Pneumonia (VAP)
- Surgical Site Infection (SSI)
- Clostridioides difficile Infection (CDI)
- Epidemiology (India): Significant burden; incidence varies (e.g., VAP 10-30% in ICUs).
- Overall Burden: ↑ morbidity, mortality, length of stay, healthcare costs.
⭐ CAUTI is the most common type of HAI globally and in India.
CAUTI & CLABSI - Invasive Line Invaders
- Pathogenesis: Biofilm formation on catheter (CAUTI); Migration of skin organisms, hub contamination (CLABSI).
- Common Organisms:
- CAUTI: E. coli, Klebsiella, Proteus, Enterococcus, Candida.
- CLABSI: Coagulase-negative staphylococci (CoNS), S. aureus, Gram-negative rods, Candida.
- Risk Factors: Prolonged catheterization (CAUTI >48h; CLABSI >2 calendar days), improper insertion/care, female (CAUTI), femoral/jugular sites (CLABSI).
- Diagnosis (CDC Criteria):
- CAUTI: Symptoms (fever, dysuria) + urine culture ≥$10^5$ CFU/mL (≤2 species) OR pyuria + ≥$10^3$ CFU/mL if catheter removed within 48h.
- CLABSI: Recognized pathogen from ≥1 blood culture OR common commensal from ≥2 blood cultures (separate occasions) + symptoms (fever, chills), with CVC in place ≥2 days.
- Key Prevention: Hand hygiene, aseptic insertion, daily review of necessity, prompt removal when no longer indicated.
⭐ The single most effective measure to prevent CAUTI is limiting catheter use and ensuring prompt removal when no longer indicated.

Prevention Bundles Comparison: CAUTI vs. CLABSI
| Prevention Element | CAUTI | CLABSI (📌 HANDS Mnemonic) |
|---|---|---|
| Hand Hygiene | ✅ Before/after manipulation | ✅ Before insertion/manipulation |
| Aseptic Insertion | Sterile technique, closed drainage system | ✅ Maximal barrier precautions |
| Skin Prep/Site Sel. | Perineal cleansing before insertion | ✅ Chlorhexidine skin prep, optimal site |
| Daily Review | ✅ Catheter necessity, drainage patency | ✅ Line necessity, site integrity |
| Secure/Removal | Secure catheter, prompt removal | ✅ Secure line, prompt removal |
VAP & SSI - Surgical & Airy Afflictions
- Ventilator-Associated Pneumonia (VAP)
- Pathogenesis: Microaspiration of oropharyngeal/gastric flora. Occurs >48h post-intubation.
- Organisms: Pseudomonas aeruginosa, Acinetobacter spp., Staphylococcus aureus (MRSA).
- Diagnosis: New/progressive pulmonary infiltrate + ≥2 clinical signs (fever >38°C, leukocytosis/leukopenia, purulent secretions). Clinical Pulmonary Infection Score (CPIS) > 6 highly suggestive.
- Prevention: Head-of-bed elevation 30-45°, oral care (chlorhexidine), daily sedation interruption & assessment of readiness to extubate. 📌 I COUGH.
- Surgical Site Infection (SSI)
- Pathogenesis: Contamination during surgery. Risk factors: obesity, diabetes, smoking, immunosuppression.
- Organisms: Staphylococcus aureus (most common), Coagulase-negative staphylococci, Enterococci, E. coli, Pseudomonas aeruginosa.
- Prevention: Pre-operative antibiotics (e.g., Cefazolin 30-60 min before incision; Vancomycin/Fluoroquinolones 60-120 min), appropriate hair removal, skin antisepsis, glycemic control (glucose <200 mg/dL).
- Classification:
Type Location Superficial Incisional Involves only skin & subcutaneous tissue Deep Incisional Involves deep soft tissues (e.g., fascia, muscle) Organ/Space Involves any organ/space opened during surgery

⭐ Staphylococcus aureus is the most common cause of SSIs, while Pseudomonas aeruginosa is a key pathogen in late-onset VAP (>5 days).
C. diff & MDR - Gut Wreckers & Drug Dodgers
- C. difficile Infection (CDI):
- Patho: Toxins A & B damage gut. Risk: Antibiotics (clindamycin, cephalosporins).
- Dx: Stool NAAT or GDH + Toxin assay.
- Tx (Initial, non-severe): Oral Vancomycin 125mg QID or Fidaxomicin 200mg BID for 10 days.
- High recurrence.
- Multidrug-Resistant Organisms (MDROs):
- Key types: MRSA, VRE, ESBLs, CRE.
- Implications: ↑morbidity, ↑hospital stays.
- Control: Hand hygiene, contact precautions, stewardship.
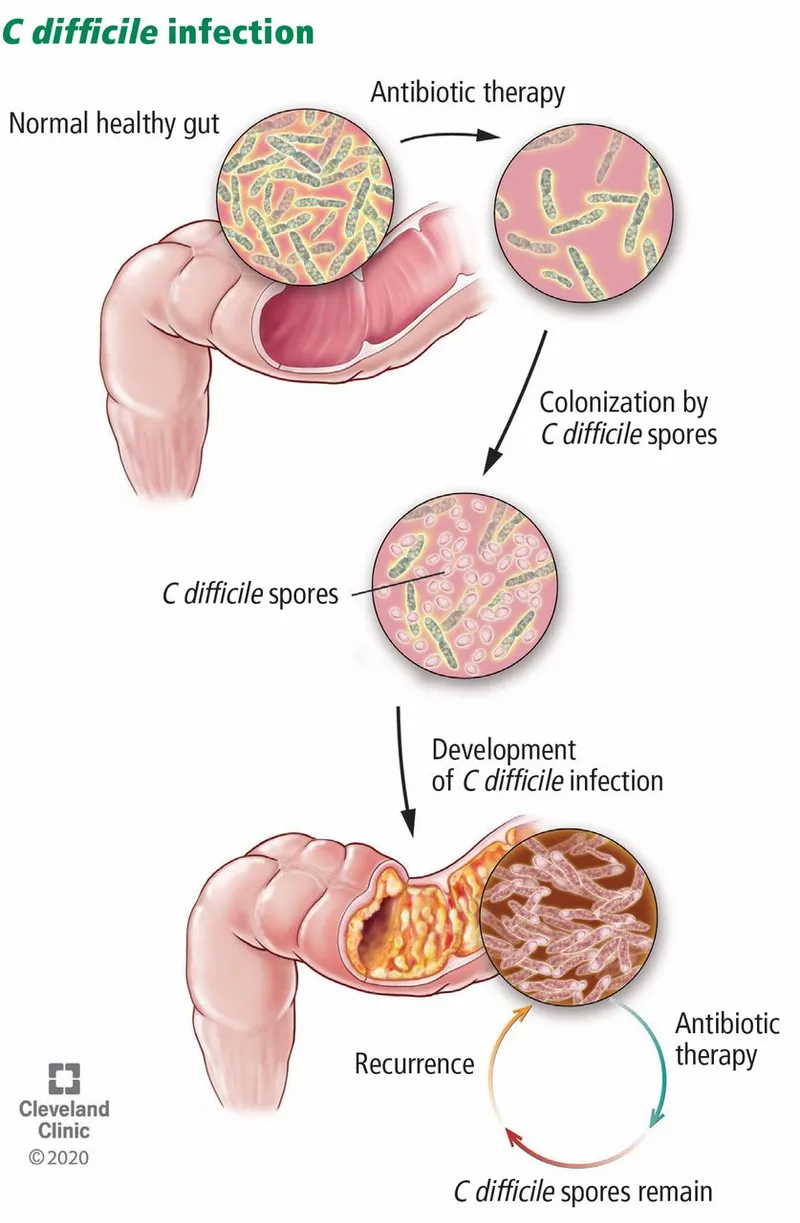
⭐ First-line for initial, non-severe CDI: Oral Vancomycin 125mg QID or Fidaxomicin 200mg BID for 10 days.
HAI Prevention - Germ Warfare Guide
- Standard Precautions: Universal: hand hygiene, PPE (gloves, gowns, masks), safe injections, cough etiquette.
- Hand Hygiene: 📌 WHO 5 Moments (see diagram). ABHR preferred; soap & water if soiled.
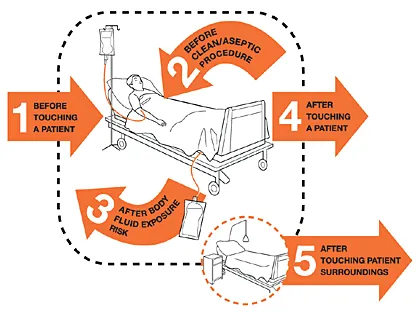
⭐ Hand hygiene is the single most important measure to prevent HAIs.
- Transmission-Based Precautions: For known/suspected pathogens.
- Key Strategies:
- Environmental Cleaning: Regular disinfection, high-touch surfaces.
- Antimicrobial Stewardship: Optimize use, dose, duration.
- HAI Surveillance: Monitor rates, detect outbreaks, feedback.
- BMW Management: Safe segregation, treatment, disposal of biomedical waste.
High‑Yield Points - ⚡ Biggest Takeaways
- CLABSI: Implement prevention bundles. Key pathogens: S. aureus, Gram-negatives.
- CAUTI: Most common HAI. E. coli frequent. Prompt catheter removal is vital.
- VAP: Prevent with head elevation, oral chlorhexidine. Pathogens: Pseudomonas, MRSA.
- SSI: Prophylactic antibiotics <60 mins pre-incision. S. aureus is a major cause.
- C. difficile: Causes antibiotic-associated diarrhea. Treat with oral vancomycin/fidaxomicin.
- Hand hygiene: Single most effective measure to prevent HAIs.
- MDROs (MRSA, CRE): Require contact precautions and active surveillance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

