Fungal Infections Overview - Fungus Among Us
- Types:
- Yeasts (e.g., Candida): Unicellular, reproduce by budding.
- Molds (e.g., Aspergillus): Multicellular, form hyphae.
- Dimorphic: Yeast form at 37°C (body/tissue), mold form at 25°C (environment). 📌 "Mold in cold, Yeast in heat."
- Key Structures:
- Cell Wall: Chitin, glucans.
- Cell Membrane: Ergosterol.
⭐ Ergosterol in the fungal cell membrane is a primary target for many antifungal drugs (e.g., Amphotericin B, Azoles).
Superficial & Cutaneous Mycoses - Itchy & Scratchy Crew
- Dermatophytes: Keratinophilic fungi. Genera: Trichophyton, Microsporum, Epidermophyton.
- Cause Tinea (ringworm): capitis (scalp), corporis (body), cruris (groin), pedis (foot), unguium (nail).
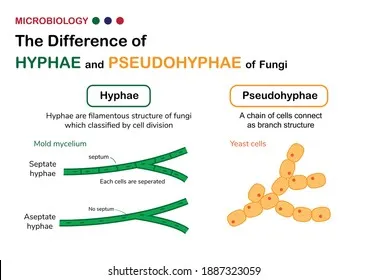
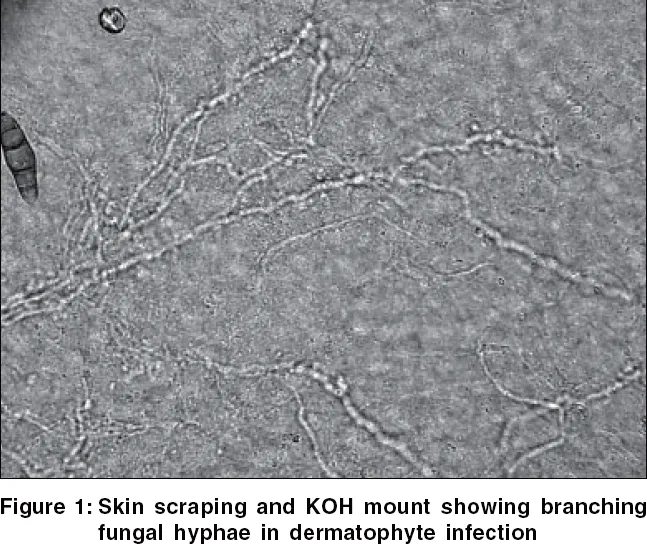
- Diagnosis: KOH mount (segmented hyphae).
- Malassezia furfur: Pityriasis (Tinea) versicolor.
- Hypo/hyperpigmented scaling macules; often on trunk.
- KOH: "Spaghetti & meatballs" (yeast & hyphae).
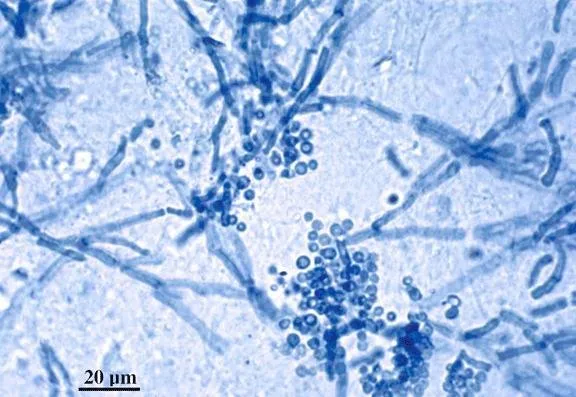
- Cutaneous Candidiasis: Candida albicans.
- Intertrigo, diaper dermatitis. Erythematous plaques, satellite pustules.
⭐ Malassezia furfur causes Tinea versicolor, is a lipophilic yeast (not a dermatophyte), and lesions typically fluoresce yellow-green under Wood's lamp.
Systemic Dimorphic Mycoses - Shape-Shifting Spores
| Fungus | Endemic Area | Morphology (Yeast Form) | Key Clinical Findings |
|---|---|---|---|
| Histoplasma | Ohio/Mississippi river valleys (bird/bat guano) | Small, oval; intracellular in macrophages | Pneumonia (often asymptomatic/mild), dissemination in IC |
| Blastomyces | Eastern/Central US (decaying organic matter) | Large, broad-based budding yeast | Pneumonia, skin (verrucous ulcers), bone lesions |
| Coccidioides | Southwestern US, N. Mexico (desert soil) | Spherules containing endospores | Valley fever (flu-like), erythema nodosum, meningitis |

⭐ Histoplasma capsulatum is typically found intracellularly within macrophages and can mimic TB.
Opportunistic Mycoses - Immune Busters
| Organism | Key Disease(s) | Dx Highlights | Image Placeholder Query |
|---|---|---|---|
| Candida | Thrush, esophagitis, disseminated dz. | Pseudohyphae, budding yeast; culture | "Candida albicans microscopy" |
| Aspergillus | ABPA, aspergilloma, invasive dz. | Septate hyphae, acute (45°) angle; Galactomannan. | "Aspergillus hyphae microscopy" |
| Cryptococcus neoformans | Meningitis (CD4 < 100); pneumonia. | India ink (capsule); Cryptococcal antigen (CrAg) test. | "Cryptococcus neoformans India ink stain" |
| Mucor / Rhizopus | Rhino-orbital-cerebral (DKA); pulmonary. | Broad, non-septate hyphae, right-angle (90°). | "Mucor hyphae microscopy" |
| Pneumocystis jirovecii (PJP) | Pneumonia (CD4 < 200). Prophylaxis. | Cysts on silver stain (GMS). | "Pneumocystis jirovecii cysts silver stain" |
Antifungal Agents - Foe Finishers
| Class | MOA | Spectrum | Key ADRs | Clinical Pearls |
|---|---|---|---|---|
| Polyenes | Binds ergosterol, ↑ cell permeability | Broad (Candida, Aspergillus, Crypto) | Nephrotoxicity, infusion reactions, ↓K⁺, ↓Mg²⁺ | Amphotericin B (AmB) |
| Azoles | Inhibit ergosterol synthesis (CYP450) | Broad (Candida, Crypto, Dermatophytes) | Hepatotoxicity, drug interactions (CYP inh.) | Fluconazole (Candida), Itraconazole (Aspergillus, dimorphic), Voriconazole (Aspergillus) |
| Echinocandins | Inhibit β-(1,3)-D-glucan synthesis | Candida, Aspergillus | GI upset, flushing | Caspofungin, Micafungin; good for azole-resistant Candida |
| Flucytosine | Inhibits DNA/RNA synthesis | Cryptococcus, Candida (combo therapy) | Bone marrow suppression, hepatotoxicity | 📌 "5-FC = Five-Fluorocytosine causes Fatty liver, Flatulence, Fall in Hb" |
High‑Yield Points - ⚡ Biggest Takeaways
- Mucormycosis: Uncontrolled diabetes, rhino-orbital-cerebral, non-septate hyphae, Amphotericin B.
- Aspergillosis: ABPA (asthma, ↑IgE), Aspergilloma, Invasive (immunocompromised, Voriconazole), septate hyphae.
- Candidiasis: Thrush, esophagitis; disseminated in immunocompromised. Fluconazole. C. auris (MDR).
- Cryptococcal meningitis: HIV/AIDS (CD4 <100), India ink, CrAg test, Amphotericin B + Flucytosine.
- PCP (P. jirovecii): HIV/AIDS (CD4 <200), bilateral infiltrates, TMP-SMX (treatment/prophylaxis).
- Histoplasmosis: Mimics TB, bird/bat droppings, disseminated in immunocompromised, Itraconazole.
- Sporotrichosis: "Rose gardener's disease", lymphocutaneous spread, Itraconazole.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

