Antimicrobial Resistance: Basics - Resistance Rising
- Antimicrobial Resistance (AMR): Microbes evolve to resist drugs, making infections harder to treat; ↑ risk of spread, severe illness, and death.
- Types of Resistance:
- Intrinsic Resistance: Natural, inherent insensitivity of a microorganism to an antimicrobial (e.g., Gram-negative bacteria to Vancomycin due to outer membrane impermeability).
- Acquired Resistance: Previously susceptible microbe develops resistance, typically via genetic mutation or Horizontal Gene Transfer (HGT - conjugation, transduction, transformation).
- Impact:
- Clinical: ↑ morbidity & mortality, treatment failures, prolonged illness, potential need for more toxic or expensive drugs.
- Economic: ↑ healthcare costs (longer hospital stays, ICU care), ↓ productivity due to illness.

⭐ The 'One Health' approach is crucial for combating AMR, recognizing the interconnectedness of human, animal, and environmental health.
Antimicrobial Resistance: Mechanisms - Bugs' Superpowers
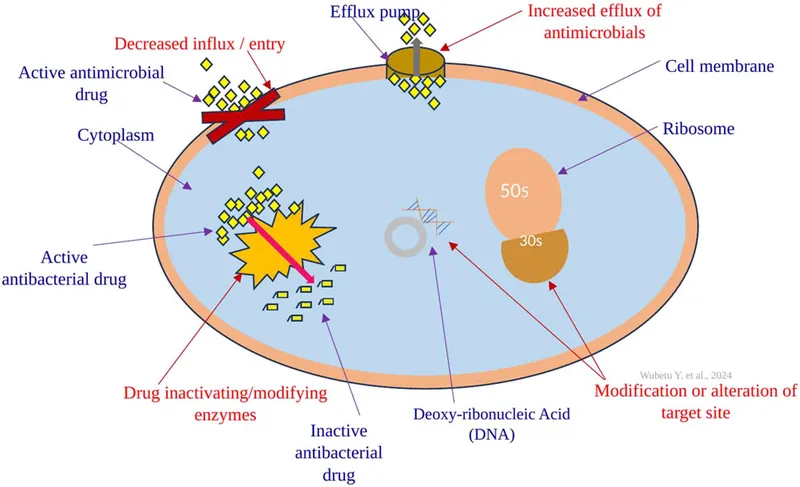
- Key Mechanisms:
- Enzymatic Inactivation: e.g., β-lactamases (ESBLs, KPCs, NDMs) destroy β-lactams.
- Target Site Modification: e.g., PBP2a in MRSA (methicillin resistance); VanA/VanB in VRE (vancomycin resistance).
- Efflux Pumps: Actively expel antibiotics (e.g., Tet efflux for tetracyclines).
- Decreased Permeability: Porin loss/mutation reduces antibiotic entry (e.g., carbapenems).
- Genetic Basis:
- Mutations: Spontaneous DNA alterations.
- Horizontal Gene Transfer (HGT): Gene acquisition. Key types (📌 Mnemonic: Transformers Can Talk):
- Transformation: Uptake of free DNA.
- Conjugation: Plasmid transfer via pili.
- Transduction: Phage-mediated transfer.
⭐ Plasmids are key vectors for the rapid spread of multi-drug resistance genes like NDM-1 via conjugation.
Antimicrobial Resistance: Key Pathogens - The Usual Suspects
📌 ESKAPE Pathogens: Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa, Enterobacter spp.
| Pathogen | Gene(s) | Resists | Tx Pearls (India) |
|---|---|---|---|
| MRSA (S. aureus) | mecA | Methicillin, most β-lactams | Vancomycin, Linezolid, Teicoplanin. |
| VRE (E. faecium) | vanA, vanB | Vancomycin | Linezolid, Daptomycin. |
| ESBL-E (E.coli, Klebsiella) | CTX-M, SHV, TEM | Cephalosporins, Penicillins | Carbapenems. Pip-Tazo (check MIC). |
| CRE (Enterobacteriaceae) | NDM, KPC, OXA-48 | Carbapenems, most β-lactams | Colistin, Tigecycline. Combo Rx. High alert. |
| MDR/XDR-TB | rpoB, katG, inhA | Rifampicin, Isoniazid, others | DST-guided. Bedaquiline, Linezolid. |
Antimicrobial Resistance: Control Strategies - Fighting Back Smart
- Antimicrobial Stewardship (AMS):
- Core: 📌 5 Ds (Diagnosis, Drug, Dose, Duration, De-escalation).
- Practices: Formulary restriction, pre-authorization, audit & feedback.
- WHO's AWARE (Access, Watch, Reserve) classification guides antibiotic choice.
- Infection Prevention & Control (IPC):
- Key: Hand hygiene, contact precautions, environmental cleaning, care bundles.
- Diagnostics & Surveillance:
- Crucial: Rapid diagnostics & antimicrobial susceptibility testing (AST).
- Monitoring: Surveillance networks (e.g., WHONET by WHO).
- Innovations & Policy:
- New drug development pipeline (challenges exist).
- Alternatives: Phage therapy, monoclonal antibodies, vaccines.
- India: National Action Plan on AMR.

⭐ The 'AWARE' classification (Access, Watch, Reserve) by WHO is a key AMS tool to guide appropriate antibiotic use and reduce AMR emergence.
High‑Yield Points - ⚡ Biggest Takeaways
- ESBLs (Extended-Spectrum Beta-Lactamases) confer resistance to penicillins & cephalosporins; carbapenems are key treatments.
- MRSA (Methicillin-Resistant S. aureus), due to the mecA gene (PBP2a alteration), is typically treated with Vancomycin.
- VRE (Vancomycin-Resistant Enterococci), via VanA/VanB genes, often requires Linezolid or daptomycin for effective treatment.
- Carbapenemases (e.g., NDM-1, KPC, OXA-48) cause broad resistance; consider ceftazidime-avibactam or newer agents.
- MDR-TB signifies resistance to at least isoniazid and rifampicin; XDR-TB involves further resistance to fluoroquinolones and injectables.
- Key AMR mechanisms: enzyme inactivation (e.g., beta-lactamases), target site modification, active efflux pumps, and decreased permeability.
- Antimicrobial stewardship programs are vital to combat the growing threat of AMR and preserve antibiotic efficacy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

