Inpatient Procedures - Tapping Treasures
I. Thoracentesis (Pleural Tap)
- Indications: Dx (new effusion), Tx (dyspnea).
- Site: Mid-scapular/axillary line, 1-2 ICS below fluid, above rib. US guidance.
- Complications: Pneumothorax, hemothorax, re-expansion pulmonary edema (drain <1.5L), vasovagal.
- Light's Criteria (Exudate if any 1):
- Pl.Pr/S.Pr >0.5 (Pleural Protein/Serum Protein)
- Pl.LDH/S.LDH >0.6 (Pleural LDH/Serum LDH)
- Pl.LDH >2/3 ULN serum (Pleural LDH > two-thirds Upper Limit of Normal for serum LDH). 📌 Mnemonic "PLE": Protein ratio, LDH ratio, Enz_LDH (absolute).
II. Paracentesis (Ascitic Tap)
- Indications: Dx (new ascites, SBP rule-out), Tx (tense ascites).
- Site: LLQ (2-3cm medial-superior to ASIS) or midline infraumbilical. Z-track.
- Complications: Leak, hematoma, bowel perf., infection.
- SAAG (Serum-Ascites Albumin Gradient):
- SAAG = S.Alb - Asc.Alb (Serum Albumin - Ascites Albumin)
- ≥1.1 g/dL: Portal HTN (cirrhosis, CHF).
- <1.1 g/dL: Non-portal HTN (malignancy, TB).
⭐ SAAG ≥1.1 g/dL ~97% accurate for portal HTN ascites.

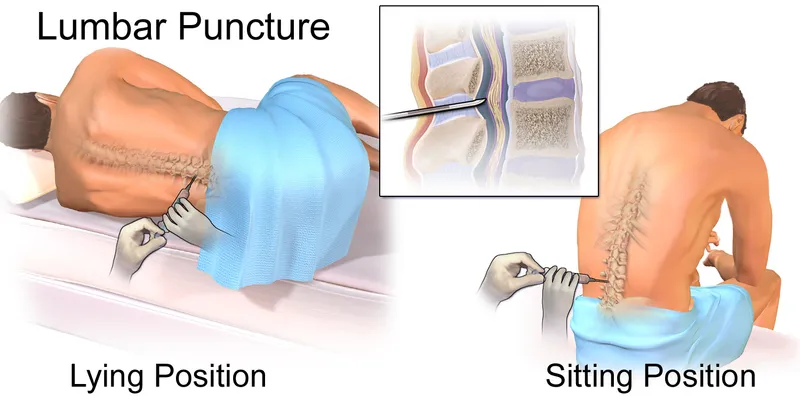
Inpatient Procedures - LP Lowdown
- Indications: Dx (meningitis, SAH, MS), Therapeutic (↑ICP, meds).
- Contraindications:
- ↑ICP signs (papilledema, focal deficits) → CT head first!
- Coagulopathy (INR > 1.5, Plt < 50k)
- Local skin infection.
- Spinal epidural abscess.
- Procedure Key Points:
- Position: Lateral decubitus, knees to chest.
- Landmark: L3-L4/L4-L5 (iliac crests).
- Opening Pressure (OP): Normal 10-20 cm H₂O.
- Collect 3-4 tubes (📌 Order: 1.Chem/Immuno, 2.Micro, 3.Cells, 4.Special).
- Complications: Post-LP headache, infection, bleeding, herniation.
⭐ Xanthochromia (yellow CSF) indicates SAH if >6-12 hrs post-bleed (bilirubin).
Inpatient Procedures - Vascular Ventures
-
Central Venous Catheter (CVC):
- Indications: CVP monitoring, TPN, vasopressors, poor peripheral access, rapid fluid resuscitation.
- Sites: Internal Jugular (IJV) (preferred), Subclavian (↑ pneumothorax risk), Femoral (↑ infection risk).
- Technique: Seldinger (needle → guidewire → dilator → catheter).
- Complications: Pneumothorax (esp. subclavian), arterial puncture, hematoma, infection (CLABSI), thrombosis, air embolism.
- 📌 Mnemonic (IJV anatomy): "Two Heads Are Better Than One" (Sternocleidomastoid heads for IJV triangle).
-
Arterial Blood Gas (ABG) Sampling:
- Indications: Assess oxygenation ($PaO_2$), ventilation ($PaCO_2$), acid-base status (pH, $HCO_3^-$).
- Sites: Radial (preferred), brachial, femoral.
- Pre-procedure: Modified Allen's Test (for radial artery patency).
- Complications: Hematoma, arterial spasm, thrombosis, nerve injury, infection.

⭐ Most common non-infectious complication of CVC is catheter malposition.
Inpatient Procedures - Tube Trails & Tips
-
Nasogastric (NG) Tube Essentials:
- Uses: Gastric decompression (SBO), lavage, medication/feed delivery.
- Sizing: Adults 12-18 Fr. Measurement: NEX (Nose-Earlobe-Xiphoid).
- Insertion: Upright, lubricate tube, chin-to-chest, swallow sips of water.
-
Placement Verification (CRUCIAL):
- Bedside checks: Aspirate appearance & pH (gastric target < 5.5). Epigastric "whoosh" on air insufflation.
⭐ Chest X-ray (CXR) is the gold standard for confirming NG tube tip location, vital before initiating feeds or high-risk medications.
-
Key Pearls & Pitfalls:
- 📌 Mnemonic: NEXt, X-ray Confirms Position (NEX, X-ray Confirmation).
- Risks: Malposition (tracheal, pulmonary, intracranial), sinusitis, epistaxis, aspiration pneumonia.
- ⚠️ If cough, excessive gagging, or respiratory distress during insertion, withdraw tube immediately.
High‑Yield Points - ⚡ Biggest Takeaways
- Thoracentesis: Use Light's criteria for exudates; site: 8th-9th ICS, mid-axillary line.
- Paracentesis: SAAG > 1.1 g/dL implies portal hypertension; site: LLQ.
- Lumbar Puncture: Avoid if raised ICP; normal opening pressure <20 cm H2O.
- Central Lines: Seldinger technique used; IJV preferred; risk: pneumothorax.
- ABG: Allen's test pre-radial puncture; radial artery common.
- NG Tube: X-ray confirms placement (gold standard).
- Urinary Catheter: Aseptic technique prevents CAUTI.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

