Blood Groups & Compatibility - Mix 'n' Match Mayhem
- ABO (Landsteiner's): Natural Abs to absent A/B Ags.
- O: Anti-A/B. A: Anti-B. B: Anti-A. AB: None.
- 📌 Univ. Donor: O Rh(D)-neg. Univ. Recipient: AB Rh(D)-pos.
- ABO Compatibility:
Recipient Donor O Donor A Donor B Donor AB O ✅ ❌ ❌ ❌ A ✅ ✅ ❌ ❌ B ✅ ❌ ✅ ❌ AB ✅ ✅ ✅ ✅
- Rh System: D Ag key. Rh(D)-neg gets Rh(D)-neg blood.
- Weak D: Donor D+; Recipient D- (if sensitized).
- Rh Prophylaxis: Anti-D Ig (300 µg) for Rh(D)-neg mother/Rh(D)+ fetus.
- Bombay (Oh): No H Ag. Anti-A, -B, -H. Needs Oh blood.
- Testing: Typing (ABO/Rh), Screen (Abs), Crossmatch.
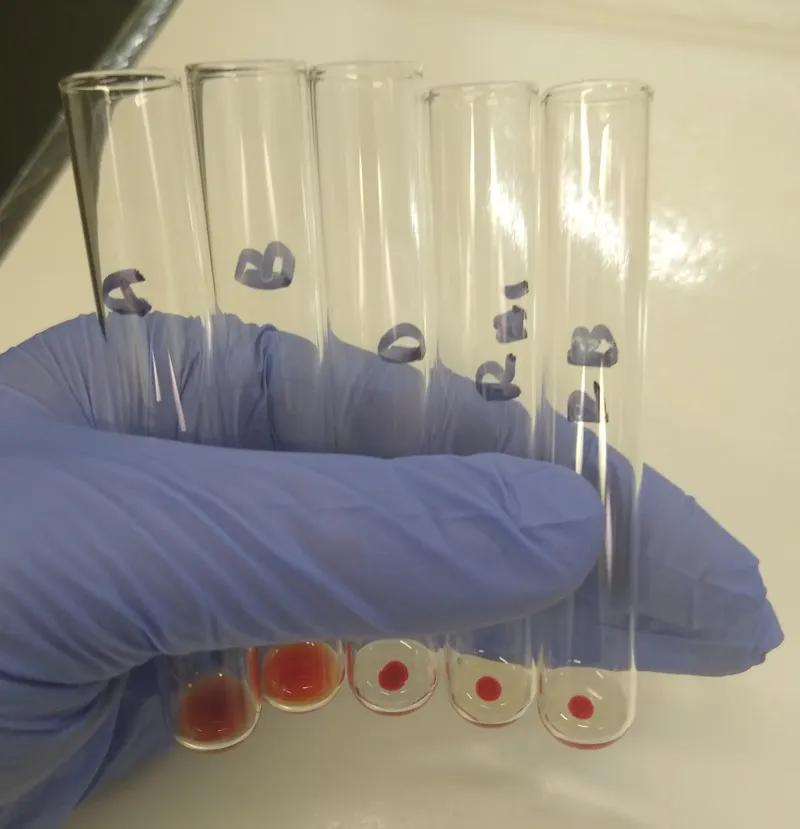
⭐ Bombay (Oh) lacks H Ag; only Oh blood compatible due to anti-H.
Blood Components - The Life-Saving Lineup
| Component | Key Contents | Storage (Temp, Life) | Vol. | Dose / Increment | Key Indications |
|---|---|---|---|---|---|
| PRBCs | RBCs, minimal plasma | 2-6°C, 35-42d | ~300mL | 1U ↑Hb 1g/dL or Hct 3% | Anemia (Hb<7g/dL), acute loss >20% |
| Platelets | Platelets, plasma | 20-24°C (agitate), 5d | 50-200mL | RDP: ↑5-10k/µL; SDP: ↑30-50k/µL | Thrombocytopenia (<10k/µL), active bleeding |
| FFP | All clotting factors, albumin | ≤-18°C, 1yr (Thawed: 24h, 1-6°C) | ~225mL | 10-15mL/kg; ↑factors 20-30% | Coagulopathy (INR>1.7), TTP, MTP |
| Cryo | Fibrinogen, F.VIII, vWF, F.XIII 📌 | ≤-18°C, 1yr (Thawed: 4-6h, 20-24°C) | ~15mL/U | 1U/10kg ↑Fibrinogen ~50mg/dL | Hypofibrinogenemia (<100mg/dL), vWD, F.XIII def. |
| Granulocytes | Neutrophils, some RBCs/PLTs | 20-24°C, 24h (no agitate) | ~250mL | Variable; clinical response | Severe neutropenia (<500/µL) + sepsis (unresponsive, rare) |
Transfusion Reactions - When Good Blood Goes Bad
STOP TRANSFUSION! Maintain IV. Notify blood bank.
Acute Reactions (<24h)
| Reaction | Onset | Features/Patho | Mgmt |
|---|---|---|---|
| AHTR | Mins-Hrs | ABO mismatch; Hemolysis, fever, shock | Supportive |
| FNHTR | <4h | Cytokines/WBC Abs; Temp ↑ ≥1°C | Antipyretics |
| Allergic/Anaphylactic | Mins-Hrs | IgE (urticaria); Anti-IgA (anaphylaxis) | Antihistamines/Epi |
| TRALI | <6h | Donor Abs; Non-cardiac pulm. edema, hypoxemia | O2, supportive |
| TACO | <6h | Volume overload; Cardiac pulm. edema, ↑BNP | Diuretics, O2 |
| Bacterial Contam. | Mins-Hrs | Toxins; High fever, shock | IV Abx |
Delayed Reactions (>24h)
- DHTR (3-30d): Extravascular hemolysis (IgG); ↓Hb, jaundice. Supportive.
- PTP (5-12d): Anti-platelet Abs (HPA-1a); Severe thrombocytopenia. IVIG.
- TA-GVHD (1-6w): Donor T-cells attack host; Rash, pancytopenia. Irradiate to prevent.
Special Transfusions & Safety - Handle With Care
- Massive Transfusion Protocol (MTP):
- Definition: Replacement of >1 blood volume in 24 hrs, >50% in 4 hrs, or >4 units in 1 hr.
- Ratio: 1:1:1 (PRBC:FFP:Platelets).
- Complications (📌 ACHE): Acidosis, Coagulopathy, Hypothermia, Electrolyte imbalance ($↑K^+$, $↓Ca^{2+}$).
- Transfusion Transmitted Infections (TTIs):
- Mandatory Indian screening: HIV, HBV, HCV, Syphilis, Malaria.
- Window period risk remains.
⭐ HBV is the most common TTI in India despite screening.
- Leucoreduction: Reduces febrile non-hemolytic reactions, CMV transmission. Indicated in immunocompromised, chronically transfused patients.
- Irradiation: Prevents Transfusion-Associated Graft-Versus-Host Disease (TA-GVHD). Indicated for immunocompromised, directed donations from relatives, and intrauterine/neonatal transfusions.
High‑Yield Points - ⚡ Biggest Takeaways
- O RhD negative is the universal RBC donor; AB RhD positive is the universal RBC recipient.
- AB group is the universal plasma donor; O group is the universal plasma recipient.
- FNHTR (Febrile Non-Hemolytic Transfusion Reaction) is the most common reaction, caused by cytokines from donor leukocytes.
- TACO (Transfusion-Associated Circulatory Overload) presents with fluid overload; manage with diuretics and slow infusion.
- TRALI (Transfusion-Related Acute Lung Injury) causes non-cardiogenic pulmonary edema due to donor antibodies.
- Massive transfusion protocol often uses a 1:1:1 ratio of PRBCs:FFP:Platelets.
- Irradiation of blood products prevents TA-GVHD in immunocompromised patients and directed donations from relatives.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

