MPN Overview - Clonal Chaos Kickoff
- Clonal hematopoietic stem cell (HSC) disorders: Characterized by excessive production of mature myeloid cells.
- Common features: Splenomegaly (due to extramedullary hematopoiesis), marrow hypercellularity, constitutional symptoms, risk of thrombosis/hemorrhage.
- Potential for transformation to myelofibrosis (spent phase) or Acute Myeloid Leukemia (AML).
- WHO classification integrates clinical, morphological, cytogenetic, and molecular (driver mutations) findings.
- Key driver mutations:
- JAK2 (V617F most prevalent)
- CALR (calreticulin)
- MPL (thrombopoietin receptor)
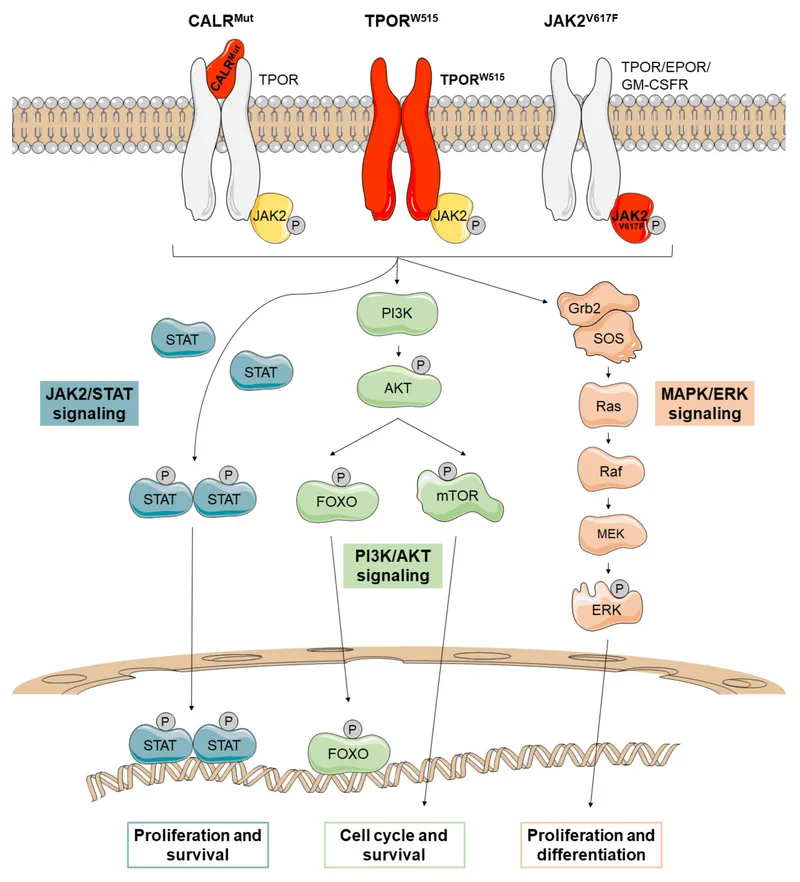
⭐ JAK2 V617F is the most common mutation across Polycythemia Vera (PV), Essential Thrombocythemia (ET), and Primary Myelofibrosis (PMF).
Polycythemia Vera (PV) - Too Much Red
- Clonal, erythroid-dominant MPN: ↑RBC mass. JAK2 V617F (>95%) or exon 12 mutation.
- Sx: Hyperviscosity (headache), plethora, ruddy cyanosis, splenomegaly, thrombosis.
- Dx (WHO): ↑Hb/Hct (Hb >16.5 g/dL (M) / >16 g/dL (W), Hct >49% (M) / >48% (W)), BM panmyelosis, JAK2 mutation. ↓EPO (minor).
- Rx: Phlebotomy (target Hct <45%), low-dose Aspirin (75-100 mg/day). Cytoreduction (e.g., Hydroxyurea) if high-risk.

⭐ Aquagenic pruritus (itching after warm water contact) is a classic and highly specific symptom of PV.
Essential Thrombocythemia (ET) - Platelet Party Peril
- Clonal MPN: ↑ megakaryopoiesis & sustained thrombocytosis (Platelets > 450 x 10^9/L).
- Mutations: JAK2 V617F (~50-60%), CALR (~20-30%), MPL (~5-10%).
- Clinical: Often asymptomatic. Vasomotor (headache, erythromelalgia), thrombosis, hemorrhage. Mild splenomegaly.
- Diagnosis: Exclude reactive thrombocytosis; BM biopsy shows ↑ large, hyperlobulated megakaryocytes.
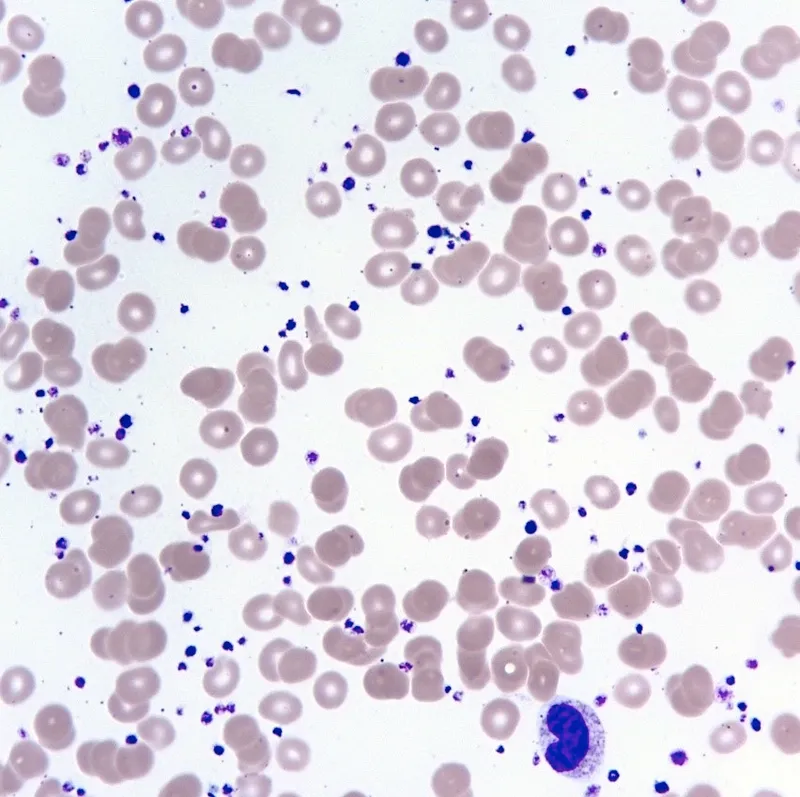
⭐ CALR mutations are typically found in JAK2 V617F-negative ET and are associated with a lower thrombotic risk compared to JAK2-mutated ET and a more indolent course. Higher platelet counts may be seen.
- Treatment Goal: Prevent thrombosis & hemorrhage. Manage symptoms. Low risk: Aspirin. High risk: Aspirin + cytoreduction (Hydroxyurea).
Primary Myelofibrosis (PMF) - Marrow's Fibrous Fate
- Clonal stem cell disorder: progressive bone marrow (BM) fibrosis, extramedullary hematopoiesis (EMH).
- Mutations: JAK2 V617F (~50-60%), CALR (~25-35%), MPL (~5-10%).
- Clinical: Massive splenomegaly (EMH), anemia, constitutional symptoms (fever, sweats, weight loss).
- Peripheral Smear (PS): Leukoerythroblastosis, dacrocytes (teardrop cells).

- BM Biopsy: Hypercellular early → fibrotic; "dry tap" common.
- Prognosis: DIPSS (Age >65, Hb <10 g/dL, WBC >25x10⁹/L, Blasts ≥1%, symptoms).
- Rx: Ruxolitinib (JAK inhibitor); Allogeneic HSCT (curative).
⭐ Extramedullary hematopoiesis leading to massive splenomegaly is a hallmark of PMF.
Chronic Myeloid Leukemia (CML) - Philly's Famous Fusion
- Patho: Philadelphia (Ph) chromosome t(9;22) → BCR-ABL1 fusion gene → constitutive tyrosine kinase activity. 📌 Philly CML.
- Phases (Bone Marrow Blasts): Chronic <10%, Accelerated 10-19%, Blast Crisis ≥20%.
- Features: Splenomegaly, fatigue, weight loss; marked leukocytosis (myeloid left shift, basophilia), thrombocytosis common.
- Tx & Monitoring: Tyrosine Kinase Inhibitors (TKIs) e.g., Imatinib. Aim for Major Molecular Response (MMR). Allogeneic SCT for resistant/advanced.
⭐ Low/absent Leukocyte Alkaline Phosphatase (LAP) score is characteristic, distinguishing CML from leukemoid reaction (high LAP).

High‑Yield Points - ⚡ Biggest Takeaways
- JAK2 V617F mutation is key in Polycythemia Vera (PV), Essential Thrombocythemia (ET), and Primary Myelofibrosis (PMF). CALR/MPL mutations are common in JAK2-negative cases.
- PV presents with ↑RBC mass, ↓EPO levels, aquagenic pruritus, and splenomegaly.
- ET is characterized by marked thrombocytosis; major risks include thrombosis or hemorrhage.
- PMF features progressive bone marrow fibrosis, massive splenomegaly, and leukoerythroblastic picture with teardrop poikilocytes.
- Chronic Myeloid Leukemia (CML) is defined by the BCR-ABL1 fusion gene (Philadelphia chromosome t(9;22)) and responds to Tyrosine Kinase Inhibitors (TKIs).
- All MPNs carry a risk of transformation to Acute Myeloid Leukemia (AML) or a myelofibrotic spent phase (except CML which has blast crisis).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

