Lymphoma Basics - Genesis & Types
- Lymphomas: Malignant clonal proliferation of lymphocytes or their precursors.
- Typically arise in lymph nodes; can involve extranodal sites.
- Broadly classified into two main types:
- Hodgkin Lymphoma (HL)
- Non-Hodgkin Lymphoma (NHL)
- Key distinction:
- HL: Characterized by pathognomonic Reed-Sternberg (RS) cells.
- NHL: More common, diverse group; lacks RS cells.
⭐ Lymphomas are broadly classified into Hodgkin Lymphoma (HL), characterized by Reed-Sternberg cells, and Non-Hodgkin Lymphoma (NHL), a more diverse group.
Hodgkin Lymphoma - Classic Reed's Story
-
Pathognomonic Cell: Reed-Sternberg (RS) cell - large, binucleated or multinucleated, prominent eosinophilic nucleoli ('owl-eye' appearance).

-
B Symptoms: 📌 Fever (>38°C), drenching night sweats, unexplained weight loss (>10% in 6 months).
-
HL Subtypes:
Subtype Features Prognosis Nodular Sclerosis Most common, young adults, mediastinal mass Good Mixed Cellularity EBV association (~70%), older adults Fair Lymphocyte-Rich Best prognosis, few RS cells Excellent Lymphocyte-Depleted Rarest, HIV/immunocompromised, many RS cells Poor
⭐ Nodular Sclerosis is the most common subtype of Hodgkin Lymphoma in young adults, often presenting with a mediastinal mass and associated with good prognosis.
- Simplified Ann Arbor Staging:
Non-Hodgkin Lymphoma - Diverse & Diffuse
- Heterogeneous group of lymphoid malignancies; more common than Hodgkin. Often disseminated at diagnosis. Classified by cell type (B, T, NK) & aggressiveness.
- 📌 NHL Translocations: Follicular $t(14;18)$ (BCL2), Mantle $t(11;14)$ (Cyclin D1), Burkitt $t(8;14)$ (c-MYC).
Common NHL Subtypes:
| NHL Type | Origin | Key Feature(s) / Translocation | Markers |
|---|---|---|---|
| DLBCL | B-cell | Most common, aggressive | CD20+ |
| Follicular | B-cell | Indolent, BCL2 ($t(14;18)$) | CD20+, CD10+ |
| Mantle Cell | B-cell | Aggressive, Cyclin D1 ($t(11;14)$) | CD20+, CD5+ |
| Burkitt | B-cell | Highly aggressive, c-MYC ($t(8;14)$), 'starry sky' | CD20+, CD10+ |
| Marginal Zone (MALT) | B-cell | Indolent, chronic inflammation (e.g., H. pylori) | CD20+ |
| Mycosis Fungoides | T-cell | Cutaneous, Pautrier's microabscesses | CD3+, CD4+ |
| ALCL | T-cell | ALK+ ($t(2;5)$ good prognosis), "hallmark" cells | CD30+, ALK+/- |
⭐ Burkitt Lymphoma, an aggressive B-cell NHL, is associated with $t(8;14)$ translocation involving the c-MYC oncogene and classically shows a 'starry sky' appearance on histology due to tingible body macrophages.
Lymphoma Management - Dx & Rx Blueprint
- Diagnosis (Dx):
- Gold Standard: Excisional LN biopsy.
- Key Tests: IHC, Flow cytometry.
- Staging: Ann Arbor; PET-CT (staging, response). BMB.
- Labs: CBC, LDH, Uric acid.
- Prognostic Scores:
Score Key Factors IPI (NHL) Age >60, ↑LDH, PS ≥2, Stage III/IV, >1 extranodal site IPS (HL) Alb <4, Hb <10.5, M, Age ≥45, Stg IV, WBC ≥15k, Lymph <0.6k/<8% - Treatment (Rx) Overview:
- HL: ABVD, BEACOPP; ISRT.
- NHL: Aggressive (DLBCL) → R-CHOP. Indolent (FL) → Watch & Wait / R-chemo.
- Relapsed/Refractory: Salvage, ASCT, CAR-T.
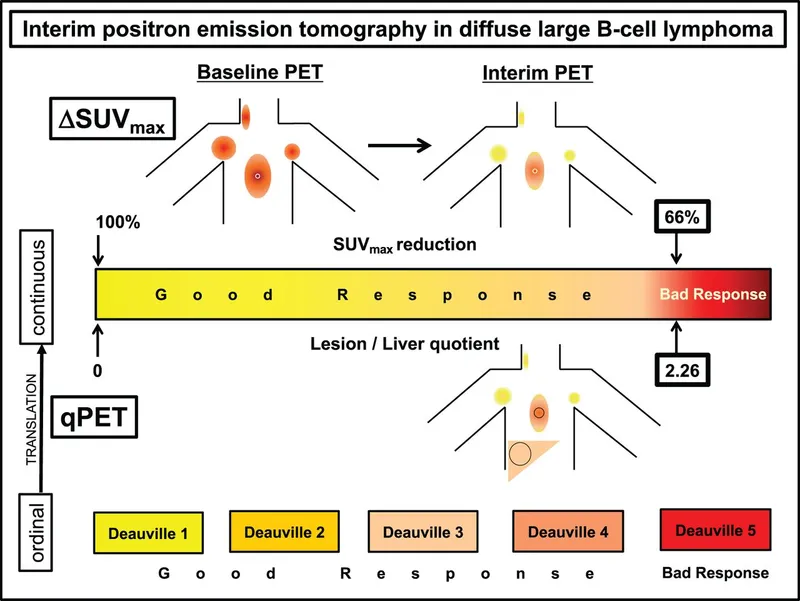
⭐ PET-CT scan is essential for initial staging, assessing treatment response (e.g., using Deauville criteria), and detecting relapse in most lymphomas.
High‑Yield Points - ⚡ Biggest Takeaways
- Hodgkin Lymphoma (HL) is characterized by pathognomonic Reed-Sternberg cells.
- Ann Arbor staging is crucial for both HL and Non-Hodgkin Lymphoma (NHL).
- NHL is more common than HL; Diffuse Large B-cell Lymphoma (DLBCL) is the most common aggressive NHL.
- Burkitt Lymphoma: features t(8;14) (c-myc oncogene), "starry sky" appearance.
- Follicular Lymphoma: features t(14;18) translocation (BCL-2 overexpression).
- Mantle Cell Lymphoma: features t(11;14) translocation (Cyclin D1 overexpression).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

