Leukemias: Overview - Blood Cell Mayhem
- Malignant clonal proliferation of hematopoietic cells, primarily originating in bone marrow (BM) & peripheral blood.
- Leads to BM failure (anemia, thrombocytopenia, neutropenia) & potential organ infiltration.
- Key Classifications:
- Acute vs. Chronic: Based on disease progression & cell maturity.
- Myeloid vs. Lymphoid: Based on cell lineage involved (e.g., AML, CML, ALL, CLL).

⭐ Auer rods (eosinophilic, needle-like granules in cytoplasm) are pathognomonic for Acute Myeloid Leukemia (AML), especially M3 (APML).
Acute Leukemias: ALL/AML - Sudden Strike Squad
- Rapid proliferation of blasts (>20% in bone marrow). Sudden onset.
- ALL (Acute Lymphoblastic Leukemia):
- Peak incidence: children (2-5 yrs). 📌 ALL kids get TdT+ toys.
- Lymphoblasts: TdT+, PAS+. Often CALLA (CD10)+.
- CNS involvement common; prophylaxis needed.
- AML (Acute Myeloid Leukemia):
- Primarily adults (median age ~65 yrs).
- Myeloblasts: MPO+, Sudan Black B+.
- Auer rods (eosinophilic needles in cytoplasm) are pathognomonic.
- DIC common in APL (M3 subtype, t(15;17)).
- Symptoms: Pancytopenia (fatigue, fever/infection, bleeding). Bone pain. Gingival hyperplasia (AML M4/M5).
⭐ Auer rods are pathognomonic for AML, representing fused lysosomal granules. Their presence excludes ALL.
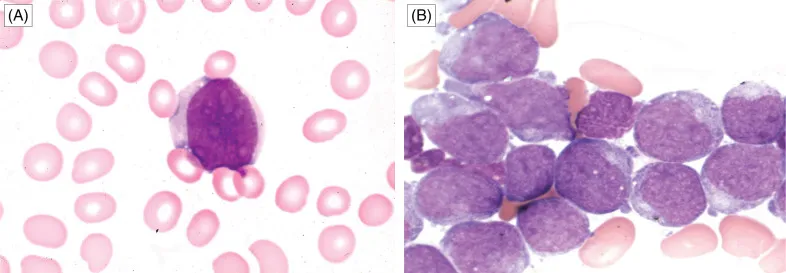
CML: Pathophysiology & Phases - The Philly Story
- Pathophysiology
- Genetic hallmark: Philadelphia chromosome (Ph+), from t(9;22)(q34;q11.2).
- Forms BCR-ABL1 fusion gene → constitutively active tyrosine kinase.
- Drives uncontrolled proliferation of myeloid cells, mainly granulocytes.
- Phases (WHO criteria)
- Chronic Phase (CP): <10% blasts (blood/BM). Often asymptomatic. Best TKI response.
- Accelerated Phase (AP): 10-19% blasts, OR ↑basophils ≥20%, OR persistent thrombocytopenia/thrombocytosis, OR new clonal chromosomal abnormalities (CCA).
- Blast Crisis (BC): ≥20% blasts (myeloid/lymphoid). Resembles acute leukemia.
⭐ BCR-ABL1 tyrosine kinase is the target for TKIs (e.g., Imatinib), revolutionizing CML treatment.
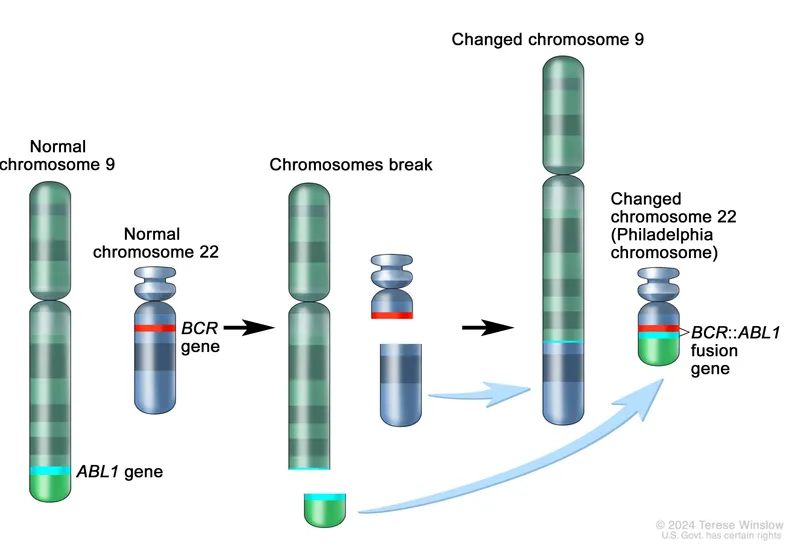 and BCR-ABL1 fusion protein diagram)
and BCR-ABL1 fusion protein diagram)
CLL: Features & Staging - The Smudge Saga
- Most common leukemia in elderly Western adults; clonal mature B-cell (CD5+) proliferation.
- Presentation: Often asymptomatic. Lymphadenopathy, hepatosplenomegaly. B-symptoms less common.
- Diagnosis: Sustained absolute lymphocytosis >5000/μL. Smudge cells (Gumprecht shadows).
- Immunophenotype: CD5+, CD19+, CD20+(dim), CD23+.
- Staging:
- Rai (0-IV): Lymphocytosis, lymphadenopathy, organomegaly, anemia (Hb <11 g/dL), thrombocytopenia (<100,000/μL).
- Binet (A,B,C): Based on # lymphoid areas, anemia, thrombocytopenia.
⭐ Richter's transformation: CLL transforms into aggressive large B-cell lymphoma (DLBCL) in ~5% cases, carrying a poor prognosis.
Leukemia: Complications & Dx - Red Alert & Clues
- Critical Complications (Red Alerts):
- Tumor Lysis Syndrome (TLS):
- Lab: ↑K, ↑$PO_4$, ↑Uric Acid, ↓Ca.
- Rx: Hydration, Allopurinol/Rasburicase.
- Neutropenic Fever:
- Criteria: ANC < 500/mm³ + Fever > 38.3°C.
- Rx: Empiric broad-spectrum antibiotics.
- Hyperleukocytosis/Leukostasis:
- WBC > 100,000/mm³ → sludging.
- Sx: CNS, respiratory distress.
- Rx: Hydration, Hydroxyurea, Leukapheresis.
- Tumor Lysis Syndrome (TLS):
- Key Diagnostic Clues:
- Peripheral Smear: Blasts ± Auer rods (AML).
- Bone Marrow Exam: Definitive Dx; cytogenetics, immunophenotyping (flow cytometry).
- Cytogenetics/FISH: Specific translocations (e.g., t(9;22) CML; t(15;17) APML).
⭐ Auer rods, eosinophilic needle-like granules in myeloblast cytoplasm, are pathognomonic for Acute Myeloid Leukemia (AML).
High‑Yield Points - ⚡ Biggest Takeaways
- Auer rods: Pathognomonic for AML, especially M3 (APL).
- APL (M3): t(15;17) translocation, treat with ATRA; risk of DIC.
- CML: Philadelphia chromosome t(9;22) (BCR-ABL1); responds to Imatinib.
- CLL: Most common adult leukemia (West); smudge cells on smear.
- ALL: Most common childhood cancer; CNS prophylaxis is mandatory.
- Richter's transformation: CLL converts to aggressive lymphoma (e.g., DLBCL).
- LAP score: High in Leukemoid reaction, low/absent in CML.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

