Cancer Genetics - Gene Game Gone Wrong
- Oncogenes: Proto-oncogenes with gain-of-function mutations (e.g., RAS, MYC, EGFR). Drive cell proliferation.
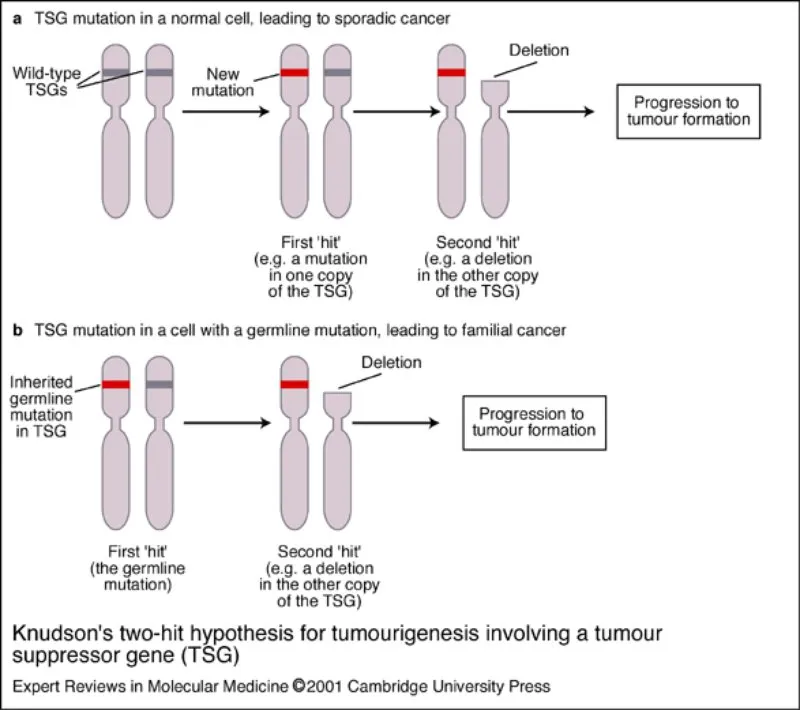
- Tumor Suppressor Genes (TSGs): Loss-of-function mutations (e.g., TP53, RB1, APC). Knudson's two-hit hypothesis.
- DNA Repair Genes: Mutations lead to genomic instability (e.g., BRCA1/2, MSH/MLH in Lynch syndrome).
- Epigenetic Changes: Alter gene expression without DNA sequence change (e.g., methylation, acetylation).
- Hereditary Cancer Syndromes: Often autosomal dominant inheritance (e.g., Li-Fraumeni, Lynch, FAP).
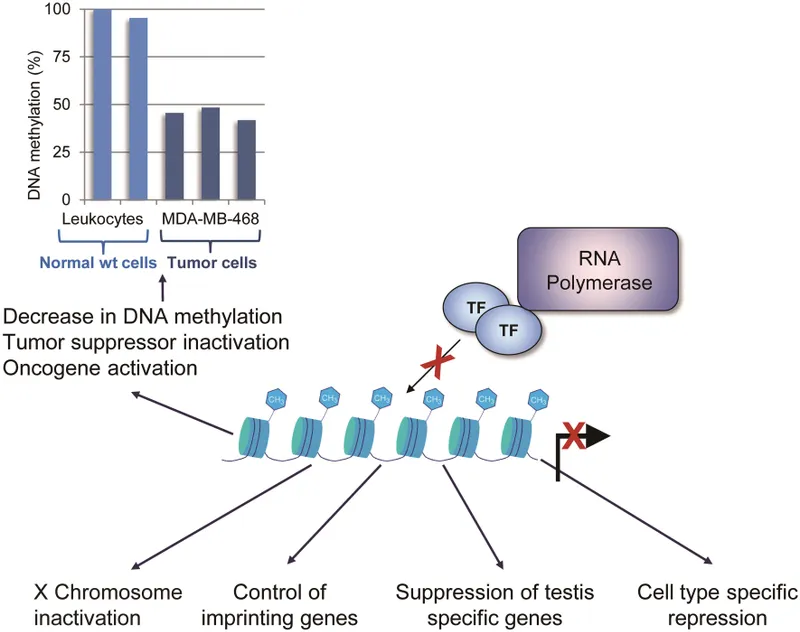
⭐ TP53 (guardian of the genome) is the most frequently mutated gene across all human cancers, involved in >50% of cases.
Hereditary Syndromes - Cancer Families
| Syndrome | Gene(s) | Cancers | Inheritance |
|---|---|---|---|
| Lynch | MSH2, MLH1+ | CRC, Endometrial, Ovarian, Stomach | AD |
| FAP | APC | CRC (100%), Duodenal, Thyroid | AD |
| Li-Fraumeni | TP53 | Sarcoma, Breast, Brain, Leukemia, Adrenal | AD |
| HBOC | BRCA1/2 | Breast, Ovarian, Prostate, Pancreatic | AD |
| VHL | VHL | Hemangioblastoma, RCC (clear), Pheo | AD |
| MEN1 | MEN1 | Parathyroid, Pancreatic NET, Pituitary (3P's) | AD |
| MEN2 | RET | MTC, Pheo; Parathyroid (2A)/Neuromas (2B) | AD |
| Retinoblastoma | RB1 | Retinoblastoma, Osteosarcoma | AD |
⭐ Knudson's "two-hit" hypothesis is key for RB1 (Retinoblastoma) & other tumor suppressor genes.
Oncogenes & TSGs - Accelerators & Brakes
Oncogenes act as "accelerators" for cell growth, requiring one activating mutation. Tumor Suppressor Genes (TSGs) act as "brakes", typically needing two inactivating mutations (hits) to lose function.
| Feature | Oncogenes (OG) | Tumor Suppressor Genes (TSG) |
|---|---|---|
| Analogy | 🚗 Accelerator | 🛑 Brake |
| Function | Promote cell growth/division | Inhibit cell growth/division, repair DNA |
| Mutation | Gain-of-function (GoF) | Loss-of-function (LoF) |
| Alleles | 1 hit (dominant) | 2 hits (recessive, Knudson's) |
| Examples | RAS, MYC, HER2, ABL, BRAF | TP53, RB1, BRCA1/2, APC, PTEN |
⭐ "Guardian of the Genome": TP53 is a critical TSG; its mutation is found in >50% of human cancers.
Simplified p53 Activation & Role (TSG Example):
DNA Repair - Cellular Fix-it Fails
Defective DNA repair leads to genomic instability, a hallmark of cancer. Key pathways:
| Pathway | Key Gene(s) | Associated Disorder(s) |
|---|---|---|
| Mismatch Repair (MMR) | MSH2, MLH1, PMS2 | Lynch Syndrome (HNPCC) |
| Nucleotide Excision Repair (NER) | XPA-XPG | Xeroderma Pigmentosum (XP) |
| Base Excision Repair (BER) | MUTYH | MUTYH-associated polyposis |
| Homologous Recombination (HR) | BRCA1, BRCA2, ATM, PALB2 | Hereditary Breast/Ovarian Cancer, Ataxia-Telangiectasia (AT) |
| Non-Homologous End Joining (NHEJ) | XRCC4, LIG4 | LIG4 syndrome |
⭐ Xeroderma Pigmentosum (XP) results from NER defects, leading to extreme UV sensitivity and skin cancer development at a young age.
Clinical Cancer Genetics - Precision Strikes
- Genetic Testing: Identifies germline (inherited, e.g., BRCA) & somatic (tumor-specific, e.g., EGFR) mutations.
- Precision Oncology: Guides targeted therapies (e.g., imatinib, olaparib) & immunotherapy selection.
- Prognosis & Risk: Assesses tumor behavior, recurrence risk, and hereditary cancer predisposition for family screening.
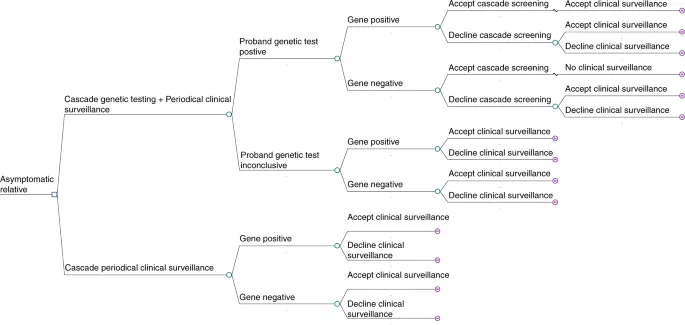
⭐ Liquid biopsies analyzing circulating tumor DNA (ctDNA) offer minimally invasive tumor genotyping and monitoring of treatment response.
High‑Yield Points - ⚡ Biggest Takeaways
- Knudson's two-hit hypothesis applies to tumor suppressor genes (e.g., RB1, TP53).
- Proto-oncogenes (e.g., RAS, MYC) require one activating mutation.
- Germline TP53 mutations cause Li-Fraumeni syndrome, predisposing to multiple cancers.
- BRCA1/BRCA2 mutations confer high risk for hereditary breast and ovarian cancer.
- Lynch syndrome (HNPCC) involves DNA mismatch repair gene defects (e.g., MSH2, MLH1).
- Philadelphia chromosome t(9;22) (BCR-ABL) is key in CML.
- Loss of heterozygosity (LOH) often inactivates the second allele of tumor suppressor genes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

