Diagnostic Foundations - Test Truths
- Purpose: To reduce diagnostic uncertainty, aiding clinical decisions and patient management.
- Types of Tests:
- Screening: Detects potential disease/risk in asymptomatic individuals (e.g., Pap smear).
- Diagnostic: Confirms/excludes disease in symptomatic individuals (e.g., ECG for chest pain).
- Monitoring: Tracks disease progression or treatment response (e.g., INR for warfarin).
- Role of Prevalence (Pre-test Probability):
- Significantly influences a test's predictive values (PPV, NPV).
- ↑ Prevalence generally → ↑ Positive Predictive Value (PPV).
- ↓ Prevalence generally → ↑ Negative Predictive Value (NPV).
⭐ No diagnostic test is 100% accurate; all tests have limitations and potential for error.
Test Performance Metrics - Number Crunch
Evaluate diagnostic tests using metrics derived from a 2x2 contingency table:
| Disease + | Disease - | Total | |
|---|---|---|---|
| Test + | True Pos (TP) | False Pos (FP) | TP + FP |
| Test - | False Neg (FN) | True Neg (TN) | FN + TN |
| Total | TP + FN | FP + TN | TP+FP+FN+TN |
- Sensitivity (Sn): Proportion of actual positives correctly identified. $Sn = TP / (TP + FN)$
- Specificity (Sp): Proportion of actual negatives correctly identified. $Sp = TN / (TN + FP)$
- Positive Predictive Value (PPV): Likelihood that a positive test means disease is present. $PPV = TP / (TP + FP)$
- Negative Predictive Value (NPV): Likelihood that a negative test means disease is absent. $NPV = TN / (TN + FN)$
- Likelihood Ratios (LR): Quantify how much a test result changes the likelihood of disease.
- LR+ (Positive): $Sensitivity / (1 - Specificity)$. How much a positive test increases disease odds.
- LR- (Negative): $(1 - Sensitivity) / Specificity$. How much a negative test decreases disease odds.
📌 SNOUT: Highly Sensitive test, when Negative, rules OUT disease. 📌 SPIN: Highly Specific test, when Positive, rules IN disease.
⭐ Sensitivity and Specificity are intrinsic test characteristics, unaffected by disease prevalence. PPV and NPV, however, are prevalence-dependent.
Strategic Test Selection - Smart Choices
Effective diagnosis hinges on smart test choices, guided by pre-test probability (PTP) and test characteristics.
-
Bayes' Theorem in Practice:
- Estimate PTP (clinical findings).
- Use Likelihood Ratios (LRs) for Post-test Probability (PoTP).
- Formula: $Post-test\ odds = Pre-test\ odds \times LR$.
- Pre-test odds = $PTP / (1 - PTP)$.
- PoTP = $Post-test\ odds / (1 + Post-test\ odds)$.
- LRs >10 (rule-in) or <0.1 (rule-out) are impactful.
- Fagan's nomogram visualizes this.
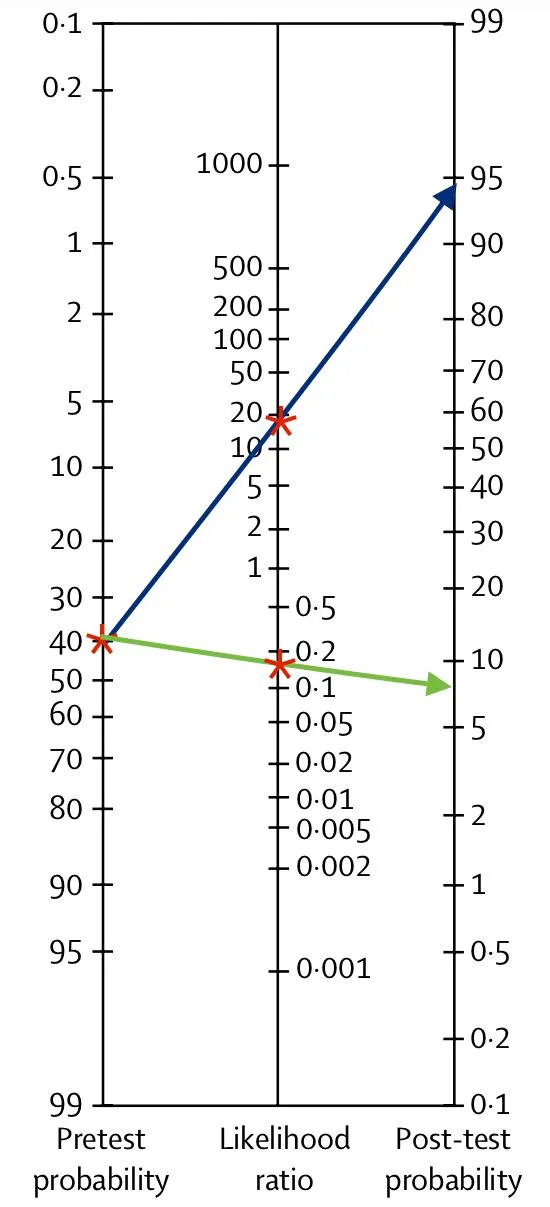
-
Test Selection Factors (📌 "AC AIP"):
- Accuracy (Sens, Spec, LRs)
- Cost
- Availability
- Invasiveness
- Patient values
⭐ Positive Predictive Value (PPV) is highly dependent on the prevalence of the disease in the population being tested.
Diagnostic Pitfalls & Screening - Testing Traps
- Common Diagnostic Biases:
- Confirmation Bias: Seeking data supporting initial hypothesis, ignoring contradictory evidence.
- Availability Bias: Over-relying on easily recalled (recent/dramatic) diagnoses.
- Testing Consequences:
- Overtesting: ↑ false positives, patient anxiety, unnecessary costs, iatrogenic harm.
- Undertesting: Can lead to missed/delayed diagnosis, ↑ morbidity & mortality.
- Principles of Screening:
- Early detection in asymptomatic individuals for significant health problems.
- Test must be accurate, acceptable, safe. Effective treatment must exist.
⭐ The Wilson-Jungner criteria provide a framework for evaluating the appropriateness of a disease screening program.
High‑Yield Points - ⚡ Biggest Takeaways
- Always estimate pre-test probability before ordering any diagnostic test.
- Likelihood Ratios (LRs) are best for assessing how test results change disease probability.
- Sensitivity and Specificity are fixed test properties, independent of prevalence.
- Use high Sensitivity tests to rule out disease (SnNOut).
- Use high Specificity tests to rule in disease (SpPIn).
- PPV and NPV vary significantly with disease prevalence in the population.
- Avoid shotgun testing; select tests to confirm or refute specific hypotheses based on clinical reasoning.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

