Differential Diagnosis Development - Diagnostic DNA
- Foundation: Systematic data (history, exam, tests) & problem representation.
- Hypothesis Generation: Broad initial list from chief complaint & key findings.
- Consider anatomical, physiological, etiological categories.
- Refinement: Narrow using pattern recognition, prevalence, acuity.
- Prioritize: Common, Critical, Curable. 📌
⭐ The 'pivot and cluster' strategy is a key technique in refining differential diagnoses, allowing clinicians to efficiently narrow down possibilities based on key findings.
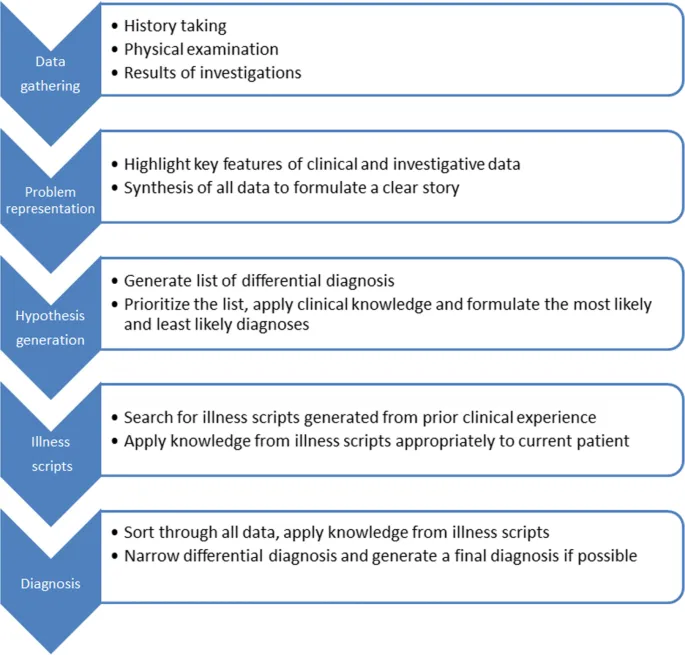
- Verification: Confirm with further tests or response to therapy.
Differential Diagnosis Development - The Detective's Drill
-
Systematic, iterative approach to identify likely diagnosis.
-
Key Strategies:
- Pattern Recognition: Rapid, intuitive.
- Analytical Reasoning: Systematic, for complex cases.
- Prioritize DDx:
- Probable
- Serious (Don't Miss!)
- Treatable
- 📌 DDx Frameworks (e.g., VINDICATE):
- Vascular, Infect/Inflam, Neoplasm, Degenerative, Iatro/Idio, Congenital, Autoimmune, Trauma, Endo/Metabolic.
- Bayes' Theorem (implicit): $P(D+|T+) = [P(T+|D+) * P(D+)] / P(T+)$.
⭐ The iterative process of diagnostic reasoning involves continuous refinement of hypotheses as new clinical data (history, examination, or investigation results) becomes available.
Differential Diagnosis Development - Framework Fanfare
- Employ systematic frameworks to build a comprehensive list of potential diagnoses (DDx).
- Key Approaches:
- Anatomical/Location-based: Localizes the problem. Ask: "Where is the lesion?" (e.g., organ, system).
- Pathophysiological: Identifies the disease process. Ask: "What is the mechanism?" (e.g., inflammation, ischemia, neoplasia).
- Mnemonic-based: Ensures broad etiological consideration; acts as a safety net.
- 📌 VINDICATE: Highly useful (see image for categories).
- Other examples: I VINDICATE AIDS, VITAMINS C&D.
- Integrate multiple frameworks for optimal diagnostic accuracy and to avoid premature closure.
⭐ The VINDICATE mnemonic (Vascular, Inflammatory/Infectious, Neoplastic, Degenerative/Deficiency, Idiopathic/Iatrogenic, Congenital, Autoimmune/Allergic, Traumatic, Endocrine/Metabolic) is a highly tested etiological framework for generating broad differentials in PG entrance exams.

Differential Diagnosis Development - Bias Busters
Cognitive biases: systematic thinking errors affecting diagnosis. Awareness & debiasing are key.
- Anchoring Bias: Over-reliance on initial data.
- Mitigation: Re-evaluate, seek alternatives.
- Availability Heuristic: Recent/vivid cases seem likelier.
- Mitigation: Use objective data, consider prevalence.
- Confirmation Bias: Favoring confirming evidence.
- Mitigation: Seek disconfirming evidence.
- Premature Closure: Early diagnostic acceptance.
- Mitigation: Systematic review, ask "What else?".
- Representativeness Heuristic: Stereotyping cases.
- Mitigation: Consider base rates, atypical forms.
⭐ Anchoring bias, where a clinician over-relies on initial information, and premature closure, accepting a diagnosis before it's fully verified, are two of the most common and impactful cognitive errors in diagnostic reasoning.
High‑Yield Points - ⚡ Biggest Takeaways
- Always prioritize life-threatening conditions (e.g., MI, PE, Aortic dissection).
- Consider common diseases first; atypical presentations are frequent in exams.
- Patient demographics (age, sex) and comorbidities significantly narrow possibilities.
- Utilize frameworks like VINDICATE for a systematic approach to generating differentials.
- Balance Occam's Razor (simplest explanation) with Hickam's Dictum (patients can have multiple diseases).
- Actively look for red flag symptoms indicating serious pathology requiring urgent intervention.
- Avoid premature closure and confirmation bias; always consider alternatives until a diagnosis is firm.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

