Malabsorption Basics - Gut's Big Gulp
- Definition: Impaired intestinal absorption of one or more dietary nutrients.
- Phases of Absorption (L-A-D):
- Luminal: Pancreatic enzymes & bile salts digest food; micelle formation for fats.
- Absorptive (Mucosal): Nutrients cross apical membrane of enterocytes; processing within cell.
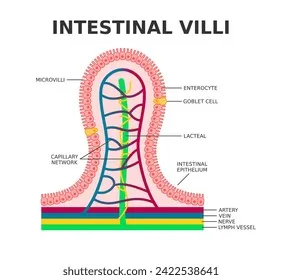
- Delivery (Post-mucosal): Transport via lymphatics (fats, fat-soluble vitamins) & portal vein (others).
- Mechanisms:
- Pre-mucosal (Luminal): Defective hydrolysis/solubilization (e.g., Pancreatic insufficiency, ↓bile salts, ZES, Bacterial overgrowth).
- Mucosal: ↓Surface area, defective enzyme/transport (e.g., Celiac disease, Whipple's, Tropical sprue, Lactase deficiency).
- Post-mucosal: Obstruction of lymphatics (e.g., Lymphoma, Intestinal lymphangiectasia, TB).
⭐ Definition of steatorrhea: >7g fecal fat/24h on a 100g fat/day diet.
Symptom Spectrum - Telltale Tummy
⭐ Weight loss despite adequate or increased oral intake is a hallmark of malabsorption.
- Key GI Symptoms:
- Chronic diarrhea, often steatorrhea (bulky, pale, foul-smelling, greasy stools)
- Abdominal distension, bloating, ↑flatus, borborygmi
- Weight loss (adults), failure to thrive (children), fatigue, anorexia
- Nutrient Deficiency Clues (Systemic Impact):
- Anemia (↓Fe, ↓B12, ↓folate): pallor, glossitis, angular stomatitis
- Bleeding (↓Vit K): easy bruising, petechiae, purpura
- Bone pain/fractures (↓Vit D, ↓Ca): osteomalacia, osteoporosis
- Neurological (↓B12, ↓Thiamine): paresthesias, ataxia; Tetany (↓Ca, ↓Mg)
- Edema (↓protein)
- Skin/Mucosal (↓Vitamins, ↓Zinc): dermatitis (e.g., herpetiformis in celiac), hyperkeratosis (↓Vit A), night blindness (↓Vit A)
Diagnostic Toolkit - Gut Sleuthing
- Initial Clues:
- Blood tests: CBC (anemia), Albumin (↓), Ca (↓), Vit D (↓), PT (↑).
- Fat Malabsorption:
- Sudan III stain (stool, qualitative).
- ⭐ > The gold standard for diagnosing fat malabsorption is quantitative 72-hour fecal fat estimation (>7g/day abnormal).
- Carbohydrate Malabsorption:
- D-xylose test: Distinguishes mucosal vs. pancreatic.
- Normal: >25mg/dL (2h serum), >4g (5h urine).
- Low in mucosal disease.
- Hydrogen breath tests (lactose intolerance; glucose for SIBO).
- D-xylose test: Distinguishes mucosal vs. pancreatic.
- Protein Malabsorption: Fecal α1-antitrypsin (protein-losing enteropathy).
- SIBO: Jejunal aspirate (>10^5 CFU/mL).
Spotlight Syndromes - Rogues' Gallery
| Feature | Celiac Disease | Tropical Sprue | Whipple's Disease |
|---|---|---|---|
| Etiology | Gluten sensitivity (HLA-DQ2/DQ8) | ?Infectious; post-infectious enteropathy | Tropheryma whipplei (Gram+ actinomycete) |
| Key Clinical | Diarrhea, wt loss, anemia, dermatitis herpetiformis | Chronic diarrhea, steatorrhea, megaloblastic anemia (folate/B12↓) | Arthralgia, wt loss, diarrhea, neuro sx (📌 WAND: Wt loss, Arthralgia, Neuro sx, Diarrhea) |
| Dx Markers | Anti-tTG IgA, Anti-EMA, Anti-DGP; HLA-DQ2/DQ8 | ↓ Folate, ↓ B12; exclusion | PCR for T. whipplei |
| Biopsy | Villous atrophy, crypt hyperplasia, ↑IELs | Partial villous atrophy, ↑IELs, chronic inflammation | PAS+ macrophages in lamina propria |
| Treatment | Lifelong gluten-free diet (GFD) | Tetracycline + Folic acid (months) | Prolonged antibiotics (Ceftriaxone then TMP-SMX) |
⭐ Anti-tissue transglutaminase (Anti-tTG) IgA antibodies are the most sensitive and specific serological screening test for Celiac Disease.
High‑Yield Points - ⚡ Biggest Takeaways
- Celiac Disease: HLA-DQ2/DQ8 linked; anti-TTG IgA antibodies; villous atrophy on biopsy.
- Tropical Sprue: Endemic areas; chronic diarrhea, malabsorption; responds to tetracycline & folic acid.
- Whipple's Disease: T. whipplei; arthralgia, weight loss, diarrhea, neurological symptoms; PAS-positive macrophages.
- Pancreatic Insufficiency: Steatorrhea; low fecal elastase-1; enzyme replacement therapy.
- SIBO: Diagnosed by carbohydrate breath tests (glucose/lactulose) or jejunal aspirate culture.
- D-xylose test: Differentiates mucosal disease (impaired absorption) from pancreatic insufficiency (normal absorption).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

