IBS Basics - Gut Feeling Gone Wrong
- Chronic functional GI disorder: Recurrent abdominal pain, altered bowel habits (diarrhea, constipation, or mixed). No organic pathology.
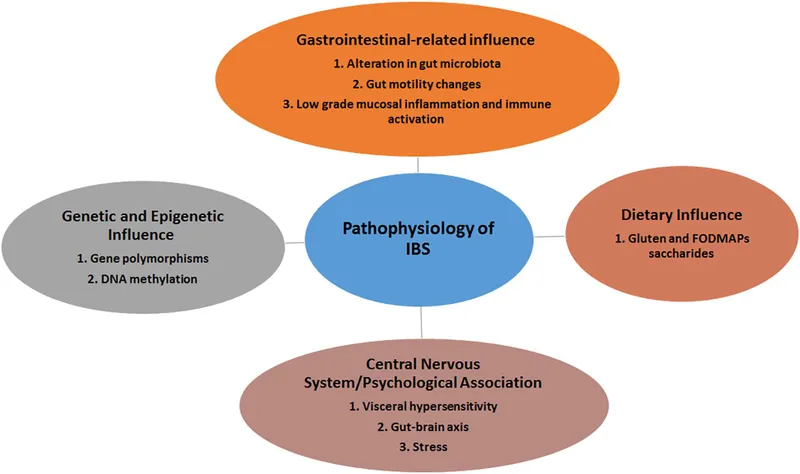
- Pathophysiology: Gut-brain axis dysfunction, visceral hypersensitivity, altered motility, gut microbiota dysbiosis, low-grade inflammation.
- Risk Factors: Genetics, stress, prior gastroenteritis (Post-Infectious IBS or PI-IBS), food intolerances.
- Epidemiology: Affects ~10-15% of population; Female > Male.
⭐ Post-infectious IBS (PI-IBS) can develop in up to 20% of individuals after an episode of acute gastroenteritis.
- Diagnosis of exclusion, based on symptom criteria (e.g., Rome IV).
Why Me? - IBS Inner Workings
- Gut-Brain Axis Dysregulation: Core issue; bidirectional CNS-ENS miscommunication.
- Psychological factors (stress, anxiety) significantly influence symptoms.
- Serotonin (5-HT) signaling alterations impact motility and sensation.
- Altered Gut Motility:
- IBS-D: Accelerated colonic transit.
- IBS-C: Delayed colonic transit.
- Visceral Hypersensitivity: Heightened pain perception from normal gut stimuli.
- Nerve endings in gut wall are oversensitive.
- Gut Microbiota Imbalance (Dysbiosis):
- Altered bacterial composition; Small Intestinal Bacterial Overgrowth (SIBO) link.
- Low-Grade Inflammation & Immune Activation:
- Subtle inflammation, ↑ mast cells, ↑ intestinal permeability ("leaky gut").
⭐ Post-infectious IBS (PI-IBS) develops in a subset of patients (approx. 10-20%) following an episode of acute bacterial gastroenteritis.
Spotting IBS - Symptom Sleuthing
- Core: Recurrent abdominal pain, altered bowel habits (diarrhea/constipation/mixed).
- Rome IV Criteria (symptom onset ≥6 mo prior; active for last 3 mo):
- Recurrent abd. pain (≥1 day/wk)
- Associated with ≥2 of:
- Pain linked to defecation
- Stool frequency change
- Stool form change (Bristol)
- Subtypes (Bristol):
- IBS-C: >25% hard, <25% loose stools
- IBS-D: >25% loose, <25% hard stools
- IBS-M: >25% hard & >25% loose
- IBS-U: Unsubtyped
- ⚠️ Alarm Features (Red Flags):
- Onset >50 yrs, weight loss, nocturnal sx
- Rectal bleeding, Fe def. anemia
- Fam Hx: IBD, celiac, CRC
⭐ Rome IV: Key for diagnosis; positive criteria, not just exclusion.
Not Just IBS - Ruling Rivals Out
- Key: Exclude organic pathology. Watch for alarm features:
- Weight loss, rectal bleeding, anemia
- Nocturnal symptoms, family Hx (CRC/IBD), age >50
- IBD (Crohn's/UC): Endoscopy, biopsy.
- Celiac Disease: Serology (anti-tTG), biopsy.
- Infections (India): Amoebiasis, Giardiasis. Stool tests.
- Lactose Intolerance: H2 breath test.
- Colorectal Cancer: Colonoscopy if alarm signs.
- Microscopic Colitis: Biopsy essential.
⭐ Nocturnal diarrhea is a key red flag pointing away from IBS towards organic causes like IBD or microscopic colitis.
Taming the Tumult - IBS Treatment Toolkit
- Foundation: Reassurance, education, regular physical activity.
- Dietary: Low FODMAP diet trial (key for bloating/pain).
- Pharmacotherapy (Subtype-Guided):
- IBS-C: Soluble fiber (psyllium), PEG; Lubiprostone, Linaclotide if needed.
- IBS-D: Loperamide (acute); Rifaximin (550mg TID x 14d); Eluxadoline. Alosetron (severe, ♀, REMS).
- Abdominal Pain: Antispasmodics (Dicyclomine), Peppermint oil. Low-dose TCAs (Amitriptyline 10-25mg).
- Psychological: CBT, hypnotherapy, stress management.
⭐ Rifaximin, a gut-selective antibiotic, offers durable relief of bloating and abdominal pain in non-constipated IBS (IBS-D/M).
High‑Yield Points - ⚡ Biggest Takeaways
- Rome IV criteria for diagnosis: recurrent abdominal pain related to defecation, or change in stool frequency/form.
- Subtypes: IBS-C (constipation-predominant), IBS-D (diarrhea-predominant), IBS-M (mixed).
- A functional bowel disorder; diagnosis of exclusion. Rule out organic disease.
- Red flag symptoms (weight loss, bleeding, anemia) necessitate further investigation.
- Management: low FODMAP diet, lifestyle changes, antispasmodics, loperamide, laxatives.
- Pathophysiology involves visceral hypersensitivity, altered gut motility, and gut-brain axis dysfunction.
- Often associated with psychological distress (anxiety, depression).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more