Upper GI Malignancies - Top Tract Terrors
Esophageal Carcinoma:
- Two main types:
- Squamous Cell Ca (SCC): Mid-upper esophagus. Risks: Smoking, alcohol, achalasia, Plummer-Vinson, hot liquids. 📌 AAH SP! (Alcohol, Achalasia, Hot liquids, Smoking, Plummer-Vinson)
- Adenocarcinoma (ADC): Lower third. Arises from Barrett's esophagus (columnar metaplasia). Risks: GERD, obesity, smoking.
- Clinical: Progressive dysphagia (solids then liquids), weight loss, odynophagia.
⭐ In ADC, Barrett's esophagus (intestinal metaplasia) increases cancer risk by 30-40 times.
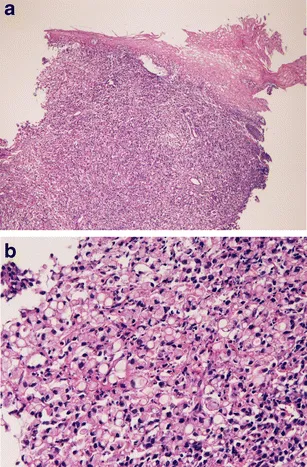
Gastric Adenocarcinoma:
- Lauren Classification:
- Intestinal type: Glandular, common in high-risk areas, assoc. H. pylori, chronic gastritis, dietary nitrosamines.
- Diffuse type: Signet ring cells, infiltrative (linitis plastica), worse prognosis, CDH1 mutation.
- Risk Factors: H. pylori (key!), smoked/salted foods, pernicious anemia, Blood group A.
- Signs: Virchow's node (supraclavicular LN), Sister Mary Joseph nodule (umbilical), Krukenberg tumor (ovarian mets).
Colorectal Cancer - Colon Catastrophe
- Risk: Age >50, IBD, family hx, adenomatous polyps (villous > tubular), ↓fiber/↑red meat.
- Features:
- Right-sided: Iron deficiency anemia, occult blood.
- Left-sided: Altered bowel habits, rectal bleeding, obstruction. 📌 "Apple core" lesion.
- Screening (Avg Risk, age 45): Colonoscopy (gold std) q10yrs; FIT annually.
- Hereditary:
- FAP (APC gene): 1000s polyps; CRC ~100% by 40; prophylactic colectomy.
- Lynch (HNPCC): DNA mismatch repair genes (MLH1, MSH2); ↑CRC & endometrial Ca.
- Staging: TNM. CEA for prognosis/recurrence. Treatment: Surgery ± Chemo.
⭐ Right-sided colon cancers often present with anemia, while left-sided cancers are more likely to cause changes in bowel habits or obstruction.
Hepatocellular Carcinoma - Liver Lesion Lore
- Risk Factors: Chronic HBV/HCV, Cirrhosis (Alcohol, NAFLD), Aflatoxin B1, Hemochromatosis. 📌 Hepatitis, Cirrhosis, Contaminants (Aflatoxin).
- Screening: Cirrhotics & high-risk HBV: Ultrasound +/- AFP every 6 months.
- Diagnosis:
- AFP: ↑ (>20 ng/mL abnormal; >400 ng/mL highly suggestive).
- Imaging (LI-RADS): Arterial Phase Hyperenhancement (APHE) & Venous/Delayed Phase Washout on CT/MRI.
- Biopsy: If imaging atypical or no underlying cirrhosis.
- Staging: Barcelona Clinic Liver Cancer (BCLC).
- Treatment: Resection, Transplant, Ablation (RFA), TACE, Sorafenib/Lenvatinib.
⭐ In a patient with cirrhosis, a liver lesion >1 cm showing APHE and washout on dynamic imaging (CT/MRI) is diagnostic of HCC (LI-RADS 5), often without needing biopsy.

Pancreatic Cancer - Pancreas Peril

- Risk Factors: Smoking (strongest), chronic pancreatitis, diabetes mellitus, obesity, family history (e.g., BRCA mutations).
- Clinical Features:
- Painless, progressive obstructive jaundice (esp. head of pancreas).
- Significant weight loss, anorexia, abdominal/back pain.
- Courvoisier's sign: Palpable, non-tender gallbladder with jaundice.
- Trousseau's sign: Migratory thrombophlebitis.
- New-onset diabetes mellitus in elderly.
- Investigations:
- Tumor marker: CA 19-9 (↑, monitor response, not for screening).
- USG Abdomen: Initial, may show mass, dilated CBD/pancreatic duct.
- CECT Abdomen: Preferred for diagnosis, staging, assessing resectability. "Double duct" sign.
- EUS with FNA: For tissue diagnosis, especially for smaller tumors or when CECT is equivocal.
- Management:
- Surgical resection (e.g., Whipple procedure for head tumors) is the only curative option.
- Adjuvant/Neoadjuvant chemotherapy (e.g., FOLFIRINOX).
- Palliative care for unresectable/metastatic disease (ERCP stenting, chemotherapy, pain management).
⭐ Courvoisier's Law: A palpably enlarged, non-tender gallbladder in a jaundiced patient suggests malignant obstruction (e.g., pancreatic or periampullary cancer) rather than gallstones.
High‑Yield Points - ⚡ Biggest Takeaways
- Esophageal SCC, common in India, linked to tobacco/betel nut; Adenocarcinoma with GERD/Barrett's.
- Gastric cancer: H. pylori is a key risk; signet ring cells & linitis plastica mean poor prognosis.
- Colorectal cancer (CRC): Screening colonoscopy is vital. FAP & Lynch syndrome are key hereditary causes.
- Hepatocellular carcinoma (HCC): Hepatitis B is main cause in India; AFP is the marker.
- Pancreatic cancer: Presents with painless jaundice (head); CA 19-9 marker. Courvoisier's sign.
- GISTs: c-KIT (CD117) positive; treat with Imatinib.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

