GI Bleed Basics - Red Alert Regions
- Classification:
- Upper GI Bleed (UGIB): Proximal to Ligament of Treitz.
- Symptoms: Hematemesis (fresh/coffee-ground), melena.
- Lower GI Bleed (LGIB): Distal to Ligament of Treitz.
- Symptoms: Hematochezia (bright red/maroon). Melena if slow bleed/proximal LGIB.
- Overt vs. Occult (FOBT+, Iron Deficiency Anemia).
- Upper GI Bleed (UGIB): Proximal to Ligament of Treitz.
- Severity Assessment & Initial Management:
- ABCDE: Secure airway, IV access (2 large-bore cannulae).
- Hemodynamic status: Tachycardia, hypotension.
⭐ Orthostatic hypotension (↓SBP >20 mmHg / ↓DBP >10 mmHg / ↑Pulse >20 bpm on standing) indicates ~15-20% volume loss.
- Resuscitation: Crystalloids, blood (Target Hb >7 g/dL; >9 g/dL in CAD).
- Risk Stratification: Rockall, Glasgow-Blatchford Score (GBS).
- Key History/Exam:
- Drugs (NSAIDs, anticoagulants, antiplatelets), alcohol, H/O PUD, liver disease.
- Stigmata of CLD, Digital Rectal Exam (DRE).
Upper GI Bleed - Above the Ligament
Bleeding proximal to Ligament of Treitz. Manifests as hematemesis (fresh red blood/coffee grounds) or melena.
- Common Causes: 📌 Peptic Ulcer Disease (PUD ~50%), Esophageal Varices (~10-20%), Mallory-Weiss tear (~5-10%), Erosive gastritis/duodenitis, Malignancy.
- Risk Stratification:
- Glasgow-Blatchford Score (GBS): Pre-endoscopy. Uses BUN, Hb, SBP, pulse, melena, syncope, hepatic disease, cardiac failure. Score >0 indicates high risk.
- Rockall Score: Pre- & post-endoscopy. Assesses age, shock, co-morbidity, diagnosis, stigmata of recent hemorrhage (SRH).
- General Management Approach:
- Resuscitation: IV fluids, blood (target Hb >7 g/dL).
- Endoscopy (OGD) within 24 hrs (urgent <12 hrs if unstable or variceal suspected).
- Non-Variceal Bleed:
- PPI: Pantoprazole 80mg IV bolus, then 8mg/hr infusion.
- Endoscopic therapy (e.g., clips, thermal) based on Forrest classification for PUD.
- Suspected Variceal Bleed:
- Vasoactive drugs (Octreotide/Terlipressin) + prophylactic antibiotics (e.g., Ceftriaxone) before endoscopy.

⭐ In suspected variceal bleeding, vasoactive drugs (e.g., Octreotide 50mcg bolus then 50mcg/hr, or Terlipressin) should be started before endoscopy and continued for 3-5 days post-procedure.
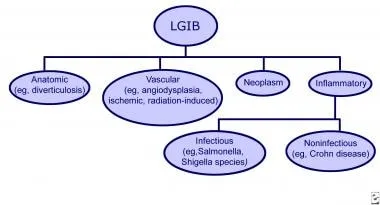
Lower GI Bleed - Below the Belt Bleeds
Bleeding distal to Ligament of Treitz. Presents as hematochezia (BRBPR), maroon stools.
-
Causes: 📌 DANCHeS
- Diverticulosis: Most common major LGIB; painless.
- Angiodysplasia: Vascular ectasias; older; right colon; recurrent.
- Neoplasms/Polyps: CRC, adenomas; occult/overt.
- Colitis: IBD, Infectious, Ischemic (elderly, watershed).
- Hemorrhoids/Fissures: Common; BRBPR on TP; pain (fissure).
- eS (Etc.): Meckel's (younger), post-polypectomy, radiation proctitis.
-
Diagnosis & Localization:
- Initial: ABCs, exclude UGIB (NGT if needed).
- Colonoscopy: Preferred initial test if stable; diagnostic & therapeutic.
- If active/recurrent bleed & colonoscopy non-diagnostic/not feasible:
- CTA: Rapid, detects bleed >0.3-0.5 mL/min.
- Tagged RBC scan: Detects slow/intermittent bleed (0.1-0.5 mL/min).
- Angiography: Diagnostic (bleed >0.5-1.0 mL/min) & therapeutic (embolization).
⭐ Tagged RBC scan is useful for detecting bleeding rates as low as 0.1-0.5 mL/min, while angiography requires 0.5-1.0 mL/min.
- Management:
- Resuscitation: IV access, fluids, blood (transfuse if Hb <7 g/dL; <8-9 g/dL if CAD/active bleed).
- Endoscopic therapy: Clips, thermal, epinephrine.
- Interventional Radiology: Angioembolization.
- Surgery: For failed endoscopic/IR therapy, persistent instability.
High‑Yield Points - ⚡ Biggest Takeaways
- UGIB is commoner; Peptic Ulcer Disease (PUD) is the top cause.
- LGIB's main cause in adults is Diverticulosis.
- Manage with ABCs, IV fluids, PPI; transfuse if Hb < 7 g/dL.
- Glasgow-Blatchford Score (GBS) (pre-endoscopy) & Rockall score (post-endoscopy) assess UGIB risk.
- Endoscopy is key for UGIB diagnosis and treatment.
- Use Octreotide for suspected variceal bleeds.
- Differentiate Hematemesis (acidic pH) from Hemoptysis (alkaline pH).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

