Motility Disorders - Movement Mayhem
-
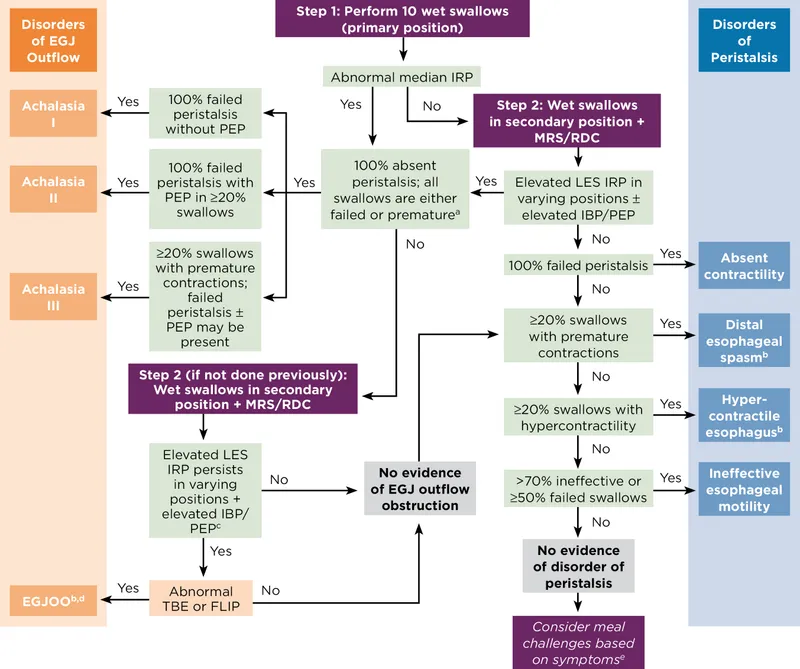
Disorders of esophageal peristalsis or Lower Esophageal Sphincter (LES) function causing dysphagia and/or chest pain. Manometry is the gold standard for diagnosis.
-
Achalasia:
- Patho: Loss of inhibitory ganglion cells in myenteric plexus → impaired LES relaxation & aperistalsis.
- Dx: Barium swallow (bird’s beak), Manometry (↑LES pressure, incomplete LES relaxation, aperistalsis).
- Tx: Pneumatic dilation, Heller myotomy, Peroral Endoscopic Myotomy (POEM), Botulinum toxin.
-
Diffuse Esophageal Spasm (DES):
- Sx: Intermittent dysphagia, non-cardiac chest pain.
- Dx: Manometry (simultaneous, premature contractions in >20% of wet swallows); Barium (corkscrew/rosary bead - uncommon).
-
Nutcracker Esophagus (Hypertensive Peristalsis):
- Sx: Chest pain, dysphagia.
- Dx: Manometry (normal peristalsis, high amplitude contractions >180 mmHg).
-
Ineffective Esophageal Motility (IEM):
- Dx: Manometry (>50% ineffective swallows: low amplitude or failed peristalsis).
⭐ Pseudoachalasia, often due to malignancy (e.g., gastric cardia cancer), can mimic achalasia. Suspect in older patients with rapid onset dysphagia and significant weight loss. Investigate with EGD and CT scan.
GERD & Inflammation - Fiery Fallout
- GERD: Symptoms or mucosal damage from gastric acid reflux. Patho: ↓LES tone, Transient LES Relaxations (TLESRs), hiatus hernia. Sx: Heartburn (pyrosis), regurgitation. Alarm Sx: Dysphagia, odynophagia, weight loss, GI bleeding, anemia.
- Diagnosis: Empiric PPI trial; Upper Endoscopy (if alarm Sx, refractory, or screening for Barrett's); 24-hr ambulatory pH monitoring (gold standard if endoscopy normal but high suspicion).
- Complications: Erosive esophagitis, peptic strictures, Barrett's esophagus (intestinal metaplasia), esophageal adenocarcinoma.
⭐ Barrett's esophagus: Intestinal metaplasia (goblet cells present) in the distal esophagus; a premalignant condition for esophageal adenocarcinoma, requiring endoscopic surveillance.
- Management: Lifestyle modification (weight loss, head elevation), Antacids, H2-receptor antagonists, PPIs (most effective). Anti-reflux surgery (e.g., Nissen fundoplication) for refractory cases.
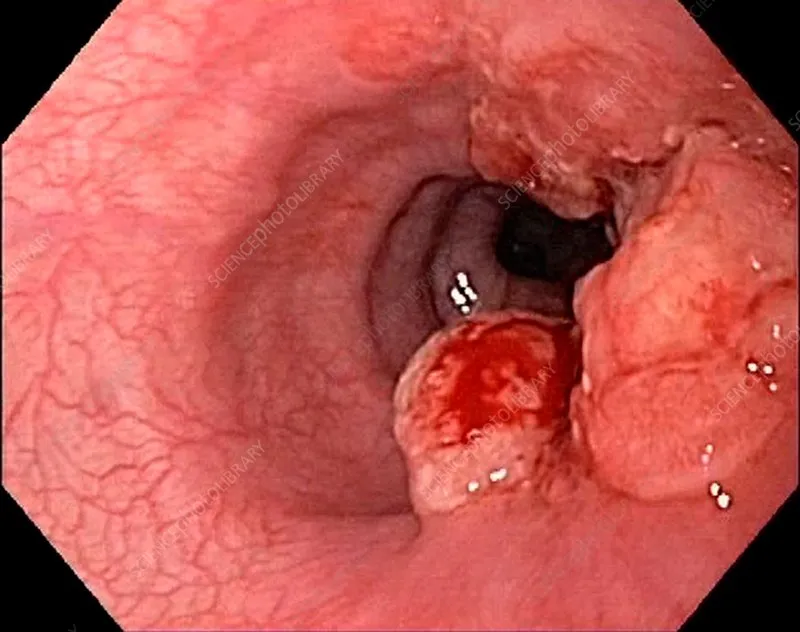
- Eosinophilic Esophagitis (EoE): Chronic, immune/antigen-mediated. Sx: Dysphagia (especially solids), food impaction. Dx: Endoscopy (rings, furrows, exudates) + Biopsy (≥15 eosinophils/HPF in at least one biopsy).
Structural Issues - Anatomic Anomalies
- Esophageal Webs & Rings
- Webs: Thin, mucosal folds; upper/mid esophagus.
- 📌 Plummer-Vinson Syndrome (PVS): Cervical webs, iron-deficiency anemia, dysphagia, koilonychia, glossitis.
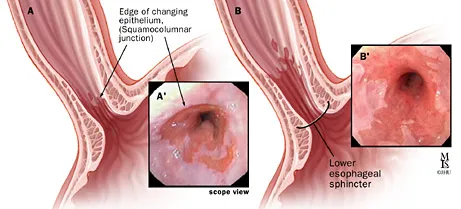
- Rings: Concentric, smooth, thin; lower esophagus.
- Schatzki Ring (B-ring): Most common; at squamocolumnar junction (SCJ); causes intermittent dysphagia (steakhouse syndrome).
- A-ring: Muscular ring, proximal to SCJ.
- Webs: Thin, mucosal folds; upper/mid esophagus.
- Diverticula
- Zenker's (Pharyngoesophageal): False diverticulum; posterior hypopharynx (Killian's dehiscence). Halitosis, dysphagia, regurgitation.
- Killian-Jamieson: Anterolateral, below cricopharyngeus.
- Traction: Mid-esophagus; true diverticulum; due to external inflammation (e.g., TB).
- Epiphrenic: Distal esophagus; often with motility disorders.
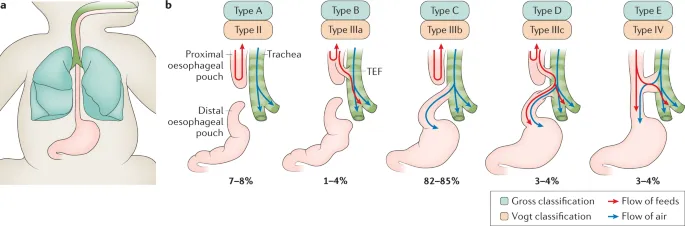
- Tracheoesophageal Fistula (TEF) / Esophageal Atresia (EA)
- Congenital; various types (Gross classification).
- Type C (EA with distal TEF) most common (>85%).
- Symptoms: Coughing, choking, cyanosis with feeds; polyhydramnios history.
⭐ Schatzki ring is the most common cause of intermittent solid food dysphagia in adults, typically when esophageal lumen is <13 mm.
Tumors & Trauma - Grave Conditions
-
Esophageal Cancer:
- Types: Squamous Cell Ca (SCC, mid-upper), Adenocarcinoma (AdenoCA, lower).
- SCC Risks: Smoking, Alcohol, Achalasia, Plummer-Vinson syndrome.
- AdenoCA Risks: Barrett's esophagus, GERD, Obesity.
- Sx: Progressive dysphagia (solids→liquids), weight loss.
- Dx: Endoscopy + Biopsy. Staging: CT, EUS, PET.
-
Trauma:
- Boerhaave Syndrome: Transmural rupture, often post-forceful emesis.
- Mackler's Triad (📌): Vomiting, chest pain, subcutaneous emphysema.
- Dx: CXR (pneumomediastinum), CT, Gastrografin swallow. Tx: Emergent surgery, antibiotics.
- Mallory-Weiss Tear: Mucosal tear (GEJ), often post-forceful retching/vomiting.
- Sx: Hematemesis.
- Dx: Endoscopy. Tx: Often self-limiting; endoscopic therapy if severe bleeding.
- Boerhaave Syndrome: Transmural rupture, often post-forceful emesis.
⭐ Adenocarcinoma is the most common type of esophageal cancer in many developed nations, strongly associated with Barrett's esophagus and chronic GERD.
High‑Yield Points - ⚡ Biggest Takeaways
- GERD: Most common cause is transient LES relaxations; PPIs are mainstay therapy.
- Barrett's esophagus: Intestinal metaplasia (goblet cells); risk for esophageal adenocarcinoma.
- Achalasia: "Bird-beak" on barium; absent peristalsis and incomplete LES relaxation on manometry.
- Eosinophilic esophagitis: Ringed esophagus ("trachealization"); >15 eosinophils/HPF on biopsy.
- Plummer-Vinson syndrome: Triad: iron-deficiency anemia, dysphagia (esophageal webs), glossitis.
- Boerhaave syndrome: Transmural esophageal rupture post-emesis; presents with Hamman's sign (mediastinal crunch).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

