Diving Physics & Physiology - Pressure Problems
- Core Gas Laws:
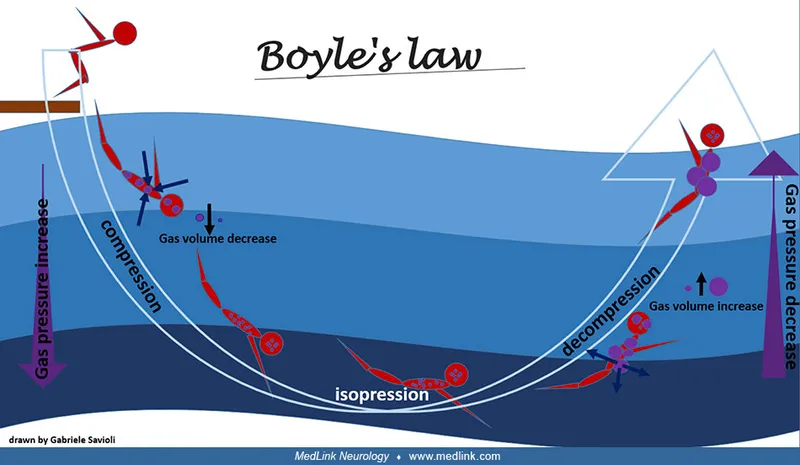
- Boyle's Law: $P_1V_1 = P_2V_2$. Volume inversely proportional to pressure. Critical for barotrauma.
- Dalton's Law: $P_{total} = \Sigma P_{partial}$. Total pressure is sum of partial pressures of gases. Explains gas toxicities.
- Henry's Law: Amount of dissolved gas in a liquid is proportional to its partial pressure. Key for Decompression Sickness (DCS) & narcosis.
- Pressure-Related Problems:
- Barotrauma: Physical tissue damage from pressure differences.
- Descent (Squeeze): Ears (most common), sinuses, lungs, mask.
- Ascent (Reverse Block/Expansion): Lungs (pneumothorax, Arterial Gas Embolism - AGE), GI tract, teeth.
- Nitrogen Narcosis: Impaired judgment/coordination at depth (typically >30m). "Martini's Law": each 10-15m depth beyond 30m feels like one alcoholic drink.
- Oxygen Toxicity: CNS (seizures, visual changes) or pulmonary effects from high partial pressures of oxygen ($P_{O_2}$), e.g., >1.4 ATA.
- Barotrauma: Physical tissue damage from pressure differences.
⭐ Boyle's Law ($P \propto 1/V$) is the cornerstone for understanding barotrauma; as pressure increases during descent, gas volume in uncompensated spaces decreases, causing "squeeze" injuries.
Decompression Illness (DCI) - Bubble Trouble
- Pathophys: $N_2$ dissolved under ↑dive pressure forms bubbles in tissues/bloodstream during ascent as pressure ↓ (Henry's & Boyle's Laws).
- DCI Spectrum:
- Decompression Sickness (DCS): $N_2$ bubbles in tissues.
- Type I (Mild): Joint pain ("bends"), skin (mottling, pruritus), lymphedema, fatigue.
- Type II (Serious): Neurological (spinal: paralysis, paresthesia, bladder dysfunction - "staggers"; cerebral: confusion), pulmonary ("chokes"), vestibular ("leans").
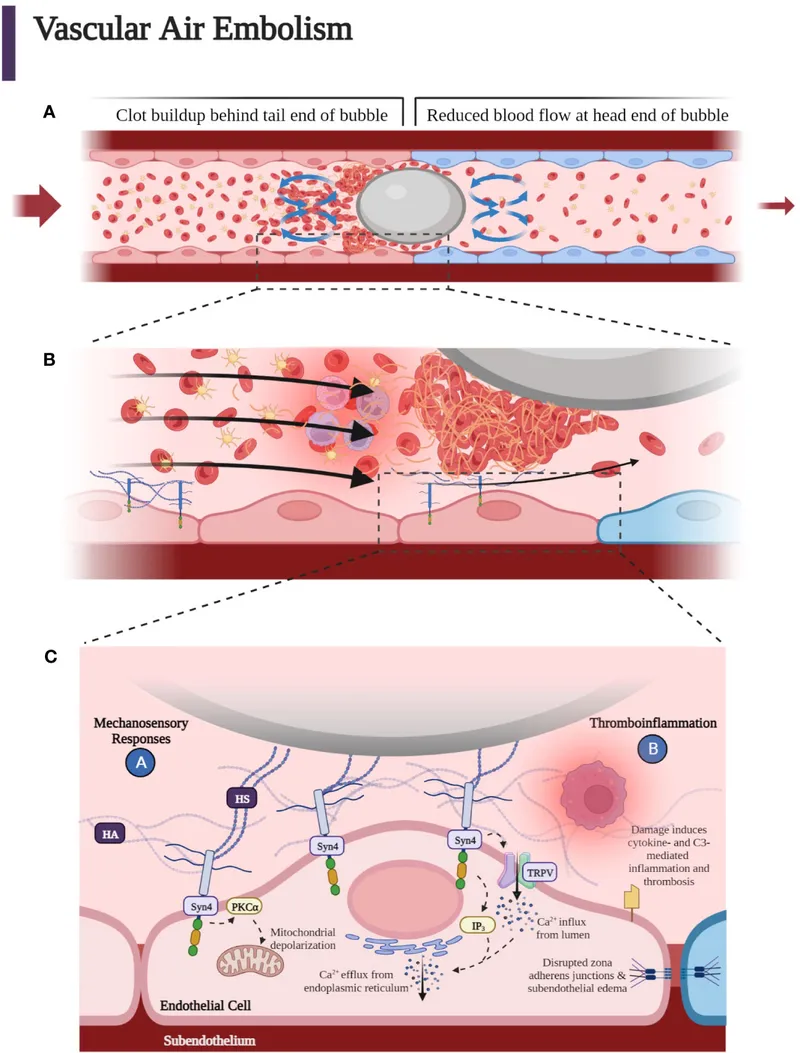
- Arterial Gas Embolism (AGE): Gas bubbles in arterial circulation (often from pulmonary barotrauma).
- Sudden, dramatic onset (<10 min post-surface). Stroke-like deficits, LOC, seizures, CV collapse.
- Decompression Sickness (DCS): $N_2$ bubbles in tissues.
⭐ Patent Foramen Ovale (PFO) significantly ↑ risk of serious, "undeserved" DCI (paradoxical embolism).
- Management:
- Immediate: 100% $O_2$ (high-flow), IV fluids, supine. Monitor vitals. Urgent transport to hyperbaric facility.
- Definitive: Recompression (Hyperbaric Oxygen Therapy - HBO) is crucial.
- Prevention: Slow ascent rates (<9-18 m/min), safety stops, dive tables/computers, hydration.
Barotrauma & Gas Toxicities - Squeeze & Poison
Barotrauma (Boyle's Law: $P \propto 1/V$): Pressure-induced tissue injury.
- Descent (Squeeze): Ambient P > Cavity P.
- Middle Ear (commonest): Eustachian tube block. Teed Score (0-5). Pain, ↓hearing.
- Sinus, Mask, Dental.
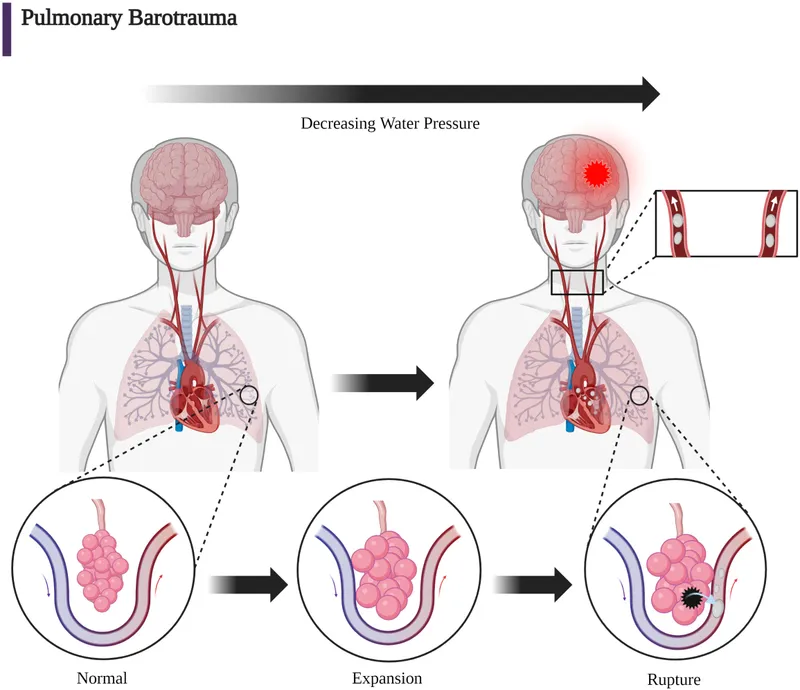
- Ascent (Expansion): Cavity P > Ambient P.
- Pulmonary (PBT): Breath-holding. Risk: AGE, Pneumothorax, Emphysema.
- ⭐ > AGE: Neurological deficits (stroke-like) <20 min post-surfacing. Critical!
- GI, Dental.
AGE Management:
Gas Toxicities:
- N₂ Narcosis: ↑$P_{N_2}$ >30 msw. Euphoria, impaired judgment. Tx: Ascend.
- O₂ Toxicity:
- CNS (Paul Bert): Acute, $P_{O_2}$ >1.6 ATA. 📌 VENTID-C (Convulsions, etc.).
- Pulmonary (Lorraine Smith): Chronic, $P_{O_2}$ >0.5 ATA. Cough, dyspnea.
- CO₂ Toxicity (Hypercapnia): Poor ventilation. Headache, dyspnea.
- CO Toxicity: Contaminated air. Headache, nausea. Tx: 100% O₂, HBO.
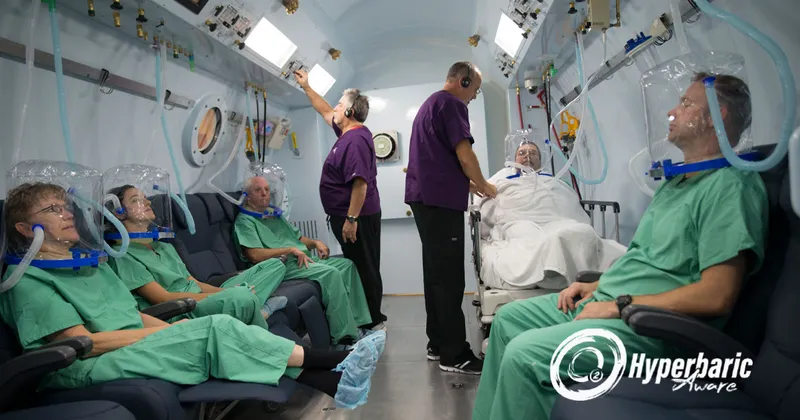
Hyperbaric Oxygen Therapy (HBOT) - Healing with Pressure
- Administering 100% $O_2$ at >1 Atmosphere Absolute (ATA), typically 2-3 ATA.
- Mechanisms:
- ↑ Tissue $O_2$ partial pressure (Henry's Law).
- Vasoconstriction (↓ edema, ↓ Intracranial Pressure).
- Antimicrobial effects, promotes angiogenesis & wound healing.
- Primary Diving Uses:
- Decompression Sickness (DCS).
- Arterial Gas Embolism (AGE).
- Other Major Uses: Carbon Monoxide poisoning, clostridial myonecrosis (gas gangrene), problem wounds (e.g., diabetic foot ulcers), radiation necrosis.
- Absolute Contraindication: Untreated pneumothorax.
- Common Side Effects: Middle ear/sinus barotrauma, $O_2$ toxicity (CNS/pulmonary), reversible myopia.
⭐ For DCS and AGE, HBOT reduces gas bubble volume (Boyle's Law) and enhances oxygen delivery to ischemic tissues, making it the cornerstone of treatment.
High‑Yield Points - ⚡ Biggest Takeaways
- Decompression Sickness (DCS): From rapid ascent (nitrogen bubbles); Type I (pain), Type II (neuro/cardiopulmonary).
- Arterial Gas Embolism (AGE): Most serious; from pulmonary barotrauma on ascent; sudden neuro deficits.
- Nitrogen Narcosis: At depths >30m; impaired judgment, reversible.
- Oxygen Toxicity: Can cause CNS seizures or pulmonary damage.
- HBOT Indications: DCS, AGE, CO poisoning, gas gangrene, non-healing diabetic wounds.
- Boyle's Law: Explains barotrauma (ear, sinus, lung squeeze).
- Untreated pneumothorax: Absolute contraindication to HBOT_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

