Endo HTN Overview - Suspect & Screen
Secondary HTN from hormone excess. Affects 5-10% of hypertensive patients. Early identification crucial.
Clinical Clues:
- Resistant HTN (≥3 drugs, or controlled on ≥4)
- Severe HTN (BP >180/110 mmHg) or abrupt onset
- Young age (<30 yrs) without family history/obesity
- HTN with hypokalemia (unprovoked/diuretic-induced)
- Adrenal incidentaloma
- Paroxysmal HTN, palpitations, pallor, perspiration (Pheochromocytoma - 📌 4 P's)
- Cushingoid features, striae, easy bruising
Initial Screening Approach:
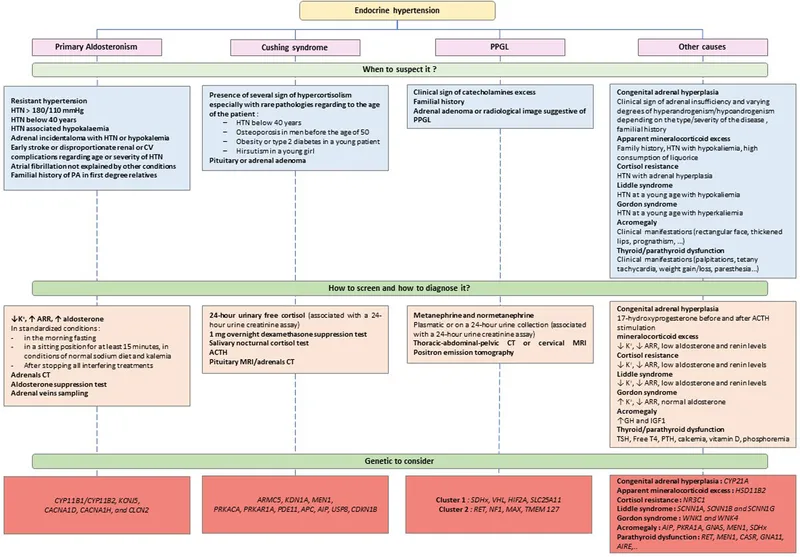
⭐ Primary Aldosteronism (PA) is the most common cause of endocrine hypertension, accounting for ~50-60% of cases.
Primary Aldosteronism - Salty Spies
- Pathophysiology: Autonomous aldosterone secretion → Na⁺ retention, K⁺ excretion, ↓renin, HTN.
- Causes:
- Bilateral Idiopathic Hyperplasia (IHA, ~60%)
- Aldosterone-Producing Adenoma (APA/Conn's, ~35%)
- Clinical: Resistant HTN, ± hypokalemia (muscle weakness), metabolic alkalosis.
- Diagnosis:
- Screening: ↑Aldosterone-Renin Ratio ($ARR$) > 20-30 (Plasma Aldosterone Concentration [PAC] > 10-15 ng/dL, Plasma Renin Activity [PRA] < 1 ng/mL/hr).
- Confirmatory: Saline suppression test (post-saline aldosterone > 5-10 ng/dL).
- Localization: Adrenal CT. Adrenal Vein Sampling (AVS) for lateralization (APA vs IHA).
- Management:
- APA: Unilateral adrenalectomy.
- IHA: Mineralocorticoid Receptor Antagonists (MRAs) e.g., Spironolactone, Eplerenone.
📌 Mnemonic - CONN'S: Causes HTN, Out K⁺, Na⁺ retention, No Renin, Spironolactone/Surgery.
⭐ Despite classic teaching, hypokalemia is present in only ~30-50% of primary aldosteronism cases.
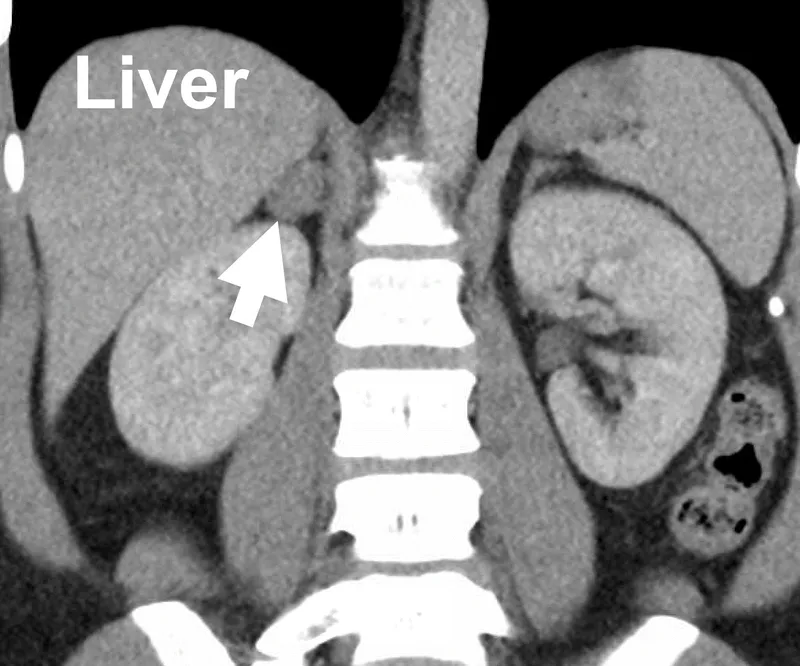
Pheochromocytoma/PGL - Adrenaline Attack
- Catecholamine-secreting tumors: Pheo (adrenal medulla), PGL (extra-adrenal).
- Classic 5 P's: Pressure (HTN), Pain (headache), Perspiration, Palpitations, Pallor.
- 📌 Rule of 10s (approximate): 10% bilateral, 10% extra-adrenal (PGL), 10% malignant, 10% familial (now ~25-40%), 10% in children.
- Diagnosis:
- Best initial: ↑ 24hr urinary fractionated metanephrines & normetanephrines; or plasma free metanephrines.
- Localization: CT/MRI; MIBG scan for PGL/metastasis.
- Management:
- Pre-op (crucial):
- Alpha-blockade (e.g., phenoxybenzamine) FIRST for 10-14 days (BP control).
- THEN Beta-blockade (e.g., propranolol) if tachycardia (⚠️ NEVER beta-blocker first).
- Saline for volume expansion.
- Surgery: Definitive.
- Pre-op (crucial):
⭐ Unopposed beta-blockade (without prior alpha-blockade) can precipitate a hypertensive crisis.

Cushing's, Thyroid & More - Diverse Disruptors
Diverse endocrine conditions beyond primary aldosteronism and pheochromocytoma cause secondary HTN. Compare key differentiating features:
| Feature | Cushing's Syndrome | Thyroid Disorders (Hyper/Hypo) | Acromegaly | CAH (11β/17α def.) |
|---|---|---|---|---|
| HTN Patho. | ↑Cortisol (MC effect), ↑SNS | Hyper: ↑CO; Hypo: ↑SVR, Na+ ret. | ↑GH/IGF-1 → Na+ ret., vol. exp. | ↑DOC (mineralocorticoid) |
| Key Clues | Striae, moon facies, central obesity | Hyper: Tachy; Hypo: Brady, fatigue | Coarse facies, big hands/feet | Virilization (11β), Ambiguous gen. (17α), HypoK+ |
| HTN Type | Systolic/Diastolic | Hyper: Systolic; Hypo: Diastolic | Systolic/Diastolic | Volume, low renin |
| Dx Tests | Dexa supp., 24h UFC, LNSC | TSH, fT3, fT4 | IGF-1, GH supp. (OGTT) | Serum DOC, 17-OHP |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | ||||
| flowchart TD |
PC["🏠 Primary Care
• Early onset HTN• Resistant HTN"]
BIS["🔬 Baseline Labs
• U+Es and TFTs• HbA1c and Lipids"]
SC["🏥 Secondary Care
• Aldosterone-Renin• Metanephrines"]
SI["🖥️ Specialist Imaging
• Adrenal CT/MRI• Pituitary MRI"]
TC["🏛️ Tertiary Care
• Venous Sampling• Genetic Testing"]
OP["💊 Management
• Adrenalectomy• Renal Angioplasty"]
PC --> BIS BIS --> SC SC --> SI SI --> TC TC --> OP
style PC fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style BIS fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style SC fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style SI fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style TC fill:#EEFAFF, stroke:#DAF3FF, stroke-width:1.5px, rx:12, ry:12, color:#0369A1 style OP fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
> ⭐ In **11β**-hydroxylase deficiency (CAH), ↑DOC leads to HTN & hypokalemia, while ↑androgens cause virilization.
## High‑Yield Points - ⚡ Biggest Takeaways
> * **Primary aldosteronism**: Most common secondary HTN; screen with **aldosterone-renin ratio (ARR)**.
> * **Pheochromocytoma**: **Episodic HTN**, palpitations, headache, sweating; test **urinary/plasma metanephrines**.
> * **Cushing's syndrome**: HTN from **cortisol excess**; screen with **24-hr UFC** or **dexamethasone suppression**.
> * **CAH**: **11β-hydroxylase** & **17α-hydroxylase deficiencies** cause HTN.
> * **Hyperthyroidism**: Causes **systolic HTN** and **widened pulse pressure**.
> * **Hypothyroidism**: May cause **diastolic HTN**.
> * Evaluate for endocrine causes in **resistant HTN** or **young hypertensives**.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

