Cushing's & Conn's - Too Much Juice!
- Cushing's Syndrome (↑Cortisol):
- Causes: Iatrogenic (commonest), Pituitary (Disease), Ectopic ACTH, Adrenal tumor.
- Sx: Central obesity, moon facies, purple striae, HTN, hyperglycemia, muscle weakness.
- Dx: Screen (24hr UFC, LDDST 1mg). ACTH: ↓ → Adrenal CT; ↑/N → HDDST (8mg)/Pituitary MRI.
⭐ LDDST fails to suppress in all Cushing's. HDDST suppresses pituitary adenomas.
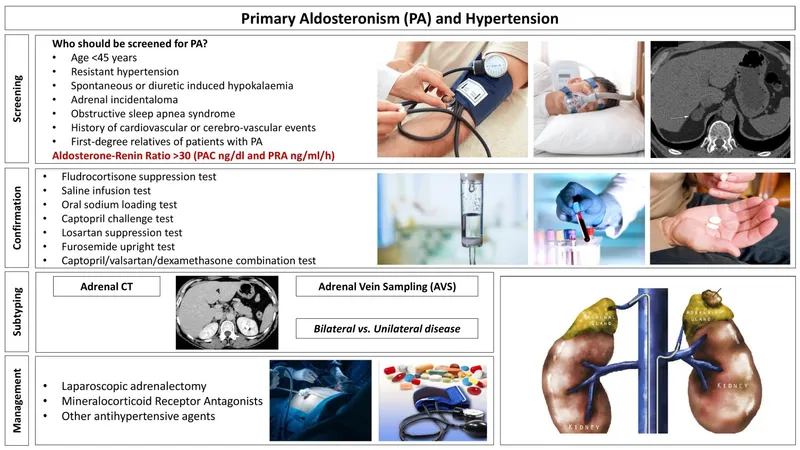
- Conn's Syndrome (↑Aldosterone):
- Causes: Adrenal adenoma, Bilateral hyperplasia.
- Sx: HTN (resistant), hypokalemia (classic, ~50% normokalemic), metabolic alkalosis. 📌 Triad: HTN, HypoK, Alkalosis.
- Dx: ↑Aldosterone-Renin Ratio (ARR >20), ↑Plasma Aldosterone (>15 ng/dL), ↓Renin. Confirm: Saline load. Localize: Adrenal CT/AVS.
- Tx: Surgery (adenoma); Spironolactone/Eplerenone (hyperplasia).
Addison's & Adrenal Crisis - Running on Empty
- Addison's Disease (Primary Adrenal Insufficiency): Chronic deficiency of cortisol ± aldosterone. Results in ↓Cortisol, ↓Aldosterone, ↑ACTH.
- Causes: Autoimmune (most common), TB, metastases, fungal infections.
- S/S: Weakness, fatigue, weight loss, orthostatic hypotension, hyperpigmentation (skin creases, buccal mucosa), salt craving, N/V/D. 📌 ADDISON: Anorexia, Dark skin, Decreased BP/Sugar/Na, Increased K+, Shock (in crisis), Orthostasis, Nausea.
- Labs: Hyponatremia, hyperkalemia, hypoglycemia, metabolic acidosis. Morning cortisol < 3 µg/dL; ACTH stimulation test (Cosyntropin): cortisol fails to rise > 18-20 µg/dL.
- Tx: Glucocorticoid (Hydrocortisone) + Mineralocorticoid (Fludrocortisone).

- Adrenal Crisis (Acute Adrenal Insufficiency): Life-threatening emergency.
- Precipitants: Stress (infection, surgery, trauma), sudden steroid withdrawal, bilateral adrenal hemorrhage (e.g., Waterhouse-Friderichsen syndrome).
- S/S: Severe hypotension/shock, fever, N/V, abdominal pain, confusion, coma.
- Tx: IV Hydrocortisone 100 mg STAT, then 50-100 mg q6-8h; aggressive IV fluids (NS/D5NS); identify & treat underlying cause.
⭐ Hyperpigmentation is characteristic of primary adrenal insufficiency (due to ↑ACTH and MSH co-secretion) but is ABSENT in secondary adrenal insufficiency (↓ACTH).
Pheochromocytoma - Catecholamine Chaos
- Tumor of chromaffin cells (adrenal medulla/extra-adrenal) secreting catecholamines (epinephrine, norepinephrine).
- Classic Triad (📌 PHE): Palpitations, Headache, Episodic sweating; also anxiety, paroxysmal/sustained hypertension.
- 📌 Rule of 10s: 10% bilateral, 10% extra-adrenal (paraganglioma), 10% malignant, 10% familial (NB: genetic predisposition now known to be higher, ~25-40%).
- Diagnosis:
- ↑ 24-hr urinary or plasma metanephrines & normetanephrines (most specific).
- CT/MRI abdomen/pelvis for localization; MIBG scan if extra-adrenal/metastatic suspected.
- Associations: MEN 2A, MEN 2B, Von Hippel-Lindau (VHL), Neurofibromatosis type 1 (NF1), SDHx gene mutations.
- Management:
- Pre-op: α-blockers (e.g., phenoxybenzamine, 10-14 days) FIRST, then β-blockers (2-3 days pre-op). Volume expansion.
- Surgical resection is definitive treatment.
⭐ Crucial Pre-op: Always initiate α-adrenergic blockade before β-blockade to prevent unopposed α-stimulation, which can precipitate a hypertensive crisis. This is a frequently tested concept!
CAH & Incidentalomas - Adrenal Oddities
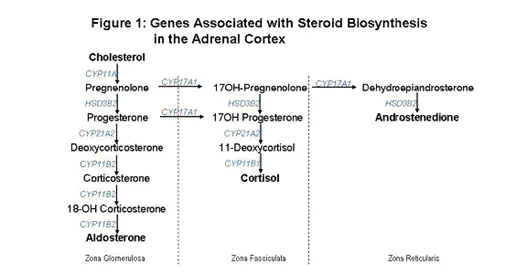
- Congenital Adrenal Hyperplasia (CAH): AR; enzyme defects in cortisol path → ↑ACTH.
- 21-Hydroxylase Deficiency (Most common, ~95%): ↓cortisol, ±↓aldo (salt-loss), ↑androgens, ↑17-OHP. Virilization, salt crisis.
- 11β-Hydroxylase Deficiency: ↓cortisol, ↑DOC (HTN), ↑androgens. ↑11-deoxycortisol.
- 17α-Hydroxylase Deficiency: ↓cortisol, ↓sex steroids, ↑mineralocorticoids (HTN). XY: ambiguous; XX: 1° amenorrhea.
- Rx: Glucocorticoids ± mineralocorticoids.
- Adrenal Incidentaloma: Mass >1 cm found incidentally.
- Workup: Hormonal (pheo, Cushing's, aldo if HTN); CT (size, HU <10 benign).
- Rx: Surgery if active, >4-6 cm, suspicious. Else, observe.
⭐ Most common CAH is 21-hydroxylase deficiency, presenting with virilization and potential salt wasting.
High‑Yield Points - ⚡ Biggest Takeaways
- Cushing's syndrome: Often exogenous steroids; dexamethasone suppression test is key for diagnosis.
- Addison's disease: Hyperpigmentation, hyponatremia, hyperkalemia; ACTH stimulation test confirms.
- Pheochromocytoma: Episodic hypertension, palpitations, headache; check urine/plasma metanephrines.
- Conn's syndrome: Primary hyperaldosteronism causing hypertension, hypokalemia, metabolic alkalosis.
- CAH (21-hydroxylase deficiency): Ambiguous genitalia (females), salt wasting crisis in neonates.
- Adrenal crisis: Life-threatening; requires immediate IV hydrocortisone and fluid resuscitation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

