RRT Fundamentals - Kidney SOS Call
- RRT: Lifesaving support for kidney failure (acute/chronic), replacing filtration.
- Goals (Kidney SOS):
- Solute clearance (uremic toxins, K⁺)
- Overload (fluid) management
- Stabilize acid-base/electrolytes
- Core Principles:
- Diffusion: Solutes move via concentration gradient.
- Convection: Solutes "dragged" with fluid.
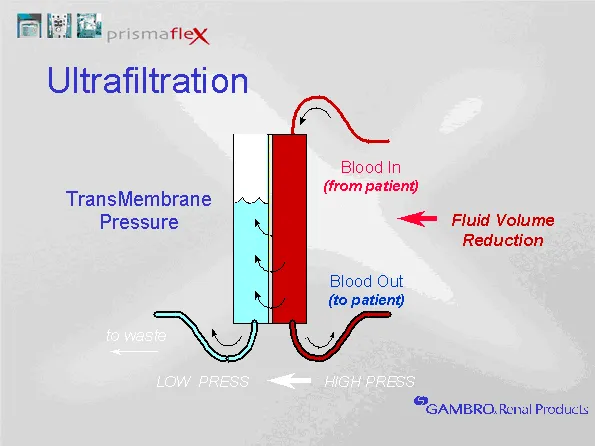
- Ultrafiltration: Fluid removal by pressure gradient.
- Indications (AEIOU 📌):
- Acidosis (severe metabolic, pH < 7.1)
- Electrolytes (refractory hyperK⁺ > 6.5 mEq/L)
- Intoxications (e.g., SLIME - Salicylates, Lithium)
- Overload (fluid, diuretic-resistant)
- Uremia (symptomatic: pericarditis, encephalopathy)
⭐ Solute removal in hemodialysis is mainly diffusion; fluid removal (ultrafiltration) by hydrostatic pressure.
 A
A
RRT Indications - Dialysis Decision Time
Deciding when to initiate Renal Replacement Therapy (RRT) is crucial. The 📌 AEIOU mnemonic is a common guide:
- Acidosis: Severe metabolic acidosis (pH < 7.1-7.2) refractory to bicarbonate therapy.
- Electrolyte abnormalities:
- Refractory hyperkalemia (K+ > 6.5 mEq/L with ECG changes or severe symptoms).
- Symptomatic hypercalcemia, severe hypermagnesemia.
- Intoxications: Dialyzable toxins (e.g., Salicylates, Lithium, Ethylene glycol, Methanol, Barbiturates - 📌 SLIME-B).
- Overload (fluid): Pulmonary edema or severe volume overload refractory to diuretics.
- Uremia: Symptomatic uremia (e.g., pericarditis, encephalopathy, intractable nausea/vomiting, uremic bleeding).
⭐ Refractory hyperkalemia (K+ > 6.5 mEq/L with ECG changes despite medical therapy) is an absolute indication for urgent RRT.
RRT Modalities - The Dialysis Menu
| Modality | Primary Mechanism | Duration | Hemodynamic Stability | Solute Clearance | Typical ICU Use |
|---|---|---|---|---|---|
| IHD | Diffusion | 3-4 hrs | ↓ (risk of hypotension) | Rapid | Stable patients, rapid toxin/K$^+$ removal |
| CRRT | Convection/Diffusion | 24 hrs | ↑ (preferred for unstable) | Slow, continuous | Hemodynamically unstable, ARDS, sepsis, TBI |
| SLEDD/PIRRT | Diffusion | 6-12 hrs | Moderate | Moderate | Alternative to CRRT; better tolerated than IHD |
- SCUF (Slow Continuous Ultrafiltration): Fluid removal only.
- CVVH (Continuous Veno-Venous Hemofiltration): Solutes by convection.
- CVVHD (Continuous Veno-Venous Hemodialysis): Solutes by diffusion.
- CVVHDF (Continuous Veno-Venous Hemodiafiltration): Convection + diffusion.
⭐ Continuous Renal Replacement Therapy (CRRT) is the preferred modality for hemodynamically unstable patients in the ICU due to its slower solute and fluid removal.
📌 Mnemonic for CRRT types (mechanism):
- SCUF: UF (UltraFiltration - fluid only)
- CVVH: Hemofiltration (convection - 'H'igh volume fluid)
- CVVHD: Dialysis (diffusion)
- CVVHDF: DiaFiltration (diffusion + filtration/convection)
RRT Complications & Anticoagulation - Clots & Calamities
- RRT Complications:
- Hypotension (most frequent; volume shifts)
- Dialysis Disequilibrium Syndrome (rapid urea ↓)
- Bleeding (anticoagulation, uremia)
- Infections (CRBSI, PD peritonitis)
- Electrolyte imbalance (↓K⁺, ↓Ca²⁺, ↓PO₄³⁻, acid-base)
- Technical: Filter clotting, air embolism, access.
- Anticoagulation: Prevents circuit clotting.
- UFH: Standard; aPTT (1.5-2.5x baseline).
- LMWH: Alternative; less monitoring; anti-Xa if needed.
- RCA: Preferred in high bleeding risk.
⭐ Regional citrate anticoagulation is effective but requires monitoring for metabolic complications such as hypocalcemia (citrate chelates calcium) and metabolic alkalosis.
- No Anticoagulation: High bleeding risk; saline flushes, high flow.
- Argatroban/Danaparoid: For HIT.
High‑Yield Points - ⚡ Biggest Takeaways
- AEIOU criteria (Acidosis, Electrolytes, Intoxication, Overload, Uremia) mandate RRT initiation.
- CRRT is preferred for hemodynamically unstable patients; IHD for rapid correction.
- Regional citrate anticoagulation is choice for CRRT; prevents filter clots.
- Key RRT complications: hypotension (esp. IHD), circuit clotting, catheter-related infections.
- Preferred vascular access: Right Internal Jugular vein for acute RRT.
- SLEDD (Sustained Low-Efficiency Daily Dialysis) balances IHD and CRRT benefits.
- Always adjust drug doses for patients on RRT.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

