EOLC Foundations - Ethi-Legal Compass
- Core Ethical Principles: Autonomy (patient choice), Beneficence (act in patient's best interest), Non-maleficence (do no harm), Justice (fair resource allocation).
- Legal Framework (India):
- Article 21 (Right to life & dignity).
- Withholding/Withdrawing life-sustaining treatment (LST) permissible if futile or per patient's wishes (Advance Medical Directive).
⭐ Passive euthanasia is legally permissible in India under strict guidelines following the Common Cause (Registered Society) vs. Union of India judgment, allowing for Advance Medical Directives.
- Key Definitions:
- Medical Futility: Intervention offers no reasonable hope of benefit.
- Brain Stem Death: Legal death; prerequisite for organ donation.
- Persistent Vegetative State (PVS): Irreversible loss of cortical function.
Communication & Decisions - Heart-to-Heart ICU
- Core Principles: Empathy, honesty, clarity, respect autonomy. Regular family conferences.
- Shared Decision-Making (SDM): Collaborative: patient/family, team.
- Discuss prognosis, options (benefits/burdens), values.
- Surrogate if patient lacks capacity.
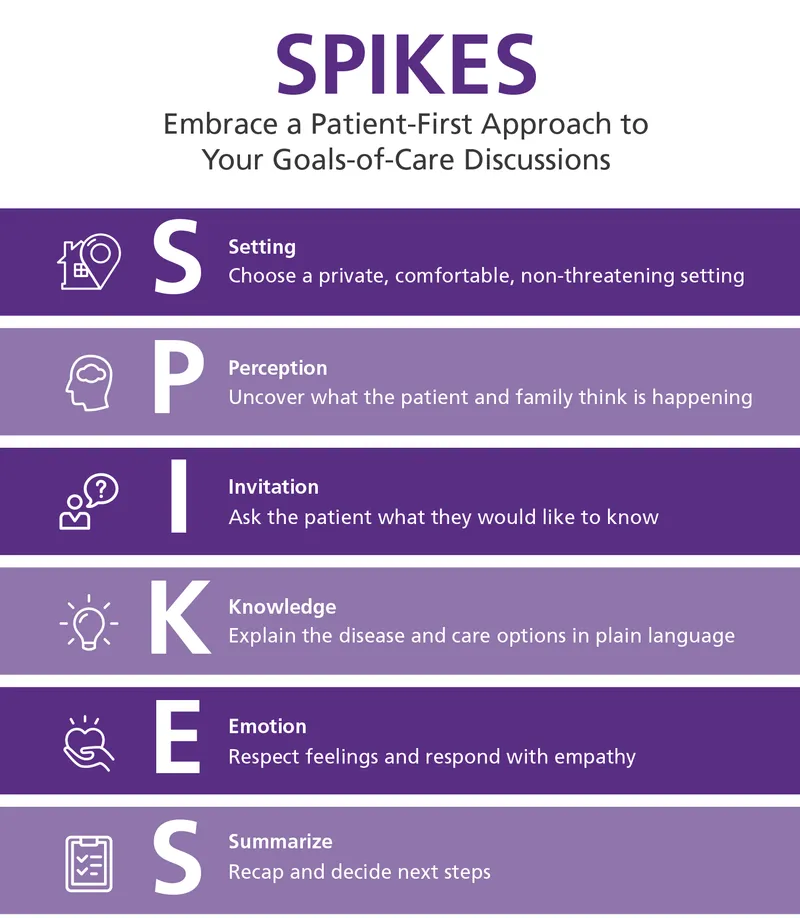
- 📌 SPIKES Protocol: For difficult conversations.
- Setting: Private, comfort.
- Perception: Gauge understanding.
- Invitation: Ask to share.
- Knowledge: Impart clearly.
- Emotions: Acknowledge.
- Strategy/Summary: Plan, summarize.
- Key Discussions:
- Goals of care (GOC): Curative, palliative, comfort.
- Code status (DNR/DNAR).
- Withholding/withdrawing treatments.
- Spiritual/cultural needs.
- Documentation: Record discussions, decisions.
⭐ The SPIKES protocol (Setting, Perception, Invitation, Knowledge, Emotions, Strategy/Summary) is a key framework for breaking bad news in EOLC.
LST & Symptom Management - Gentle Exit Strategies
- Life-Sustaining Treatment (LST) Decisions:
- Focus: Align care with patient's goals & values.
- Process: Shared decision-making, clear communication, meticulous documentation.
- Options: Withholding (not starting) or withdrawing (stopping) LST.
- Common LST: Mechanical ventilation, vasopressors, dialysis, artificial nutrition/hydration.
- Symptom Control - The Core of Comfort: 📌 "PADS" (Pain, Agitation/Anxiety, Dyspnea, Secretions)
- Pain: Opioids (e.g., Morphine 0.5-2mg IV, Fentanyl 25-50mcg IV). Titrate to effect.
- Dyspnea: Opioids (low-dose Morphine), O2 therapy, positioning, anxiolytics.
- Agitation/Delirium: Haloperidol 0.5-2mg IV/IM. Use benzodiazepines cautiously.
- Secretions ("Death Rattle"): Anticholinergics (e.g., Glycopyrrolate 0.2mg SC/IV).
- Non-pharmacological: Family presence, spiritual care, calm environment.
- Ethical Pillar:
⭐ The doctrine of double effect is crucial in EOLC, ethically permitting symptom relief (e.g., opioids for dyspnea) even if it may indirectly hasten death, provided the primary intention is palliation.
Care After Death - Lasting Respect
- Pronounce death: Document time, ensure dignified body handling.
- Remove lines/tubes (unless autopsy or organ donation indicated).
- Facilitate family viewing with privacy and empathy.
- Complete accurate death certification; adhere to medico-legal case protocols.
- Organ Donation Process:
⭐ As per the Transplantation of Human Organs and Tissues Act (THOTA), brain death certification in India requires two certifications by a specified team of doctors, with a minimum interval of 6 hours.
- Offer bereavement support to family; connect with counseling/resources.
- Support staff: Debriefing sessions for emotional well-being.
- Uphold cultural and religious sensitivities throughout.
High‑Yield Points - ⚡ Biggest Takeaways
Error generating content for this concept group: No object generated: the tool was not called.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

