Perioperative Pitfalls - Intro & Goals
- Perioperative Period Defined:
- Pre-operative: Time before surgery.
- Intra-operative: Duration of surgery.
- Post-operative: Period after surgery.
- Primary Goals:
- Identify patient-specific risks (cardiac, pulmonary, etc.).
- Optimize co-morbidities pre-surgery.
- Plan comprehensive perioperative care.
- Ensure informed consent.
- Crucially, it's about risk assessment, NOT 'medical clearance'.
- Core Components:
- Detailed history.
- Targeted physical examination.
- Investigations: Guided by H&P and anticipated surgical risk.
⭐ The primary goal of preoperative evaluation is risk stratification and optimization, not to 'clear' a patient for surgery.
Heart Hazards - Cardiac Risk Check
-
RCRI (Lee Index): 6 predictors for MACE.
- 📌 RCRI: 'CREATININE' - CAD (IHD Hx), CHF Hx, CVA/TIA Hx, Preop Creatinine >2mg/dL, Insulin for DM, High-risk Surgery.
- Risk: 0 pts: 0.4% MACE; 1 pt: 0.9%; 2 pts: 6.6%; ≥3 pts: 11%.
-
METS: Functional capacity. <4 METS (e.g., can't climb 1 flight stairs) = poor, ↑ risk.
-
ASA Physical Status Classification:
-
High-Risk Cardiac Conditions (defer elective):
- Recent MI (<30-60d), Unstable/Severe Angina.
- Decompensated HF, Sig. Arrhythmias, Severe Valvular Dz.
-
Preoperative Cardiac Evaluation Algorithm:
⭐ Continue chronic β-blockers. Avoid routine new β-blocker initiation on surgery day, esp. low/intermediate risk.
Lung Landmines - Pulmonary Perils
- Postoperative Pulmonary Complications (PPCs): Atelectasis, pneumonia, resp failure, COPD/asthma exacerbation.
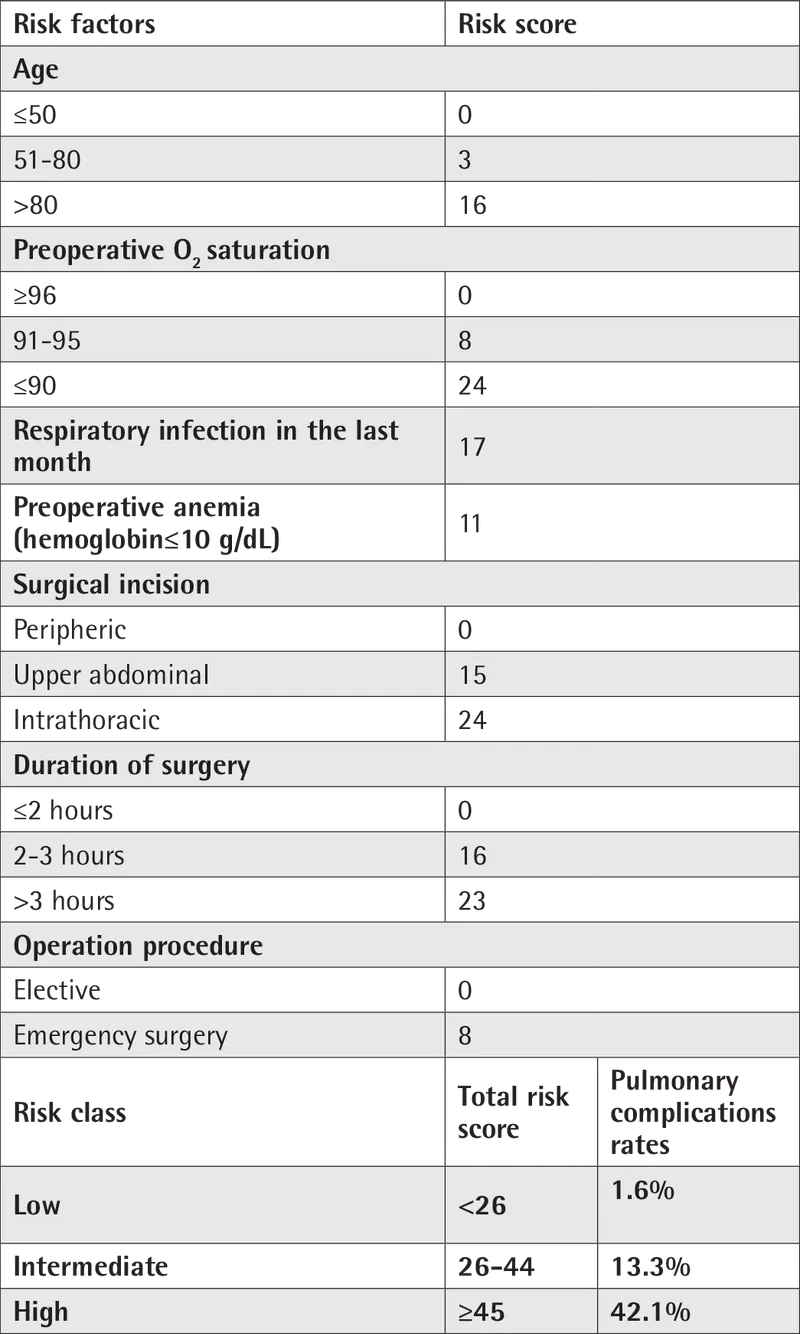
- ARISCAT Score (Assess Respiratory Risk in Surgical Patients in Catalonia):
- Components: Age, Preop SpO$₂$, Resp infection <1mo, Anemia (Hb<10 g/dL), Incision, Duration >2h, Emergency.
- Risk: Low <26, Intermediate 26-44, High ≥45.
- Patient Factors: Age >60, COPD, asthma, smoking, OSA, CHF, dependence, low albumin (<3.5 g/dL).
- Procedure Factors: Site (thorax/upper abd.), >3h surgery, GA, emergency.
- OSA: 📌 STOP-BANG: Snoring, Tired, Observed apnea, Pressure, BMI >35 kg/m², Age >50, Neck >40cm, Male. Score ≥3 high risk.
⭐ Lung protective ventilation strategies intraoperatively and early postoperative mobilization are key to reducing PPCs.
Systemic Snafus - Beyond Heart & Lungs
- Renal Risk:
- AKI predictors: CKD, eGFR <60, DM, HTN, CHF, contrast use, major surgery.
- Hepatic Risk:
- Child-Pugh Score: (Components: Encephalopathy, Ascites, Bilirubin, Albumin, PT/INR). Classes A, B, C & operative mortality.

- MELD Score: (Bilirubin, Creatinine, INR) - better for 30-day mortality.
⭐ For patients with cirrhosis, a MELD score ≥ 15 is associated with significantly increased perioperative mortality for elective non-hepatic surgery.
- Child-Pugh Score: (Components: Encephalopathy, Ascites, Bilirubin, Albumin, PT/INR). Classes A, B, C & operative mortality.
- Hematologic Risk:
- Anemia: Preop Hb <7-8 g/dL (transfusion trigger).
- VTE Risk: Caprini score for VTE prophylaxis.
- Coagulopathy: Assess INR, aPTT, platelets.
- Endocrine Risk (Diabetes):
- HbA1c target: <8% (acceptable); avoid >8.5-9%.
- Perioperative glucose control: Target 140-180 mg/dL.
- Geriatric Considerations:
- Frailty assessment, cognitive dysfunction (delirium risk), polypharmacy.
High‑Yield Points - ⚡ Biggest Takeaways
- RCRI (Revised Cardiac Risk Index) predicts MACE; components include IHD, CHF, CVA, DM (insulin), Cr >2 mg/dL, high-risk surgery.
- ASA classification strongly correlates with perioperative mortality and morbidity.
- Functional capacity <4 METs (Metabolic Equivalents) signifies poor reserve and ↑ cardiac risk.
- Key pulmonary risks: Age >60 years, COPD, active smoking, OSA, surgery duration >3 hours.
- Continue beta-blockers & statins if already prescribed; initiate cautiously in select high-risk patients.
- VTE prophylaxis (e.g., LMWH) is crucial, guided by risk scores like Caprini.
- Maintain perioperative blood glucose <180 mg/dL for optimal outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

