Postoperative Complications - Feverish Frights
Postoperative fever (>38°C or 100.4°F) is a common concern, prompting systematic evaluation.
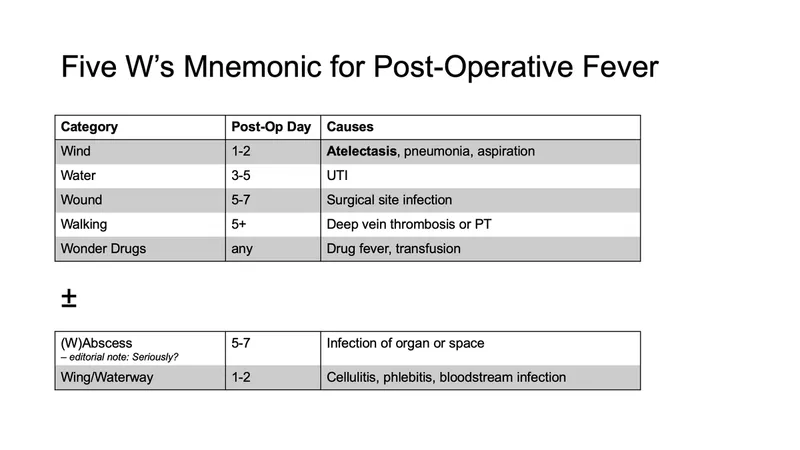
📌 5 W's of Post-Op Fever:
- Wind (Pulmonary: Atelectasis - common in first 48 hrs; Pneumonia): POD 1-2.
- Water (UTI - esp. catheterized; pyelonephritis): POD 3-5.
- Wound (SSI: Staph aureus/Strep; erythema, warmth, discharge. Deep infections later): POD 5-7.
- Walking (VTE: DVT/PE; assess risk - Virchow's, Wells score): POD >5-7.
- Wonder drugs / What did we do? (Drug fever - exclusion; transfusion rxns, line sepsis): Anytime.
⭐ Most common causes of fever by postoperative day:
- Day 1-2: Atelectasis
- Day 3-5: UTI
- Day 5-7: Wound Infection
- Day >7: DVT/PE, Abscesses
Postoperative Complications - Respiratory Riddles
- Atelectasis:
- Most common, 24-48h post-op. Fever, ↓breath sounds.
- Prevention: Incentive spirometry, deep breathing exercises, early mobilization.
⭐ Atelectasis is the most common overall postoperative complication.
- Pneumonia (HAP/VAP):
- Hospital-Acquired (HAP): >48h post-admission.
- Ventilator-Associated (VAP): >48h post-intubation.
- Symptoms: Fever, cough, purulent sputum, leukocytosis.
- Risk factors: Aspiration, prolonged ventilation, immunosuppression.
- Pulmonary Embolism (PE):
- Symptoms: Sudden dyspnea, pleuritic chest pain, tachycardia, hemoptysis.
- 📌 Virchow's Triad: Stasis, Hypercoagulability, Endothelial injury.
- Diagnosis: Wells/Geneva score, D-dimer, CT Pulmonary Angiography (CTPA - gold standard).
- Management: Anticoagulation. Prophylaxis is key (LMWH, UFH).
- ARDS (Acute Respiratory Distress Syndrome):
- Acute onset hypoxemia with bilateral pulmonary infiltrates not fully explained by cardiac failure.
- Key diagnostic criterion: $PaO_2/FiO_2$ ratio ≤300 mmHg.
- Berlin Criteria for severity (based on $PaO_2/FiO_2$ with PEEP ≥5 cmH2O):
- Mild: 201-300 mmHg
- Moderate: 101-200 mmHg
- Severe: ≤100 mmHg

Postoperative Complications - Cardiac & Clot Catastrophes
- Postoperative Myocardial Infarction (MI)
- Risk Factors: RCRI: IHD, CHF, CVA, Insulin DM, Cr >2 mg/dL, High-risk surgery.
- Diagnosis: Serial ECGs, ↑Troponins. Management: Aspirin, β-blockers, statins; consider revascularization.
⭐ Peak incidence: postoperative MI 24-72 hours.
- Venous Thromboembolism (VTE: DVT/PE)
- 📌 Virchow's Triad: Stasis, Hypercoagulability, Endothelial injury.
- Prophylaxis: Risk-stratify (Caprini). Early ambulation. Pharm: LMWH (e.g., Enoxaparin 40mg OD/30mg BID), UFH. Mech: IPC, GCS.
- Diagnosis: Wells score, D-dimer. US Doppler (DVT); CTPA (PE).
- Postoperative Arrhythmias
- Atrial Fibrillation (AFib): Most common.
- Triggers: Hypoxia, electrolytes (K⁺↓, Mg²⁺↓), pain, sepsis, cardiac surgery.
- Management: Rate/rhythm control; anticoagulation if persistent/high CHADS₂-VASc.
Postoperative Complications - Gut & Gash Griefs
- Surgical Site Infection (SSI):
- Types: Superficial, Deep, Organ/Space.
- Onset: 5-7 days. Prophylaxis: antibiotics, asepsis.
⭐ Staphylococcus aureus is the most common cause of SSIs.
- Hematoma/Seroma:
- Blood/fluid collection.
- Risk: Anticoagulants.
- Manage: Observe or Drain.
- Wound Dehiscence & Evisceration:
- Dehiscence: Fascial separation. Evisceration: Viscera protrudes (emergency!).
- Risks: ↑IAP, infection.

- Postoperative Ileus:
- Impaired GI motility; prolonged if >3-5 days.
- Causes: Opioids, bowel handling.
- Manage: NPO, NG, ambulate.
- Anastomotic Leak:
- Grave; 5-7 days post-op.
- Signs: Fever, tachycardia, pain, peritonitis, drain changes.
- 📌 LEAK: Low BP, Elevated WBC, Abdominal pain, Kindling (fever).
High‑Yield Points - ⚡ Biggest Takeaways
- Atelectasis: Most common cause of post-op fever within 48 hours ("Wind").
- UTI: Common fever source after day 3 ("Water"), especially with catheters.
- Surgical Site Infection (SSI): Presents after day 5 ("Wound"); S. aureus is the usual culprit.
- DVT/PE: Major risks; prophylaxis (e.g., LMWH, SCDs) is crucial.
- Malignant Hyperthermia: Immediate, life-threatening reaction to succinylcholine/halothane.
- Postoperative Ileus: Common after abdominal surgery; rule out obstruction if prolonged.
- Wound Dehiscence/Evisceration: Requires immediate surgical intervention.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

