Consultative and Perioperative Medicine

On this page
🎯 Perioperative Excellence: The Surgical Safety Command Center
Surgery transforms patients from stable outpatients into physiologically stressed individuals navigating anesthesia, tissue trauma, and healing-a journey where your medical expertise becomes the safety net. You'll master how to evaluate surgical candidates, optimize their physiology before incision, anticipate intraoperative crises, recognize postoperative complications early, and coordinate multidisciplinary care that bridges operating room and ward. This isn't about becoming a surgeon; it's about becoming the internist who ensures patients survive and thrive through one of medicine's highest-risk intervals.
📌 Remember: PERIOP - Preoperative assessment, Endocrine management, Respiratory optimization, Infection prophylaxis, Optimal recovery, Postoperative monitoring
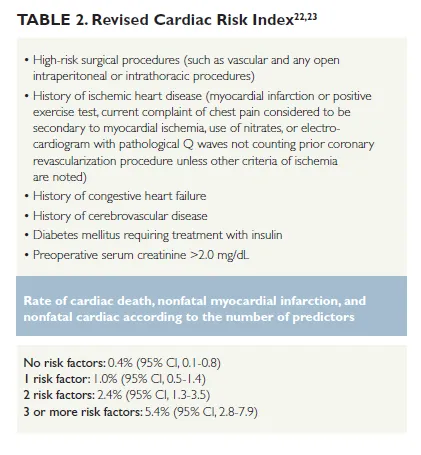
The foundation of perioperative excellence rests on systematic risk assessment and evidence-based interventions. Lee's Revised Cardiac Risk Index identifies 6 major predictors with each factor increasing cardiac event risk by 0.4-0.9%. Patients with ≥3 risk factors face >9% cardiac complication rates, demanding intensive perioperative optimization.
| Risk Assessment Tool | Validation Population | Predictive Accuracy | Clinical Application | Threshold Values |
|---|---|---|---|---|
| Lee's RCRI | 4,315 patients | C-statistic 0.81 | Cardiac risk stratification | ≥3 factors = high risk |
| ARISCAT Score | 2,464 patients | AUC 0.88 | Pulmonary complications | >44 points = high risk |
| Caprini Score | 8,216 patients | Sensitivity 88% | VTE risk assessment | ≥5 points = high risk |
| FRAX Calculator | 250,000 patients | Specificity 90% | Fracture risk prediction | >20% major fracture risk |
| ASA Physical Status | Universal application | Inter-rater κ=0.56 | Perioperative mortality | ASA ≥4 = high mortality |
- Low Risk (0-1 RCRI factors): <1% cardiac event rate
- Intermediate Risk (2 RCRI factors): 1-5% cardiac event rate
- High Risk (≥3 RCRI factors): >5% cardiac event rate
- Requires cardiology consultation for intermediate-high risk surgery
- Consider stress testing if results change management
- Beta-blocker optimization reduces events by 13-17%
⭐ Clinical Pearl: Patients with active cardiac conditions (unstable angina, decompensated heart failure, significant arrhythmias) require immediate cardiology consultation and surgery delay until optimization. Emergency surgery proceeds with intensive monitoring regardless of cardiac status.
💡 Master This: Functional capacity <4 METs (inability to climb 2 flights of stairs) predicts 2-3x higher perioperative cardiac complications. This simple assessment guides the need for formal cardiac evaluation in intermediate-risk patients.
Understanding perioperative risk assessment creates the foundation for developing comprehensive optimization strategies that reduce morbidity and mortality across surgical populations.
🎯 Perioperative Excellence: The Surgical Safety Command Center
🔧 Physiological Optimization: The Preoperative Tuning Protocol
📌 Remember: OPTIMIZE - Oxygen delivery, Pulmonary function, Thrombosis prevention, Infection control, Medication management, Immune status, Zinc/nutrition, Endocrine balance
Cardiovascular Optimization Framework:
- Hypertension Management
- Target <140/90 mmHg for most patients
- <130/80 mmHg for diabetes/CKD patients
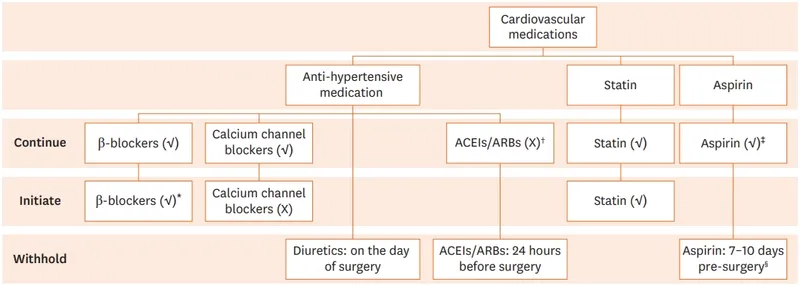
- ACE inhibitors held 24 hours before surgery
- Beta-blockers continued perioperatively if chronic therapy
- Metoprolol 25-100mg BID reduces cardiac events by 15%
- Atenolol 50-100mg daily provides 24-hour coverage
| Optimization Target | Intervention | Timeline Required | Success Rate | Complication Reduction |
|---|---|---|---|---|
| Smoking Cessation | Counseling + NRT | 8+ weeks optimal | 15-20% quit rate | 23-41% pulmonary complications |
| Anemia Correction | Iron/EPO therapy | 4-6 weeks | 85% achieve Hgb >10 | 39% transfusion reduction |
| Diabetes Control | Insulin optimization | 2-3 months | 70% achieve HbA1c <8% | 30% infection reduction |
| Heart Failure | Diuretic/ACE optimization | 4-6 weeks | 60% symptom improvement | 25% cardiac events |
| COPD Management | Bronchodilator/steroid | 2-4 weeks | 40% FEV1 improvement | 35% respiratory complications |
- Incentive spirometry training reduces atelectasis by 50%
- Bronchodilator therapy for FEV1 <80% predicted
- Systemic steroids for COPD exacerbation within 2 weeks
- Prednisolone 30-40mg daily × 5-7 days
- Inhaled budesonide 400-800mcg BID for maintenance
⭐ Clinical Pearl: Preoperative anemia (Hgb <12 g/dL women, <13 g/dL men) increases 30-day mortality by 42% and LOS by 0.5-1.5 days. Iron deficiency accounts for >50% of surgical anemia and responds to IV iron within 2-4 weeks.
💡 Master This: Enhanced Recovery After Surgery (ERAS) protocols incorporating preoperative carbohydrate loading, goal-directed fluid therapy, and multimodal analgesia reduce LOS by 1-4 days and complications by 30-50% across surgical specialties.
Systematic preoperative optimization establishes the physiological foundation for successful surgical outcomes, connecting directly to intraoperative management strategies.
🔧 Physiological Optimization: The Preoperative Tuning Protocol
🎪 Intraoperative Orchestration: The Surgical Theater Command
Hemodynamic Management Protocols:
- Fluid Responsiveness Assessment
- Pulse pressure variation >13% predicts fluid responsiveness
- Stroke volume variation >10% indicates preload dependence
- Passive leg raise increases CO >10% in fluid responders
- 250-500mL crystalloid boluses for responders
- Vasopressor support for non-responders with hypotension
📌 Remember: MONITOR - Mean arterial pressure >65mmHg, Oxygen delivery optimization, Neuromuscular blockade reversal, Intraoperative glucose <180mg/dL, Temperature >36°C, Output monitoring, Respiratory protection
| Monitoring Parameter | Target Range | Intervention Threshold | Clinical Significance | Adjustment Strategy |
|---|---|---|---|---|
| Mean Arterial Pressure | 65-100 mmHg | <65 or >100 mmHg | Organ perfusion pressure | Fluid/vasopressor titration |
| Stroke Volume Index | 35-65 mL/m² | <35 mL/m² | Cardiac output optimization | Preload/contractility support |
| Oxygen Delivery | >500 mL/min/m² | <400 mL/min/m² | Tissue oxygenation | Hemoglobin/cardiac output |
| Central Venous Pressure | 8-12 mmHg | <8 or >15 mmHg | Volume status assessment | Fluid management guidance |
| Lactate Level | <2 mmol/L | >4 mmol/L | Tissue hypoperfusion | Resuscitation intensification |
- Minimum Alveolar Concentration (MAC) decreases 6% per decade after age 40
- Propofol 1-2mg/kg induction with 4-12mg/kg/hr maintenance
- Sevoflurane 0.5-2 MAC provides organ protection benefits
- Myocardial conditioning reduces troponin elevation by 40%
- Neuroprotective effects in cerebral surgery
⭐ Clinical Pearl: Intraoperative hypothermia (<36°C) increases surgical site infections by 200%, bleeding by 16%, and cardiac events by 55%. Forced-air warming and warmed IV fluids maintain normothermia in >90% of patients.
💡 Master This: Neuromuscular blockade reversal with sugammadex 2-4mg/kg provides complete reversal within 2-3 minutes compared to neostigmine requiring 10-15 minutes. Residual paralysis (TOF ratio <0.9) occurs in 30-60% of patients with conventional reversal.
Intraoperative optimization creates the foundation for smooth emergence and transition to postoperative care, where early recognition and management of complications becomes paramount.
🎪 Intraoperative Orchestration: The Surgical Theater Command
🔍 Complication Recognition: The Early Warning System
Cardiovascular Complication Patterns:
- Myocardial Infarction Recognition
- Troponin elevation >0.03 ng/mL within 48 hours postoperatively
- >50% patients present without chest pain (silent MI)
- ECG changes occur in only 25-50% of perioperative MI
- New Q waves indicate transmural infarction
- ST depression >1mm suggests subendocardial ischemia
- T-wave inversions may be delayed 24-72 hours
📌 Remember: FAILURE - Fever patterns, Arrhythmia detection, Infection signs, Lung complications, Urinary issues, Renal dysfunction, Emergent bleeding
| Complication Type | Incidence Rate | Early Warning Signs | Detection Timeline | Mortality Impact |
|---|---|---|---|---|
| Pulmonary Embolism | 0.1-0.8% | Tachycardia, hypoxemia, chest pain | 24-72 hours | 25-30% if untreated |
| Myocardial Infarction | 1-5% | Troponin elevation, ECG changes | 24-48 hours | 15-25% mortality |
| Pneumonia | 2-40% | Fever, leukocytosis, infiltrates | 48-96 hours | 20-50% in high-risk |
| Anastomotic Leak | 1-15% | Fever, tachycardia, abdominal pain | 3-7 days | 10-25% mortality |
| Acute Kidney Injury | 5-15% | Creatinine rise, oliguria | 24-72 hours | 2-5x mortality risk |
- Pneumonia develops in 2-40% depending on surgery type
- Atelectasis affects >90% of patients within 24 hours
- Pulmonary embolism peaks at 48-72 hours postoperatively
- Wells Score >4 indicates high probability
- D-dimer >500 ng/mL has 95% sensitivity but low specificity
- CTPA remains gold standard for diagnosis
⭐ Clinical Pearl: Postoperative fever within 48 hours is non-infectious in >80% of cases, typically representing inflammatory response or atelectasis. Fever >48 hours postoperatively suggests infectious etiology requiring systematic evaluation including blood cultures, urinalysis, and chest imaging.
💡 Master This: Anastomotic leak presents with subtle signs including unexplained tachycardia, low-grade fever, and abdominal discomfort before overt peritonitis develops. C-reactive protein >150 mg/L on postoperative day 3-5 suggests anastomotic complications with 75% sensitivity.
Systematic complication recognition enables rapid intervention and improved outcomes, connecting directly to evidence-based treatment algorithms and management protocols.
🔍 Complication Recognition: The Early Warning System
⚖️ Treatment Algorithms: The Evidence-Based Response Matrix
Cardiac Complication Management:
- Perioperative Myocardial Infarction Protocol
- Dual antiplatelet therapy unless high bleeding risk
- Atorvastatin 80mg daily reduces recurrent events by 25%
- Beta-blocker optimization to HR 60-70 bpm
- Metoprolol 25-100mg BID titrated to heart rate response
- Carvedilol 3.125-25mg BID for heart failure patients
- Avoid beta-blockers if hemodynamically unstable
📌 Remember: RESPOND - Recognize early, Escalate appropriately, Systematic assessment, Protocol-driven care, Outcome monitoring, Notify consultants, Document thoroughly
| Complication | First-Line Treatment | Response Timeline | Success Rate | Escalation Criteria |
|---|---|---|---|---|
| Sepsis/Septic Shock | Antibiotics + fluid resuscitation | 1-hour bundle | 70-80% survival | Persistent hypotension >6 hours |
| Pulmonary Embolism | Anticoagulation/thrombolysis | 24-48 hours | 85-95% survival | Hemodynamic instability |
| Acute MI | Dual antiplatelet + statin | 12-24 hours | 80-90% survival | Cardiogenic shock |
| Pneumonia | Targeted antibiotics | 48-72 hours | 75-85% resolution | Respiratory failure |
| Anastomotic Leak | Conservative vs surgical | 24-72 hours | 60-80% success | Peritonitis/sepsis |
- High-flow nasal cannula at 30-60 L/min reduces intubation by 25%
- Non-invasive ventilation for COPD exacerbations and cardiogenic edema
- Lung-protective ventilation with tidal volumes 6-8 mL/kg predicted body weight
- PEEP 5-15 cmH2O to maintain FiO2 <60%
- Plateau pressure <30 cmH2O prevents ventilator-induced lung injury
⭐ Clinical Pearl: Antibiotic de-escalation within 48-72 hours based on culture results and clinical improvement reduces C. difficile infections by 50% and antimicrobial resistance without compromising treatment efficacy. Procalcitonin <0.25 ng/mL supports antibiotic discontinuation.
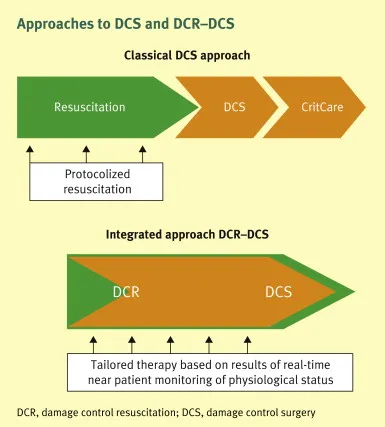
💡 Master This: Damage control surgery principles apply to critically ill patients with multiple organ dysfunction. Abbreviated procedures focusing on hemorrhage control and contamination source control followed by ICU optimization improve survival by 15-25% compared to definitive surgery in unstable patients.
Evidence-based treatment algorithms provide the framework for optimal complication management, leading to comprehensive recovery optimization and long-term outcome improvement.
⚖️ Treatment Algorithms: The Evidence-Based Response Matrix
🔗 System Integration: The Multidisciplinary Care Network
Care Coordination Framework:
- Preoperative Optimization Clinics
- Anesthesiology-led assessment 2-4 weeks before surgery
- Risk stratification and optimization protocols reduce cancellations by 50%
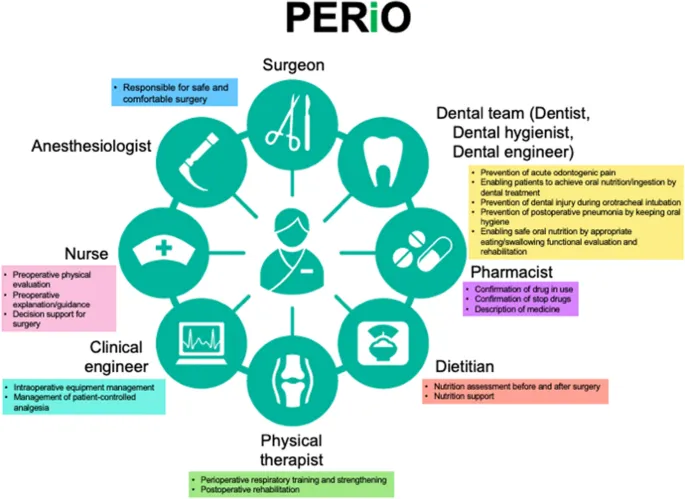
- Multidisciplinary planning includes surgery, anesthesia, nursing, and pharmacy
- Medication reconciliation prevents 75% of drug-related errors
- Patient education improves compliance by 40-60%
- Shared decision-making enhances satisfaction scores by 25%
📌 Remember: INTEGRATE - Interdisciplinary rounds, Nursing communication, Transition planning, Electronic coordination, Goal alignment, Risk sharing, Accountability measures, Team huddles, Evaluation metrics
| Integration Component | Implementation Strategy | Outcome Improvement | Cost Impact | Quality Metrics |
|---|---|---|---|---|
| Surgical Home Model | Shared accountability | 20-30% complication reduction | 10-20% cost savings | Patient satisfaction >90% |
| Enhanced Recovery | Standardized protocols | 1-4 day LOS reduction | $2000-5000 per case | 30-50% complication reduction |
| Rapid Response Teams | 24/7 availability | 40% failure-to-rescue reduction | ICU utilization optimization | Response time <15 minutes |
| Medication Reconciliation | Pharmacist involvement | 75% error prevention | Adverse event reduction | 95% accuracy target |
| Discharge Planning | Case management | 15-25% readmission reduction | $3000-8000 savings | 48-hour follow-up >80% |
- Real-time dashboards track >20 quality metrics continuously
- Morbidity and mortality conferences drive systematic improvements
- Root cause analysis for adverse events prevents recurrence by 60-80%
- Plan-Do-Study-Act cycles enable rapid improvement
- Benchmarking against national databases identifies improvement opportunities
- Physician feedback with peer comparison improves performance by 15-25%
⭐ Clinical Pearl: Perioperative handoffs represent high-risk transitions with communication failures contributing to 65% of sentinel events. Structured handoff protocols using SBAR format (Situation, Background, Assessment, Recommendation) reduce information loss by 80% and improve safety outcomes.
💡 Master This: Value-based care models in perioperative medicine align financial incentives with quality outcomes, creating shared savings of $1000-3000 per case while improving patient satisfaction, reducing complications, and optimizing resource utilization across the surgical episode.
Comprehensive system integration establishes the foundation for sustainable perioperative excellence, connecting all care elements into a cohesive framework for optimal surgical outcomes.
🔗 System Integration: The Multidisciplinary Care Network
🎯 Mastery Arsenal: The Perioperative Command Toolkit
Essential Clinical Thresholds:
- Cardiac Risk Stratification: RCRI ≥3 = high risk requiring optimization
- Pulmonary Risk: ARISCAT >44 points predicts respiratory complications
- VTE Prophylaxis: Caprini ≥5 mandates pharmacologic prevention
- Hemodynamic Targets: MAP ≥65 mmHg, SVV <13%, lactate <2 mmol/L
- Temperature Management: Core temperature ≥36°C prevents complications
📌 Remember: MASTERY - Metrics monitoring, Algorithm execution, System thinking, Team coordination, Evidence application, Risk mitigation, Yield optimization
| Clinical Scenario | Rapid Assessment | Key Intervention | Success Metric | Escalation Trigger |
|---|---|---|---|---|
| Preoperative Optimization | RCRI + functional capacity | Risk-specific protocols | Complication reduction >20% | Uncontrolled risk factors |
| Intraoperative Management | GDFT + organ protection | Hemodynamic optimization | Stable vital signs | Persistent instability |
| Complication Recognition | MEWS + systematic surveillance | Early intervention protocols | Rapid response <30 min | Clinical deterioration |
| Recovery Optimization | ERAS + discharge criteria | Multimodal approach | LOS reduction 1-4 days | Delayed milestones |
💡 Master This: Continuous quality improvement in perioperative care combines real-time monitoring, outcome tracking, and systematic feedback to achieve sustained excellence. High-performing programs demonstrate mortality rates <1%, complication rates <10%, and patient satisfaction >95% through integrated care delivery and shared accountability.
🎯 Mastery Arsenal: The Perioperative Command Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























